Uvic thesis template
The Reconstructionof Pharmacist Authority
in British Columbia: 1965-1968
B.Sc (Pharm), University of British Columbia, 1974 A Thesis Submitted in Partial Fulfillment of the Requirements for the Degree of in the Department of History Stephen Dove, 2010 University of Victoria All rights reserved. This thesis may not be reproduced in whole or in part, by photocopy or other means, without the permission of the author. Supervisory Committee
The Reconstruction
of Pharmacist Authority
in British Columbia: 1965-1968
B. Sc. (Pharm), University of British Columbia, 1974 Supervisory Committee
Dr. Mitchell Lewis Hammond, (Department of History)
Supervisor
Dr. John Lutz, (Department of History)
Departmental Member
Dr. Eike-Henner Kluge, (Department of Philosophy)
Outside Member
Abstract
Supervisory Committee
Dr. Mitchell Lewis Hammond, (Department of History)
Supervisor
Dr. John Lutz, (Department of History)
Departmental Member
Dr. Eike-Henner Kluge, (Department of Philosophy)
Outside Member
Despite extensive research on the history of medicine, little has been written on the role played by pharmacists. The diminished demand for compounding services that accompanied the explosion of manufactured pharmaceuticals after World War II left pharmacists over educated and underutilized. This study demonstrates how British Columbia pharmacists reconstructed their professional authority in the 1960s through the formation of a Pharmacy Planning Commission, a process that pre-dated and influenced other jurisdictions. Examination of the archives of the College of Pharmacists of British Columbia reveals that pharmacists overcame ethical restrictions, adopted clinically focussed education and increased accessibility to facilitate a role as consultant to the public on non-prescription medications. The addition of prescription drug counselling and an increased role as drug consultants to physicians allowed British Columbia pharmacists the authority to claim a core competency as drug information experts. Table of Contents
Introduction . 1 Chapter 1 . 16 Chapter 2 . 37 Chapter 3 . 48 Chapter 4 . 72 Conclusion . 83 I would like to acknowledge the help and guidance provided by my supervisor, Dr. Mitchell Lewis Hammond. Additionally, I am grateful to both additional members of my committee, Dr. Eike-Henner Kluge and Dr. John Lutz. Your help was greatly appreciated. I would also like to acknowledge all of the History Department instructors who have helped guide a student with a background in science and business into the world of humanities. My wife, Frances Dove, deserves all the credit in the world for reading my work over the past four years and enhancing the clarity of my writing. She has learned more about pharmacy history than she ever expected, or desired.

Dedication
This thesis is dedicated to Mr. Gibb Henderson, Executive Secretary of the
Pharmaceutical Association of British Columbia, who had the foresight to recognize the
importance that the records of the Association would be to future pharmacists and
historians. He was responsible for saving the Association records from 1891 to 1982,
some by storing them in his own basement. They are now kept in the Special Collections
Division of the University of British Columbia library. As you can judge by the note
below, not everyone shared the vision he had about the value of these records. The note
was found in one of the documents that he saved.
The issues at stake in the history of medicine – how societies organize health care, how individuals or states relate to sickness, how we understand our own identity and agency as sufferers or healers – are simply too important for the practice of medical history not to be persistently subjected to vigorous reflection and re-examination.1
Frank Huisman, Medical Historian
The community pharmacist occupies a unique position within the medical
community and society. Educated in Canada with a five-year university degree,
including extensive medical, biological and physical sciences, the community
pharmacist's professional work setting situates them in a unique position. They usually
practice their profession within the commercial retail sector, rather than within the
confines of an office or hospital setting like most health practitioners. Their location in
commercial areas, in combination with the large number of pharmacies in our society,
has made pharmacists the most easily accessible health professional. The public takes
advantage of this accessibility by often making the pharmacist their first contact with the
health care system. The pharmacist may respond with simple advice, over-the-counter
treatments or, if warranted, referral to another health professional. Thus, part of the
pharmacist's role resembles that of a triage nurse in the hospital setting.
While accessibility has been mutually convenient and beneficial for the public and
pharmacists, it has also affected the public's view of pharmacists as health professionals.
For much of the twentieth century, pharmacists were unable to support themselves with
income derived solely from the professional services they offered. As a result, they have
1 Frank Huisman, "Medical Histories," in Locating Medical History: The Stories and Their Meanings, ed. Frank Huisman and John Harley Warner (Baltimore: The Johns Hopkins University Press, 2004), 3.
supplemented their income with a variety of non-professional commercial services and
products, ranging from minimal offerings in clinic pharmacies to broad arrays of services
and products in mass merchandise locations. The public expects non-professional
products to be available in a pharmacy, alongside professional services. This
combination of a professional and commercial role left pharmacists struggling, for much
of the twentieth century, to attain recognition as a complete profession; from the public,
other health professionals and even within their own profession. In this thesis, I will
examine how community pharmacists in British Columbia, in the mid 1960s,
reconstructed their professional foundations in an attempt to enhance their professional
image. To achieve this goal, pharmacists had to break away from the ethical and legal
constraints that had restricted the scope of their practice, since the 1920s.
The definition of a profession is socially constructed. Consequently, those groups
recognized as professions vary in each society. At the beginning of the nineteenth
century, the only recognized professions in western society were medicine, law and the
clergy. These groups acquired legitimacy as professionals through a classical education
which was requisite to their status as gentlemen. The classics endowed the professional
with the qualities of character and culture which, in turn, conferred authority upon their
expertise. This requirement ensured that the professions would be restricted to those
members of society from the upper end of the economic scale since university was
beyond the financial resources of the majority of the public. If they possessed these
basics, professionals could develop the specific skills they needed through
apprenticeships with experienced members of their profession.2
2 R. Gidney and W. Millar, Professional Gentlemen: The Professions in Nineteenth-Century Ontario
(Toronto: University of Toronto Press, 1994), 5.
Since the mid-nineteenth century, professions in Canada have gained recognition
by legal statute in addition to social recognition. Typically, when the state recognizes a
profession it allows them to control their membership, education and discipline through
self-regulating statutory professional associations. In Canada, the Ontario College of
Pharmacy was recognized in 1871 by The Pharmacy Act.3 British Columbia pharmacists
received self-regulatory status with the passage of the British Columbia Pharmacy Act in
1891.4 While legal sanction is a prerequisite to recognition as a profession, academics
have devoted considerable effort to defining the attributes that separate professions from
other occupations.
Sociologist Talcott Parson defined professionals as possessing several
characteristics. They are recruited and licensed, he argued, based on technical merits and
use generally accepted scientific principles. Additionally, they restrict their work to their
technical competences and put their client's interests first, avoiding emotional
involvement in order to retain objectivity.5 Sociologist Eliot Freidson agrees with
Parsons but points out that these characteristics could apply to other occupations as well.
Freidson defines professionalism as the occupational control of work and, like most
occupations, professions perform specialized functions."6 Unlike mechanical
specialization, which includes a small number of simple, invariant, repetitive actions,
professions demonstrate theoretically based discretionary specialization. These tasks are
so varied that the professional must exercise considerable discretion in adapting their
3 R. J. Clark, "Professional Aspirations and the Limits of Occupational Autonomy: The Case of Pharmacy in
Nineteenth-Century Ontario." Canadian Bulletin of Medical History Vol. 8 (1991): 44.
4 Arnold Raison, A Brief History of Pharmacy in Canada (Canadian Pharmaceutical Association, 1967), 46.
5 Talcott Parsons, The Social System (London: Tavistock Publications Limited, 1952), 434-5.
6 Eliot Freidson, "Theory of Professionalism: Method and Substance," International Review of Social and
Behavioural Sciences Vol. 9 No. 1 (1999):118.
knowledge and skills to each circumstance encountered.7 Professional authority derives
from specialized knowledge as well as legal statute.8 What Freidson adds to Parson is the
recognition that complex judgment brings the dimension of risk, either success or failure,
to the professional.9
When a profession is privileged with occupational control they are afforded
certain monopolies. Freidson argues that these monopolies imply that the problems that
professions deal with are too complex for the public to make choices that are in their own
best interest. This restriction creates the possibility of exploitation and consequently
professions are held to have a fiduciary role in protecting the interests of the public.
Professions instil a aura of trust in the public through the adoption of Codes of Ethics and
the formation of intra-professional disciplinary committees. In addition, professions
make a claim to independence from either political or client control. This manifests
itself, Freidson argues, in allegiance to a transcendent value of truth, beauty,
enlightenment, justice, salvation, health or prosperity and enforces the professions claim
to special status.10 In short, professionals are expected to value the interests of the public
over their own self interest.
It is important to keep in mind, when looking at the characteristics of a profession
that professions cannot be established and maintained without powers they do not
possess. Freidson has pointed out that knowledge and skill might give professions human
7 Freidson, "Theory of Professionalism," 119.
8 Eliot Freidson, Professional Dominance: The Social Structure of Medical Care (New York: Atherton Press
Inc, 1970): 108.
10 Freidson, "Theory of Professionalism," 127.
and cultural capital but not economic or political capital. Only the state has the power to
establish and maintain professionalism.11
Other academics have examined the development of professions as well.
Economist Deborah Anne Savage defines a profession as "a network of strategic alliances
across ownership boundaries among practitioners who share a core competence." 12 This
definition lacks many of the accepted elements that define a profession but is useful
because it introduces the concept of core competences which reflect a professions
knowledge and skill. For Freidson these competencies constitute a knowledge mandate
that "represents the capacity of a profession to exercise influence by virtue of its body of
knowledge and skill."13 In pharmacist's struggle to gain and maintain their professional
status, core competencies, representing their knowledge mandate, would play a vital role.
Savage and Freidson's work can provide a valuable framework for evaluating
pharmacists' professional progress. Savage defines competencies as the collective
learning of an organization and distinctive competencies are those that an organization
can perform better than anyone else. Core competencies are those that are crucial to an
organization's survival and play an important role in defining professions as knowledge-
reliant production organizations. Capabilities are activities that an organization can
perform with a set of competencies. Dynamic capability is defined as the organization's
"ability to integrate, build, and reconfigure internal and external competencies to address
rapidly changing environments." Dynamic capabilities and competencies can explain
how a profession develops, and adapts itself, in response to changes in its external and
11 Freidson, "Theory of Professionalism," 123. 12 Deborah Anne Savage, "The Professions in Theory and History: The Case of Pharmacy," Business and Economic History Vol. 23 No. 2 (Winter 1994): 131. 13 Freidson, "Theory of Professionalism," 127.
internal competitive environment. For Freidson, the strength of a professions capacity is
measured by its knowledge and skill – the depth of its scientific foundation - , its sphere
of authority – its technical, moral and cultural authority, and its institutional spheres – the
legal environment where it practices.14
In Canada, pharmacists have been legally designated as professionals since the
nineteenth century. Their struggles have been with the additional aspects of
professionalism outlined in the preceding discussion. What makes pharmacy an
important profession to examine is that they significantly adjusted their core
competencies, the expression of their knowledge and skill, over the course of the
twentieth century. Additionally, as their core competencies shifted, their sphere of
authority, technically, morally and culturally, also adjusted.
The application of power and authority is integral to any discussion about
professions. Paul Starr argues, in The Social Transformation of American Medicine, that
the authority of medical practitioners incorporates two effective forms of control,
legitimacy and dependence.15 Practitioners, he says, are able to exercise legitimacy
through social acceptance of their specialized knowledge and competence. Dependence
results from the expected negative consequences that might befall a patient if they choose
not to accept the practitioner's authority. Backing up authority is an implied threat of
coercion provided by either force or persuasion. Some authorities, such as police and the
armed forces, routinely use force to back up society's collective authority. Medical
practitioners generally back up their authority with persuasion although society has
delegated physicians the authority to use force in certain situations. Physicians are able
14 Freidson, "Theory of Professionalism," 127. 15 Paul Starr, The Social Transformation of American Medicine (New York: Basic Books Inc, 1982), 9-29.
to order involuntary confinement of mentally ill patients who are a threat to themselves or
society for 48 hours.16 More commonly, a health practitioner's authority derives from the
patient's dependence on their specialized knowledge along with their statutory powers.
In order to protect the public from potential abuse of authority, professions develop codes
Ethical codes are put in place when a profession acquires sufficient specialized
training and knowledge to justify society delegating to them the authority to make
informed decisions. Along with this authority comes the responsibility and
accountability to use their expert knowledge for the benefit of their client. These ethical
codes ensure that the power and authority vested in the profession are used in society's
best interest. Ethical codes can be developed in a number of ways. They can represent
an ethical consensus among the members of the profession while not necessarily taking
society's needs into consideration. A second route creates codes that outline the
profession's judicial position. This type of code is useful for disputes that end up in the
courts but doesn't address the "grey" issues that arise just outside of legislation. Third,
codes can serve as statements of role-specific rules that are unique to the profession but
differ from those that govern society as a whole.17
A fourth method is similar to the third, with the exception that codes are created
by adapting ethical principles that apply to society in general, to activities that are
specific for the profession. Philosopher Eike-Henner Kluge argues that since the process
that a profession uses to select its members is constructed by society, it follows logically
that its members should be held to the same ethical principles as that society. On that
16 British Columbia Mental Health Act, 1996, Part 3 Section 22. 17 Eike-Henner W. Kluge, Biomedical Ethics: In a Canadian Context (Scarborough: Prentice-Hall Inc, 1992), 46-53.
basis, the last method of constructing codes of ethics would most appropriately provide
guidance to the profession on their responsibilities to society.18 Codes of ethics created
using the fourth method reflect the ethical principles of the society in which it was
created, as well as the profession that created them.
Codes of ethics can be created accessing several different models. The model that
a profession chooses defines the type of relationship that it wishes to have with the
society they serve. One alternative, the paternalistic or priestly model, allows the
professional to make decisions on behalf of their client. When this model is used in
medicine, the patient has very little input into their diagnosis and treatment. It follows
that they need to be given very little information about their diagnosis or treatment
because they are not part of the decision making process. This model is familiar in
medicine and leaves the patient with the role of obeying "doctor's orders" or "following
the instructions on your prescription."
A second alternative is the "agency" model which embodies the opposite
characteristics to the paternalistic model. In this model the client is in complete control
and the professional is used only for technical consultation. Unlike the paternalistic
model, this patient needs as much information as possible, preferably as much as the
health professional, because they are ultimately responsible for determining their own
diagnosis and treatment. With complete control reverting to the patient, the health
practitioner is obligated to provide a treatment, even if its effectiveness is doubtful or
contrary to his or her better judgment.
One last possibility is the fiduciary model, which implies that a relationship of
trust exists between the professional and the client, even though their knowledge is not on 18 Ibid., 46-53.
an equal footing. In this model, the ethical values of the health practitioner would be
balanced by the values expressed by the patient. A patient in this model would have to
receive enough information about the diagnosis and treatment to allow them to make an
informed decision on the risks versus the benefits of the treatment. Variations of these
three models have been employed at different times by health practitioners at different
times in history, in different societies.
Ethical codes have played an important role in pharmacists' development. They
have been used effectively to control the professional activities of pharmacists, in times
when pharmacists needed to consolidate their core competencies. Conversely, they have
acted as a brake on professional progress in times when pharmacists needed to expand
their core competencies. Their examination will play a significant role in my study.
Frank Huisman has reminded us that an important role for medical historians is to
persistently subject society's health care organizations to vigorous reflection and re-
examination. The relative levels of medical authority assigned to health practitioners are
constructed by society. Those levels are not static or inevitable and affect the
relationships that develop between health practitioners and the public. Little has been
written about pharmacists' access to authority or their relationships with physicians and
patients. Although operating legally as a self-governing profession since the nineteenth
century, pharmacists' access to authority in society has ebbed and waned since that time.
My thesis provides a case study of British Columbia pharmacists in the mid
1960s, a time when pharmacists in North America were pessimistic about the future of
their profession. Their core competency as experts in compounding prescriptions had
been disappearing in the decades after World War II with the increasing availability of
pre-fabricated pharmaceuticals. Pharmacists were trapped by an ethical code, adopted in
1923, that restricted the scope of their practice while at the same time the core
competency that formed their professional identity had diminished. For much of the
twentieth century, pharmacists were prohibited, by their ethical code, from disclosing the
composition of the medications they dispensed to their patients or discussing patient's
treatment. In the 1960s, pharmacists sought to expand their core competencies to include
recognition as drug information experts and British Columbia pharmacists provide an
important case study since they were one of the first jurisdictions that attempted to
expand their scope of practice. Their formation of the Pharmacy Planning Commission
in 1966 was pivotal for professional development of pharmacists in British Columbia. It
is of particular significance, in a broader context, as it pre-dated similar commissions by
the Canadian Pharmaceutical Association (CPhA) and the Millis Study Commission in
the United States. Their reports were released in 1971 and 1975 respectively.
Until now, neither historians nor pharmacists have focused significant resources
on the history of pharmacy, a fact noted by the few authors who have made contributions.
Even fewer have focused on the Canadian scene. Despite this vacuum, there is a body of
literature that will be useful in carrying out this study. Elenbaas and Worthen in their
recently published article "The Transformation of a Profession: An Overview of the 20th
Century" cover similar topics to those in this thesis, in an American context. While the
two countries differed significantly in their health care systems, pharmacists in both
countries faced similar professional struggles. Their article gives a good description of
the Millis Study Commission on Pharmacy.19
19 Robert M. Elenbaas and Dennis B. Worthen, "The Transformation of a Profession: An Overview of the 20th
Century," Pharmacy in History Vol. 51 No. 4 (2009): 151-182.
The only extensive overview of pharmacy history in the English language is
Kremers and Urdang's History of Pharmacy.20 This book provides a good survey of
pharmacy from the Babylonians through to nineteenth century Europe. The authors then
turn to pharmacy in the United States, which they follow from pre-revolutionary colonial
days into the twentieth century. The extent of its coverage defines its strengths and its
weaknesses. Nowhere else is so much information specific to pharmacy available. This
makes it an essential reference to anyone writing pharmacy history. On the other hand,
like all survey works, it is unable to provide depth to any one subject. For purposes of
this study, it fails to provide any information on the development of pharmacy in Canada.
Therefore, its usefulness is limited to providing a contextual background for Canadian
pharmacy, in comparison to developments throughout the world, and specifically the
United States. Another limitation to this work is that it was originally written in 1940,
although updated in 1976 by pharmacy historian Glenn Sonnedecker. It cannot,
therefore, provide insight into pharmacy developments in the last third of the century.
Daniel Malleck has published several articles which are useful when examining
the shift in pharmacist/physician authority allocations at the turn of the twentieth century.
"Professionalism and the Boundaries of Control: Pharmacists, Physicians and Dangerous
Substances in Canada, 1840-1908" is important because it argues that, despite the
contentious issues that separated them, pharmacists and physicians had entered into an
uneasy alliance by the beginning of the twentieth century.21 Malleck also details
Canada's quest to control addictive substances through two articles, "Pure Drugs and
20 Glenn Sonnedecker, Kremers and Urdang's History of Pharmacy (Madison: American Institute of the
History of Pharmacy, 1976 ). (1986 Paperback edition)
21 Daniel J Malleck, "Professionalism and the Boundaries of Control: Pharmacists, Physicians and Dangerous
Substances in Canada, 1840-1908," Medical History Vol. 48, (2004): 175-198.
Professional Druggists: Food and Drug Laws in Canada, 1870s-1908" and "Its Baneful
Influences are too Well Known: Debates over Drug Use in Canada, 1967-1908."22
Another article of importance is Robert Buerki's "The Historical Development of
an Ethic for American Pharmacy" which follows the evolution of pharmacy ethics in the
United States, noting of particular interest the 1922 clause that prohibited the discussion
of therapeutic effect of a physician's prescription with the patient.23 Buerki has also
published Foundations of Ethical Pharmacy Practice along with Louis Vottero.24 While
this book is intended to provide pharmacy students with a basic grounding in current
pharmaceutical ethical issues, it provides a historical overview of ethical codes put in
place by the American Pharmaceutical Association from 1852 to 1994.
This study is aided by the contributions of scholars outside the discipline of
history. The Social Transformation of American Medicine, by sociologist Paul Starr, is
an excellent study of physicians, and the medical system, as it developed in the
nineteenth and twentieth centuries.25 Starr describes how physicians survived the
competitive climate of the nineteenth century to emerge, in the twentieth century, with
unprecedented professional authority, what he terms "cultural authority." John Harley
Warner compliments Starr on avoiding the temptation to account for this rise by citing
increased efficacy of the new scientific medicine but says he was much more successful
at describing the change than explaining it. Warner finds fault in three areas,
22 Daniel Malleck, "Pure Drugs and Professional Druggists: Food and Drug Laws in Canada, 1870s-1908,"
Pharmacy in History Vol 48 No 3 (2006): 103-110 and Daniel Malleck, "Its Baneful Influences are too Well Known: Debates over Drug Use in Canada, 1967-1908," Canadian Bulletin of Medical History Vol 14 (1997): 236-288.
23 Robert Buerki, "The Historical Development of an Ethic for American Pharmacy," Pharmacy in History
Vol. 39 No. 2 (1997): 54-72.
24 R. Buerki and L. Vottero, Foundations of Ethical Pharmacy Practice (Madison: American Institute of the History of Pharmacy, 2008). 25 Starr, Social Transformation, 9-29.
undervalued alternative medicine in early twentieth century, the lack of recognition of
"the language of science" as a source of cultural authority and the lack of patients'
voices. Despite these objections, and those of other historians, Warner maintains that "no
other synthetic narrative has appeared to supplant Starr's work."26 Warner notes that
Starr's concept of the renewal of legitimate complexity is critical to the understanding of
cultural authority. Starr's work provides a good theoretical discussion on the nature of
authority and status as it applies to physicians in particular, and professions in general.
In addition to Starr, economist Deborah Anne Savage lays out a useful framework
for examining the influence that core competencies can exert on professional authority in
her article "The Professions in Theory and History: The Case of Pharmacy."27 Her study
is flawed in several ways. First, her interpretation of professionalism fails to take into
account the fiduciary nature of professions. Second, her case study of pharmacy confuses
manufacturing with compounding, thus reducing its usefulness. However her discussion
on core competencies is pertinent to the restructuring of pharmacists' professional
identity. Eliot Freidson's "Theory of Professionalism: Method and Substance" and
Professional Dominance: The Social Structure of Medical Care help to fill in the gaps in
professional theory that Savage neglects.28 Philosopher Eike-Henner Kluge provides
background into the origins and uses of medical ethics in his book Biomedical Ethics in a
Canadian Context.29
26 John Harley Warner, "Grand Narrative and its Discontents: Medical History and the Social Transformation
of American Medicine," Journal of Health Politics, Policy and Law Vol 29 No 4-5 (Aug-Oct 2004): 771.
27 Savage, "Professions in Theory," 129-160.
28 Eliot Freidson, "Theory of Professionalism: Method and Substance," International Review of Social and
Behavioural Sciences Vol. 9 No. 1 (1999): 117-129 and Eliot Freidson, Professional Dominance: The Social Structure of Medical Care (New York: Atherton Press Inc, 1970).
29 Eike-Henner W. Kluge, Biomedical Ethics In a Canadian Context (Scarborough: Prentice-Hall Inc, 1992).
Primary sources will be important to this study and the main source will be the
archive of the College of Pharmacists of British Columbia, held in the University of
British Columbia's Special Collections Division. My thesis develops a case study around
the efforts of British Columbia pharmacists to reform their profession through a broad
based commission. The commission is significant because of its success and because it
predates similar national commissions in both Canada and the United States. This
archive includes a nearly complete record of minutes, membership records, financial
records, correspondence and reference files of the Registrar of the College of Pharmacists
of British Columbia, encompassing College activities from its inception in 1891 to the
early 1980s. This archive includes two reports that are critical to this study, The Study
Committee on Pharmacy in British Columbia, completed in 1966 and the Pharmacy
Planning Commission, completed in 1967. Additionally, the archive includes a number
of additional reports that are pertinent to this investigation such as the "Health Services in
Canada" – a report of a working conference on implications of a health charter from 1965
and the "Royal Commission on Health Services" – Pharmacist manpower in Canada from
1966. Also included are various records from the British Columbia Professional
Pharmacists Society, an organization founded in 1968 to protect the interests of
pharmacists. Many of the minutes recorded by each council, at their annual general
meetings and interim meetings, provide a great amount of detail. They provide in depth
information about the issues that were important to pharmacists, and the public, at the
time of each meeting and the different opinions expressed by pharmacists.
While the college records form the bulk of the primary sources for this study, the
Canadian Pharmaceutical Journal provides a useful source of information. Debates on
the issues that were important to pharmacists were often carried out in this journal.
Another important source is the archives of McGill & Orme Prescriptions, a Victoria
pharmacy whose records are in my possession.
My study starts, in Chapter One, with a general historical overview of Canadian
medical and pharmacist authority in the late nineteenth century and the significant shift
that occurred in the early decades of the twentieth century. It discusses how pharmacists
adapted their core competencies to adjust to changing attitudes towards health and health
practitioners. Chapter Two examines the general factors that led up to the crisis in
confidence that Canadian pharmacists experienced in the mid 1960s. Chapters Three and
Four provide a specific case study of pharmacy of in British Columbia from 1965 to
1968. Chapter Three examines the formation of the Pharmacy Planning Commission, in
1966, and the recommendations that came out of their report. Chapter Four examines the
implementation of the Commission's report and their implications for British Columbia
pharmacists. This study will provide understanding in the underlying factors that led
British Columbia pharmacists to reconstruct their profession in the mid-1960s.
Chapter One
I would urge upon you and upon every druggist in Canada to pay serious attention to the educational, professional and ethical problems . which confront us: keeping in view not only immediate results, but the more lasting effect upon Pharmacy as a vocation.30
CPhA President W. McMullen's Address to 1923 Annual Convention
In 1930, William McGill and Cecil Orme founded McGill & Orme Prescription
Chemists in Victoria, British Columbia.31 Their business was described by McGill as an
"old apothecary shop" which would "confine itself to the filling of prescriptions."32 They
pledged to carry sick room supplies, vaccines and extracts but not the general goods
usually found in contemporary pharmacies. In 1935, they wrote a letter to the physicians
of Victoria announcing that they were moving their pharmacy to a new location.33 They
used the opportunity to reiterate a statement of ethics originally declared when they first
opened for business. One clause in their declaration is remarkable above all others,
stating that a pharmacist should have "no discussion with the patient as to symptoms or
treatment, believing that such belongs in the sphere of the physician only." Pharmacists
in the twenty-first century believe that one of their most important professional roles is to
discuss treatments with their patients and, in fact, they are legally and ethically obligated
to do so.34 In this chapter, I will analyze McGill & Orme's statement for insight into
early twentieth century medical authority, through the exploration of three areas of
30 W. McMullen, "President's Address to CPhA 1923 Convention," Canadian Pharmaceutical Journal Vol
LVI No. 12 (July 1923): 447.
31 I have used McGill & Orme not McGill and Orme because that is how the company identified itself in all
documents, advertising and signage.
32 Victoria Daily Times, 7 November 1930. Appendix C shows that McGill & Orme increased from 7.64
Rx/day in March 1931 (4 months after opening) to 108 Rx/day in 1947.
33 See Appendix A for a copy of McGill & Orme's letter.
2010). See Appendix G for a copy of the Code of Ethics adopted in 2009.
inquiry. First, did this statement, made by one Victoria pharmacy, reflect the wider
ethical values of their contemporaries? Second, what does this ethical statement reveal
about medical authority and its effect on physician-pharmacist-patient relationships in the
early twentieth century? Finally, I will examine the implications that this ethical code
had for physicians, pharmacists and patients in a general Canadian context.
In the late nineteenth century, pharmacists had fought hard and successfully for
legal professional status, in both Canada and the United States. In British Columbia
pharmacists were trained as apprentices with private pharmacy schools adding some
academic instruction; an educational system that continue until the middle of the
twentieth century. Before being granted licensure, pharmacists were tested in six
subjects; botany, chemistry, materia medica, prescriptions, pharmacy and dispensing.35
These subjects were focused primarily on pharmacists' manufacturing and compounding
roles. In some jurisdictions, such as Ontario and the Maritimes, pharmacists could
qualify with a degree in pharmacy from a university or through apprenticeship.36
Pharmacists who had qualified from jurisdictions whose "standing and requirements are
equal to those of the [B.C.] association" could be licensed without examination.37
Pharmacists could lay claim to a wide scope of practice composed of four core
competencies: manufacturing, compounding, diagnosing and prescribing. Pharmacists
were not only expert compounders of physician's prescriptions but also manufactured
drugs directly from raw materials. In addition, capitalizing on the public's desire to self
medicate, pharmacists engaged in the practice of "counter prescribing"; diagnosing their
35 University of British Columbia Special Collections, College of Pharmacists of British Columbia Records
(hereafter UBC-SM-CPBC), Box 27-8, Pharmaceutical Association of British Columbia licensing exams- 1914, 1921, 1928 (hereafter Licensing exams).
36 UBC-SM-CPBC, Box 27-8, Licensing exams.
37 UBC-SM-CPBC, Box 9-1, Pharmacy Act – amended to December 24, 1925 Clause 12-1.
customers' ailments and prescribing treatments as well as compounding those treatments.
None of these competencies were distinct, by Deborah Savage's definition, since
physicians often compounded prescriptions as well as diagnosing and prescribing. The
manufacturing role of community pharmacists was diminishing, due to the emergence of
large scale pharmaceutical manufacturers. Despite sharing these competencies with other
groups, pharmacists were recognized and respected as legitimate practitioners of all four
In Canada, physicians fought hard to prohibit counter prescribing as they felt that
pharmacists had "no knowledge whatever of diagnosis and pathology."38 Attempts to
curb pharmacists by guiding legislation through Ontario's legislature failed, partially
because of defensive lobbying by pharmacists.39 Physicians were supported neither in
the courts when they tried to bring actions against pharmacists nor in the media. One
newspaper editorial explained their position,
the professional man may not be at home or cannot come immediately when
called; while the chemist is always behind his counter. A still more important consideration is involved . we shut off from the poor cheap and ready medical assistance.40
Pharmacists benefited from their accessibility to the public, as well as their ability to
provide cheap medical assistance. Physician authority was not strong enough to
overcome the public's belief that pharmacists provided diagnosis and treatment that was
accessible, inexpensive and legitimate.
Counter prescribing by pharmacists was also opposed by pharmacy elites, who
tried to prohibit its practice through the use of ethical codes. The American
38 Clark, "Professional Aspirations," 52.
40 Ibid., 52-53.
Pharmaceutical Association (APhA) had declared, in their 1852 Code of Ethics, that "the
practice of pharmacy is quite distinct from the practice of medicine" and "the conduction
of the business of both [medicine and pharmacy] professions by the same individual"
could lead to "pecuniary temptations."41 In April 1880, the Victoria Pharmaceutical
Society developed a Code of Ethics that included the clause that pharmacists should not
practice medicine or give medical advice.42 Some pharmacists followed those ethical
directives; Victoria newspapers carried the advertisement "If you are sick see a doctor. If
you get a prescription [see] C.E. Jones [at] The Peoples Popular Prescription Pharmacy."
In many other cases, pharmacists ignored that ethical stricture.
Physician's efforts to prevent pharmacists from counter prescribing had failed to
find support through legislation or through the press. Pharmacy elites had similarly failed
to control it with ethical codes. Pharmacists did not accept an ethical code that prohibited
counter prescribing because the public supported its practice. Although not formally
constructed, pharmacists operated in an ethical environment that most closely resembled
an agency model. Patients were primarily responsible for their own healthcare decisions
and were free to access whichever health professional they trusted to provide them with
information or treatments they required.
Much of the public's thirst to self medicate was quenched by the increasing
availability of so-called "patent" medicines, although most of these medications were not
actually patented. Those medicines that were patented had their formula revealed in the
details of their patent. More often, although termed patent medicines, they were not
actually patented but were considered as proprietary products by their manufacturers and,
41 David Cowan, "Pharmacists and Physicians: An Uneasy Relationship," Pharmacy in History Vol. 34 No. 1
42 The Daily Colonist, 15 April 1880, 3.
as such, their formulas were kept secret. They were advertised directly to the public as
specific remedies for specific diseases, often with extravagant claims of success.
Physicians felt that specifics made people "look to the medicine alone, as possessing the
skill within itself – as though it had intelligence, genius, judgment, learning, all
combined."43 While physicians and pharmacists both condemned patent medicines, their
objections were never completely consistent with their actions. Physicians participated in
their sale through endorsements and most prescribed them to their patients. In 1890, Dr.
D.D. McDonald claimed in an advertisement in the Victoria Daily Colonist that "I have
been prescribing Scott's Emulsion with good results . especially . in persons of
consumptive tendencies."44 Some physicians also manufactured patent medicines as did
pharmacists but, more importantly, pharmacists also sold them in their pharmacies.
Druggists Cochrane and Munn advertised Aphrodite, the celebrated French cure,
warranted to cure any nervous disease or money refunded.45 A pharmacist in 1880,
declared that patent medicines made up thirty percent of his sales, a strong indication
how economically dependent pharmacists were on patent medicines and self-
At the beginning of the twentieth century, the spectre of drug addiction from
recreational drug use and patent medicines had become a concern in Canada. William
Lyon Mackenzie King, federal deputy minister of labour and future Prime Minister, had
observed that smoking opium resulted in "baneful influences [that] are too well known to
43 Lee Anderson, Iowa Pharmacy 1880-1905: An Experiment in Professionalism (Iowa City: University of Iowa Press, 1989), 23. 44 The Daily Colonist, 19 February 1890, 1.
45 The Daily Colonist, 11 March 1891, 4.
46 Canadian Pharmaceutical Journal Vol XIII No 7 (1881): 238.
require comment."47 Patent medicines were also coming under fire, in both Canada and
the United States. Many patent medicines were, in reality, nothing more than standard,
safe formulations from the British or U.S. pharmacopoeia. On the other hand, others
contained addictive drugs such as cocaine, morphine, heroin, and opium as well as
excessive amounts of alcohol. The fact that their formula was secret meant that neither
the public nor pharmacists and physicians knew which products might be harmful.
The public's use of addictive drugs led to the fear that the health of the nation
could be harmed, as well as individuals. In 1907, the Western Canada Medical Journal
noted that "the best asset that any nation can have . is health."48 Physicians used the
opportunity to criticize the practice of self-medication, "the first objection to proprietary
medicines is that the prescribing of such preparations is apt to lead to self-medication by
the public."49 Physicians were clear that "our weak-kneed friend, the druggist" had
pandered to the public's desire for self-medication by selling patent medicines and
thereby helping patients avoid paying the physician's fee.50 The editor of the Canadian
Pharmaceutical Journal accepted the criticism, but felt the blame was the result of three
causes, "the carelessness on the part of physicians . a certain class of patent medicines .
[and] the aid rendered by unscrupulous druggists."51
The debate over the appropriate control of patent medicines elicited different
solutions from physicians and pharmacists. Physicians wanted full disclosure of the
formula on the label. Pharmacists banded together to form the Canadian Pharmaceutical
Association (CPhA) and argued that disclosure was naïve, as it didn't recognize the
47 Malleck, "Baneful Influences," 264.
48 Ibid., 274. 49 Anderson, Iowa Pharmacy, 132. 50 Malleck, "Pure Drugs," 111.
51 Malleck, "Professionalism," 188.
manufacturer's rights to protection from competitors copying their product. They also did
not believe that the public were knowledgeable enough to understand the formula.52
Pharmacists wanted manufacturers to submit their formulas to an impartial government
board. When the Patent and Proprietary Medicine Act was finally passed by the federal
government in 1908, they chose a compromise between the two suggestions. Products
that contained substances from an attached schedule would be labelled with those
ingredients. If the manufacturer chose to print the entire formula on the label, they would
be exempt from the act.
The passage of the Patent and Proprietary Medicine Act was of critical
significance to pharmacists, physicians and the public. Manufacturers were required to
register annually with the federal Inland Revenue department and submit their formulas
and products for analysis.53 For the first time, social authority over drugs included
laboratory science and was administered by the federal government. Daniel Malleck has
argued that this signalled a shift by pharmacists and physicians to use laboratory science
to back up their right to protect the public from dangerous drugs. They had previously
relied on moral authority and character. The act prohibited the inclusion of cocaine in the
formula of any patent medicine. Henceforth, cocaine would only be available on a
physician's prescription, filled by a licensed pharmacist. The 1911 Opium Act added
morphine and opium to the list and, perhaps more significantly, empowered the
government to add substances as was "deemed necessary in the public interest."54 For
physicians, these two acts made them gatekeepers assigned with the authority to
safeguard the public from the misuse of drugs. A self-medicating public was seen as
52 Malleck, "Pure Drugs," 111.
54 UBC-SM-CPBC, Box 9-1, An Act to prohibit the improper use of Opium and other Drugs, May 19, 1911.
detrimental to the health of the nation; physicians were now the public's best source of
medical advice and treatment. S.E.D. Shortt has explained that the advanced knowledge
of physiology and pathological conditions meant that medical knowledge was no longer
accessible to the layman. Physicians "gained stature not because they could always act
effectively, but because only they could name, describe and explain."55
For pharmacists the verdict was mixed. On one hand, they had succeeded in
pushing the government to consider their views on patent medicines. They had also won
the right to be the only legally sanctioned distributors for the drugs named in the act. On
the other hand, views on self-medication and counter prescribing had hardened, resulting
in a reduced scope of practice for pharmacists.56
Pharmacists' traditional core competency of manufacturing was also
disappearing. A pharmacist's primary skill for centuries had been manufacturing
medications directly from raw materials, usually botanical but sometimes chemical.
They were trained to distil and extract active medicinal ingredients from plants and
prepare them in a form that allowed ingestion or application by the patient. Pharmacists
also had training in chemistry that facilitated the manufacture of medications such as
ether or chloroform.
R. J. Clark argues that during the last twenty years of the nineteenth century, physicians
were standardizing the dosage forms they prescribed. This consolidation encouraged
wide scale manufacturing and reduced the role played by pharmacists as "cottage
55S.E.D. Shortt, "Physicians, Science, and Status: Issues in the Professionalization of Anglo-American
Medicine in the Nineteenth Century," Medical History Vol. 27 (1983): 63.
56 McGill & Orme's letter in 1935 assured physicians that they would discourage the use of secret or quack
nostrums. They would advise their patients to see their physician instead. The CPhA and APhA code of ethics "discouraged the use of objectionable nostrums." It is ironic that physicians and pharmacists discouraged the use of secret remedies at the same time that they were keeping the composition of their prescriptions secret.
industry" manufacturers.57 This development coincided with a shift from skilled
tradesmen to mass production techniques. It was at this time that pharmaceutical
companies such as Merck, Lilly, Frosst and Abbott were founded. Manufacturing
innovations such as automatically powered compressed and coated tablet machines in
1875 and Warner's parvules (small pills) in 1879 could be produced on a large scale.
New extraction processes pioneered between 1845 and 1875 and biological products,
such as diphtheria anti-toxin, at the turn of the twentieth century were not suited for
manufacture in community pharmacies.58 It made more sense to purchase pre-fabricated
medications from manufacturers whose economies of scale could provide pharmacists
with cost savings. By the twentieth century, the manufacturing role had all but
disappeared from community pharmacies. Pharmacist J. Murdoch felt that this shift had
resulted in a loss of prestige and expertise, "our knowledge of dispensing is confined to
washing the bottle and being careful not to spill the mixture." This, he says, meant that
"the public are beginning to question our right to make any charge for knowledge or
services, in filling the prescription."59 Lee Anderson argues that pharmacists gambled on
the strength of self medication and manufacturing traditions. The loss of both avenues of
revenue left them in a vulnerable position.60 Pharmacists had lost the legitimacy that
specialized skill and competence in manufacturing had provided. When added to the loss
of legitimacy created by the movement away from self-medication, the public's overall
dependence on pharmacists had also diminished. As Paul Starr has argued, a reduction in
legitimacy and dependency is reflected in a corresponding reduction in authority. Loss of
57 Clark, "Professional Aspirations," 46.
58 Sonnedecker, History of Pharmacy, 329.
59 J. Murdoch, "A Far Cry from Swansdown to Suntan," Canadian Pharmaceutical Journal Vol LXII No.22 (July 15, 1929): 777. 60 Anderson, Iowa Pharmacy, 137.
authority contributed to a sense of pessimism among pharmacists by the early twentieth
century. Some feared that pharmacy might disappear as a profession altogether.
The rise of scientific medicine in the late nineteenth century created the optimistic
view that science might ultimately solve all health problems. Progress had been made in
diagnosis, antiseptic techniques and surgery as well as preventative measures such as
vaccines and public health measures. Drug therapy, however, had seen very few
advances. Oscar Herzberg wrote, in Lippincott's Magazine in 1898, that "it is not
unreasonable to believe that … the drug-shop will be in less and less demand, until … it
may become entirely extinct."61 The spectre that their profession might disappear
completely weighed on the minds of pharmacists.
It was in this context that the work of educator Abraham Flexner contributed to
pharmacist insecurity. In 1910, he had written a report for the Carnegie Foundation that
advocated the reform of medical education in the United States and Canada.62 Although
Flexner did not include pharmacy in that report he did examine the question, "Is
Pharmacy a Profession?" in a separate study, in May 1915.63 His findings were not
designed to please pharmacists, and they did not. On the positive side, he found that
pharmacy had a definite purpose, communicable technique and acquired essential
material from science. On the negative side, Flexner claimed, pharmacy was not
primarily intellectual and its responsibility was not primary or original. "The physician",
he said, "thinks, decides and orders while the pharmacist obeys, albeit with discretion,
61 Robert Buerki, "The Public Image of the American Pharmacist in the Popular Press," Pharmacy in History
Vol. 38 (1996): 73.
62 Abraham Flexner, Medical Education in the United States and Canada (North Stratford: Ayer Company
Publishers Inc, 2003 reprint edition).
63 Buerki and Vottero, Foundations, 5.
intelligence and skill." Flexner concluded that pharmacy was an arm of medicine, not a
Flexner's verdict struck directly at pharmacists' professional identity. The loss of
counter prescribing and manufacturing as core competencies and the resultant reduction
of authority left pharmacists demoralized and pessimistic about their future. CPhA
President, W. McMullen, started his address to the 1923 convention with the declaration
that "the future of Pharmacy is uncertain. It is a matter of grave concern to us what the
future will be."65 McMullen was not alone in his fears; throughout the 1920s many
others were adding their voices to the chorus. Dr. V. Henderson, Professor of Pharmacy
and Pharmacology at the Faculty of Medicine, University of Toronto, said that "this
continent has run wild on pharmacy as a business and not as a profession."66 An editorial
in the Canadian Pharmaceutical Journal felt that the public's regard for pharmacists was
"slipping down the ladder rung by rung."67 The problems, President McMullen said in
his opening address to the convention, were educational, professional and ethical.
Pharmacists in the United States felt the same despair. In an attempt to remedy
the situation, APhA president Charles LaWall, proposed a revision of their 1852 Code of
Ethics. Flexner's determination that professions are "explicitly . meant for the
advancement of the common social interest" led LaWall to declare that "the soul . of a
professional organization is its code of ethics."68 Although LaWall received "sincere
support" from the APhA, no concrete action was taken so he undertook the project
64 Buerki, "Historical Development," 57.
65 W. McMullen, "President's Address to CPhA 1923 Convention," Canadian Pharmaceutical Journal, Vol
LVI No. 12 July 1923, 447.
66 Editorial, Canadian Pharmaceutical Journal, Vol LIX No 12 (July1926): 536. 67 V. Henderson, "Dr. Henderson urges the Importance of Advance in Canadian Pharmaceutical Education," Canadian Pharmaceutical Journal Vol LIX No 9 (April 1926): 367. 68 Buerki and Vottero, Foundations, 3.
himself in the hope that it would restore pharmacists' professional prestige and
reputation.69 LaWall's new version was adopted by the APhA in August 1922.70
The CPhA invited LaWall to their convention as keynote speaker, in July 1923, to
discuss pharmaceutical ethics. At the convention, the CPhA adopted the APhA Code of
Ethics as a basis for their own, with only a few minor modifications. LaWall divided his
code of ethics into three sections, each one detailing a pharmacist's duty to a different
constituency.71 Significantly, LaWall included physicians, along with the public and
fellow pharmacists, highlighting his belief that pharmacists had a special relationship
with physicians, worthy of special ethical conditions. The code enumerated a series of
role-specific rules that were unique to the profession of pharmacy, spanning issues from
the conduct of wholesalers to patient confidentiality to financial arrangements with
physicians. The following clauses (numbered for clarity) were included as duties to the
The Pharmacist even when urgently requested so to do should always
refuse to prescribe or attempt diagnosis. He should, under such
circumstances, refer applicants for medical aid to a reputable
legally qualified Physician.
He should never discuss the therapeutic effect of a Physician's prescription
with a patron nor disclose details of composition which the Physician has
withheld, suggesting to the patient that such details can be properly discussed
with the prescriber only.72
McGill & Orme's ethical statement can be recognized as an economically worded
rephrasing of the above two clauses. Based on its genealogy, it appears that McGill &
71 See Appendix G for a copy of the APhA Code of Ethics.
72 "Principles of Pharmaceutical Ethics," Canadian Pharmaceutical Journal, Vol LVII No. 3 (October 1923):
Orme's ethical view did reflect the wider view of their contemporaries, both in Canada
and the United States.
I will analyze both of these ethical statements by connecting McGill & Orme's
concise version to the more comprehensive clauses adopted by the CPhA and APhA.
McGill & Orme's promise to refrain from discussion of symptoms encapsulates the heart
of the first clause. Symptoms, whether observed or measured, are the basis upon which
diagnosis is determined. McGill & Orme's prohibition on discussing treatment with
patients also summarizes the first clause, as well as the second. Treatment is the end
result of prescribing but also can be used to "back engineer" information about the
diagnosis. Any discussion of treatment or symptoms could migrate to an evaluation of
the appropriateness of either the diagnosis or the prescribed treatment, both designated,
by the code, as within the professional boundaries of the physician. Charles LaWall
emphasized this point, in his revised Code of Ethics, by including it within the
pharmacist's duties to the public, as well as to physicians. Pharmacists, he said, "should
make no attempt to prescribe or treat diseases."73 By including this prohibition on
diagnosis and prescribing as a duty to the public, LaWall acknowledges that pharmacists
who engaged in this practice were potentially jeopardizing the safety of the public. A
prohibition was necessary to follow Flexner's view that professions must advance the
common self-interest. This meant putting the public's interests ahead of those of
The promise not to discuss treatment summarizes the second clause;
encompassing both therapeutics and composition. This clause would be unacceptable to
twenty-first century pharmacists because therapeutics forms the basis of their profession. 73 Ibid., 18.
To resolve the dichotomy created between professional views from both eras requires an
examination of the term "therapeutics", as well as medical and pharmacy education. In
the twenty-first century, therapeutics is closely associated with pharmacology. Standard
pharmaceutical reference books, such as Goodman and Gilman's The Pharmacological
Basis of Therapeutics, emphasize the interaction of the two subjects.74 These reference
books, as well as detailing the indications (uses) of drugs, also explain the post-
administration reactions that occur when drugs interact with complicated physiological
processes in the human body. Included in that discussion are drug-drug interactions and
drug side-effects. Modern therapeutics is largely concerned with what happens after the
drug enters the body and twentieth-first century pharmacists are extensively trained in
therapeutics and pharmacology. When McGill & Orme made their ethical statement,
therapeutics had a narrower meaning and pharmacists had different training. The
Merriam-Webster dictionary traces the term therapeutics back to 1671 and cites its
definition as "the application of remedies to diseases."75 That definition is restricted to
the indications aspect of therapeutics with no mention of post-administration effects.
Medical science, in the 1920s and 1930s, did have some knowledge of post-
administration effects of drugs and that knowledge was taught to physicians through
courses in pharmacology. Pharmacists, however, did not receive any training, nor were
they examined, in pharmacology or any other related studies such as toxicology. The
reference books used by pharmacists, such as the British or U.S. Pharmacopoeia, give the
indications of drugs but virtually no information on post-administration implications.
74 Goodman and Gilman's The Pharmacological Basis of Therapeutics was first published in 1941 and is
currently in its 11th edition.
75 Merriam-Webster Dictionary, (February 2,
The narrower definition of therapeutics at the time put therapeutics outside the practice
boundaries of pharmacists. Further, and even more significantly, pharmacists were not
trained in pharmacology and were therefore not qualified to discuss therapeutics, in the
modern sense, with competence.
McGill & Orme's 1935 promise not to discuss treatments with patients would
have assured physicians of their agreement not to disclose composition. The Pharmacy
Act of 1925 states that disclosing the composition of a prescription was not required if it
originated from a physician's order.76 In this circumstance, pharmacists were neither
legally required nor prohibited from labelling prescriptions with its composition. On the
other hand, with the exception of cocaine, morphine and heroin, pharmacists were
allowed to compound and dispense any drug without a physician's prescription but, in
that case, they were required to record the composition on the label.77 Additionally, the
Pharmacy Act specifically stated that any person could request a copy of their
prescription, provided the pharmacist kept the original on file.78 The decision to disclose
composition, therefore, was legally within the jurisdiction of the pharmacist and the
patient. Conversely, the ability to keep the composition secret was out of the physician's
legal control. In practice, however, pharmacy ethics promised to voluntarily revert that
control back to physicians. In this case, pharmacy ethics increased physician authority
beyond what was assigned to them by law. For pharmacists, this allowed them to
strengthen their link to physician authority, as well as ensuring that the public would
continue to be dependent upon physicians and pharmacists to provide treatments for their
76 UBC-SM-CPBC, Box 9-1, Pharmacy Act – amended to December 24, 1925 Clause 28.
77 Ibid., Clause 26 & 27.
78 Ibid., Clause 23.
Did pharmacists, in practice, withhold composition? In addition to the Code of
Ethics declaration, and McGill & Orme's letter, there are two additional pieces of
information that indicate that they did. Appendix D shows labels from the 1930s to the
1960s that were generated without composition information. Additional evidence comes
from two books of prescriptions, filled at McGill & Orme in 1931 and 1947 (Appendix
C). In practice, when a physician wanted a pharmacist to disclose composition he would
add the notation "label" to his prescription. In these cases, the pharmacist would label the
prescription with its composition. In the survey, I found that only one prescription
included the notation "label" in each sample.79 McGill & Orme's records can be
reasonably taken to represent pharmacists' practices at that time and they indicate that, at
least in this pharmacy, physicians rarely asked pharmacists to reveal composition.
Considering all these factors it is unlikely that pharmacists revealed the composition of a
physician's prescription, except in rare occasions, and only on the request of the
prescribing physician.
Why would physicians want to withhold the composition of a prescription? In
most cases, in the 1920s and 1930s, patients would have to pay to consult a physician.
From a physician's point of view, the treatment they prescribed represented the tangible
result of the patient's consultation with the physician. Included in the cost of consultation
was the intangible art and skill of the physician's diagnosis and choice of treatment.
Disclosing composition and discussing diagnosis would reveal the secrets of the
physician's art and skill. The potential implications of these revelations can be seen
through an examination of the 1931 McGill & Orme prescription survey. Here we see
that only 58 out of 978 prescriptions were for heroin, morphine and cocaine. These were 79 See copies of prescriptions in Appendix C.
the only drugs that the Pharmacy Act restricted solely to a physicians' prescription.
Conversely, 920 prescriptions could have been dispensed on the direct request of a
patient, without a physician's prescription.80 These included phenobarbital, digitalis,
phenazopyridine, quinidine and quinine, all of which were eventually made prescription
only. If the composition of their treatments was revealed, patients could use that
information at a later date to self-medicate, either for their own conditions or those of
their family or friends. This would be facilitated further, if the patient's diagnosis was
discussed by the pharmacist. Therefore, prohibition on the discussion of diagnosis was
important to physicians for proprietary reasons, not just to prevent second guessing.
A second reason that physicians might not wish to reveal composition was the
number of manufactured products, many of them patent medicines. The sample
examined from the records of McGill & Orme show that 390 out of 978 or 40% of
prescriptions dispensed were manufactured products.81 This ratio of manufactured
products to total prescriptions fits roughly with other surveys of this time period. In the
United States, manufactured products were found to make up 25% of the prescriptions
surveyed.82 The sample includes patent medicines such as Musterole, Lavoris, Calamine
Lotion and Ichthyol antiseptic vaginal cones. Most of these products, like many other
prescribed remedies, could be purchased without a physician's prescription, at a
pharmacy, department store or grocery.
Access to prescription information may have tempted patients to economize by
self-medicating their conditions with non-prescription or patent medicines rather than 80 In 2010, the situation is reversed. The vast majority of prescriptions are written for drugs that can only be
obtained through a physician's prescription. Therefore, secrecy is not important to safeguard the physician's art and skill. Even when the patient knows what was prescribed they are unable to get more in the future without a prescription from the physician.
81 See Appendix C. 82 Sonnedecker, History of Pharmacy, 315.
consulting a physician. For pharmacists, revealing the composition of a prescription
might encourage patients to purchase patent medicines in non-pharmacy locations. The
increase in drug regulations was an important part of the transference of medical
authority to physicians, in the early years of the twentieth century. Having lost the
authority to be advisors to the public in their efforts to self medicate, pharmacists saw
that their best interests lay in supporting physicians in their efforts to control information
about their patient's health.
President McMullen had warned that pharmacists faced educational, as well as
ethical and professional problems. Pharmacists still retained an educational curriculum
designed for manufacturing, despite the fact that its usefulness was becoming limited.
Pharmacists were not required to have any knowledge of anatomy, physiology,
bacteriology, toxicology, or pharmacology. By the twentieth century, these were the
subjects that formed the basis of modern medicine.
By the 1920s, pharmacists were coming under fire from within the profession as
well as from the medical profession because their education had not kept up with the
times. Dr. V Henderson, told pharmacists that "we are talking a different language"
because pharmacy education had not kept pace with new developments.83 This lack hurt
pharmacists because, as Eliot Freidson argues, "without a common language, cooperative
endeavours are impossible." 84 Dalhousie Pharmacy Dean, George Burbidge, believed
that education should be "acquired only in a college of pharmacy . in close contact with
the science and medical facilities of a university."85 Burbidge, like many pharmacists,
83 Henderson, " Canadian Pharmaceutical Education," 536.
84 Freidson, "Theory of Professionalism," 117.
85 G. Burbidge, "Are Apprentices being properly Educated?," Canadian Pharmaceutical Journal Vol LIX No 8 (March 1926): 313.
worried whether the profession would survive and believed that education needed to be
improved, before pharmacists could advance.
These commentators indicated that educational improvement could be achieved in
three areas. First, pharmacy needed to be taught in universities where it would have
access to medical and scientific faculties. Private pharmacy schools were no longer
adequate to educate pharmacists. Second, pharmacists needed to re-evaluate certain areas
of study, specifically botany and materia medica, which were rooted in their
manufacturing past. Third, pharmacists needed to learn to speak the modern language of
medicine. Burbidge believed that pharmacy needed to update the field of materia medica
to courses in pharmacology.86 Progress in education was uneven across Canada. Some
provinces, such as Ontario and Nova Scotia, were already educating pharmacists at
universities in the 1920s. British Columbia would be the last to convert; at the 1925
Annual General Meeting of the Pharmaceutical Association of British Columbia (The
Association), Councillor Crowder told the meeting that the association was seeking
affiliation with the University of British Columbia. Curriculum, he said, should be
adjusted to include biology and toxicology with reduced emphasis on botany but, due to
competition for facilities at the new university, no progress should be expected for three
or four years.87 In reality, Crowder was optimistic; pharmacy education would not move
to the university until 1948. The state of pharmacy education in the 1920s was such that
pharmacists were unqualified to do more than compound prescriptions. They had no
educational legitimacy to diagnose or prescribe and had lost the economic viability as
medicinal manufacturers.
86 Burbidge, "Apprentices," 313.
87 UBC-SM-CPBC, Box 23-33, Minutes of Annual General Meeting, Pharmaceutical Association of British
Columbia, June 10, 1925.
Pharmacists were at a professional crossroads. They had lost their manufacturing
function as well as their role in self-medication. Their education over emphasized a
manufacturing role that had all but disappeared and was deficient in the subject areas that
defined modern medicine. Pharmacist's insecurities about the future of their profession
were encouraged by plans to classify pharmacy as a trade by the British Columbia
legislature. This plan was thwarted by a delegation led by CPhA delegate, John
Cochrane.88 A Canadian Pharmaceutical Journal editorial advocated in 1925 that
pharmacists return to their ancient role as the physician's cook, focusing their fortunes on
the remaining core competency of compounding physician's prescriptions. Forming
what LaWall termed an "entente cordiale" would allow pharmacists to attach their
professional fortunes to the medical authority of physicians.89 A key feature to any
arrangement with physicians would be a prohibition on diagnosis and prescribing by
pharmacists, a goal that had proven unachievable in the past.
Pharmacy elites were aided in their goal by increasingly stringent regulations and
enforcement. The Act Respecting the Practice of Medicine and Surgery had specified,
since 1911, that only those who were licensed as members of the College of Physicians
and Surgeons could practice medicine in British Columbia.90 In Ontario, pharmacists
were warned that they would be prosecuted if they counter prescribed in contravention of
their medical legislation.91 The files of the Association contain numerous letters citing
88 Raison, Brief History of Pharmacy, 35.
89 Buerki, "Historical Development," 68.
90 UBC-SM-CPBC, Box 9-1, An Act respecting the Practice of Medicine and Surgery, 1924.
91 Canadian Pharmaceutical Journal, Vol LIX No. 6 (Jan 1926).
pharmacists for infractions against the by-laws.92 Regulation and enforcement was now
sufficiently strong to ensure that those who did not comply would be disciplined.
The Code of Ethics adopted by the CPhA went beyond legally defined limits,
however. The prohibition on counter prescribing, the discussion of treatment and the
disclosure of composition were only partially backed by legal statute. Pharmacy elites
had endorsed a similar prohibition for decades but lacked the authority to enforce its
adoption throughout the pharmacy profession. Pharmacist's professional practices were
now dictated, in detailed form, by the pharmacy elite. Local pharmacies, such as McGill
& Orme Prescriptions, provided consensus for the 1923 code because they believed that
confining their professional pattern of practice to the filling of physician's prescriptions
was their best hope for professional survival. Pharmacists were able to replace authority
lost by the reduction of their core competencies with authority gained by forging
professional alliances with physicians. Pharmacists' success in attaching themselves to
the authority of physicians meant that the public would remain dependent on pharmacists
for drug distribution and physician's for drug information for nearly fifty years.
Pharmacists may have lost some of the authority they had enjoyed in the nineteenth
century but were able to forestall the fears of their demise by attaching themselves to
physician authority and concentrating on their one remaining competency, compounding.
92 UBC-SM-CPBC, Boxes 2-5, 2-6, 2-7, 2-25, Letters and Inspections, 1891-1917.
Chapter Two
Today, the public overlooks the real mission and social value of our profession.
We forget to put in the limelight the importance and real dignity of our work and of our social role … We are losing our prestige.
Emile Coderre August 14, 195793
In the 1920s, pharmacists identified their core competency as the compounding of
physician's prescriptions. Using the Code of Ethics, pharmacy elites were able to ensure
that pharmacists stayed primarily within the capabilities dictated by this core
competency. As long as compounding skills were required to fill the majority of
prescriptions, this remained a viable capability. In this chapter, I will examine how the
dynamics of pharmacy in North America changed significantly after World War II, in
two very important ways.
Firstly, the number of prescriptions increased rapidly. In the United States,
prescriptions rose from 400 million per year in 1950 to 1 billion per year in 1965 while
prescriptions usage rose from 2.4 to 5 prescriptions per person per year from 1950 to
1965.94 The increase came mainly from increased prescription usage, not increased
population. Canada experienced a similar trend; the number of prescriptions filled
increased from 35 million in 1956 to 60 million in 1965.95
The second change that occurred was the mix of prescriptions filled by
pharmacists. More and more, prescriptions were being filled with manufactured pre-
fabricated products, primarily tablets and capsules, while pharmacists were being called
93 UBC-SM-CPBC, Box 9-18, Emile Coderre, introductory remarks to the paper "An outline of the History of
Pharmacy in the Province of Quebec from 1617-1930." presented to the Canadian Academy of the History of Pharmacy, Montreal August 14, 1957.
94 Stephen Schondelmeyer, "Recent Economic Trends in American Pharmacy," Pharmacy in History Vol. 51 No 3 (2009): 104-5. 95 UBC-SM-CPBC, Box 12A-10, Report of the Pharmacy Planning Commission, May 1967 (hereafter PPC
on to compound fewer prescriptions. We can see this trend in the analysis of McGill &
Orme's prescription registers, the percentage of compounded prescriptions dropped from
sixty percent in 1931 to twenty-five percent in 1947.96 In the United States, statistics
were similar, compounding dropped from seventy-five percent in 1930 to twenty-six
percent in 1950 and to three-four percent in 1962.97
Elenbaas and Worthen have examined the twentieth century transformation of
United States pharmacy and conclude that "pharmacy was at the crossroads" in the 1960s
and 1970s. Their verdict was that pharmacists were viewed by the public as the "most
overeducated and underutilized healthcare profession" who achieved little more than
"counting pills from big-bottles into little bottles."98 Pharmacists reached this
unenviable position, they say, because of the decline in compounding and the increase in
pre-fabricated medications.
From a business perspective, this shift in prescription dynamics was a boon to
community pharmacists. Although the loss of compounding represented a corresponding
loss of revenue this was more than made up by the increase of prescription volume.
Pharmaceutical companies constantly developed new medications and many, such as
penicillin, tetracycline and other antibiotics, were dramatically effective. Manufacturers
were also successful in simultaneously promoting new medications and the conditions
they treated. Although advertising was restricted in the United States by the enforced
inclusion of risks as well as benefits, pharmaceutical companies were able to infiltrate
popular media to create demand.99 Pharmaceutical companies formed the Medical and
96 See Appendix C.
97 Sonnedecker, History of Pharmacy, 315.
98 Elenbaas and Worthen, "Transformation of a Profession," 156-7.
99 David Herzberg, "Will Wonder Drugs Never Cease!," Pharmacy in History Vol. 51 No 2 (2009): 50.
Pharmaceutical Information Bureau (MPIB) which distributed drug information,
complete with brand names, to the media. Articles such as "Aureomycin: It fights germs
penicillin won't" read like news articles and promised availability" right now on your
doctor's prescription."100 Miltown (meprobamate) was touted in Cosmopolitan magazine
by MPIB writer, Donald Cooley, as bringing "perfect peace" and helping "frigid women
who abhorred marital relations" and juvenile delinquents to become "calm . quiet,
cooperative, better-behaved children."101 This trend helped expand the market for
medications. Other health breakthroughs such as polio vaccines increased the public's
confidence in medical science. Prescription revenue increased in the United States from
$1.25 billion in 1955 to $2.75 billion in 1965.102 In Canada, prescription revenues
increased from $87 million in 1956 to $200 million in 1965.103 Since pharmacists priced
prescriptions with a mark-up on the cost of the drug these revenue increases resulted in a
gross margin increase of over 100% over the ten year period. Pharmacies benefited from
this increased revenue and dispensaries started to contribute more to the overall financial
health of the drugstore. In the United States, twenty-five percent of drugstores in 1962
received at least half of their revenues from the pharmacy department, up from only one
percent in 1931.104 Economic benefits came from more than just increased prescription
volume. The reduced filling time required to fill pre-fabricated prescriptions increased
pharmacist productivity and thus improved the profitability of dispensaries. Some
pharmacies used that increased productivity to promote their businesses. In August 1955,
a drive-in pharmacy boasted that "an average prescription is compounded and delivered 100 Ibid., 51.
102 Sonnedecker, History of Pharmacy, 313.
103 UBC-SM-CPBC, Box 12A-10, PPC Report, 11. 104 Sonnedecker, History of Pharmacy, 311.
in less than two minutes … all prescriptions are filled in full view of customers." The
pharmacist, Tony Lauglin, explained that "since drug houses put up many standard
prescriptions in tablets today, the pharmacist can count these in a matter of seconds."105
While the efficiency that Lauglin prized may have been good for short term
economics, the public were now viewing pharmacists in a different light. Rather than
expert compounders, the public saw pharmacists primarily as "pourers and counters."106
Despite increases in prescription volume, dispensing pre-fabricated products allowed
pharmacists to spend more time in the non-professional areas of the store. While this
increased their visibility to the public, that visibility was primarily in a non-professional
capacity. Pharmacists were seen as commercial retailers, with a technical role in
dispensing physician's prescriptions. Pharmacists' core competency of compounding no
longer occupied the center of their professional practice. Bound by a Code of Ethics that
restricted the scope of their practice, pharmacists struggled to develop new competencies.
Running parallel to a loss of public prestige, pharmacists also faced increasing
public criticism regarding the cost of prescriptions. A poll in 1953, found that 63.1 per
cent of people thought prescriptions were "higher than they should be." Manufacturer
Sharp and Dohme's survey found that 38 per cent of their sample believed that
"prescription prices have gone up faster in the past five years than have other prices."107
Prescription pricing was also a sensitive issue in Canada, prompting the federal
government to form the Special Committee on Drug Costs and Prices in July 1966.108 To
counter negative public reaction publicity campaigns were instigated by provincial
105 Robert Buerki, "The Public Image of the American Pharmacist in the Popular Press," Pharmacy in History Vol. 38 (1996): 75. 106 Elenbaas and Worthen, "Transformation of a Profession," 156.
107 Buerki, "Public Image," 69.
108 Canadian Pharmaceutical Journal Vol 99 No 7 (July1966): 28.
associations and private pharmacies. The Pharmaceutical Association of British
Columbia issued a pamphlet that attempted to show that prescription prices had remained
steady at the same time that other medical costs had risen steeply.109 Private community
pharmacies such as Jay's Pharmacy in Vancouver produced their own pamphlets that
showed the costs incurred to dispense a prescription.110 This public focus on prices
would have an impact on pharmacist's attempts to professionalize prescription pricing.
Although licensed as professionals, pharmacists operated under the economic
framework of a commercial enterprise. They had traditionally priced prescriptions by
adding a percentage to the drug cost to reach a retail price, a method used in most
commercial retail settings. It was hard for pharmacists to promote their professionalism
when they priced their professional services in the same way as Kleenex, paint or
tobacco. As early as 1957, Professor H.J. Fuller, Professor of Pharmacy at the University
of Toronto, advocated shifting the pricing of prescriptions to a system of cost plus
professional fee. The professional fee would cover all of the overhead costs incurred in
the dispensary and would bear no relation to the cost of the drug. This became known as
the Fuller Method. This method of pricing was not adopted quickly, by 1963 only ten
percent of pharmacies in Canada used this system.111 This reluctance can be attributed to
several reasons. Firstly, most pharmacies did not keep separate account records for their
dispensaries and thus would be unable to determine the overhead costs for the dispensary
alone. Secondly, pharmacists worried that, although this system would decrease the cost
to consumers for some prescriptions, others prescriptions would increase in price. Lastly,
109 UBC-SM-CPBC, Box 1-27, The Low Cost of Drugs, July 1967.
110 UBC-SM-CPBC, Box 1-24, The Facts about Prescription Prices, 1967.
111 David Thompson, "More Pharmacists to Price a la Fuller?," The Financial Post Vol 57 No. 14 (April 6, 1963): 11.
the public view that pharmacists were "pourers and counters" made it difficult to justify a
professional fee for what appeared to be a purely technical function.
Technical aspects had always been part of the pharmacist role but with the decline
in compounding, that technical role had simplified considerably. Pharmacists had
received university training in British Columbia since 1948 but their ethical code
prohibited them from fully accessing much of that knowledge. As a result, pharmacists
were seen by the public as overeducated and underutilized. This was not a new issue. An
editorial in the Pacific Drug Review in February 1950 had noted that a pharmacist "finds
himself in a sort of no man's land, charged with professional responsibility but denied the
right to exercise individual professional judgment."112 By the 1960s, pharmacists started
to worry that filling prescriptions could become a strictly technical function not requiring
the services of a pharmacist. In Kentucky, hospital administrators opposed a bill proposed
by pharmacists that would prevent non-pharmacists from dispensing medications in
hospitals.113 In Canada, the pharmaceutical manufacturer's policy of selling drugs to
hospitals for less than community pharmacies was seen as a threat by pharmacists. They
feared that low prices could encourage provincial governments to dispense government-
paid welfare prescriptions through hospital outpatient departments.114 Potentially this
could be accomplished by technicians rather than pharmacists. In British Columbia, many
hospitals did not have a pharmacist on staff in the 1960s. Eliot Freidson argues that when
professionals are seen as merely technical specialists, they will be given little autonomy
112 Buerki, "Historical Development," 70.
113 Ronald Akers, "The Professional Association and the Legal Regulation of Practice," Law and Society Review Vol. 2 No. 3 (May, 1968): 475.
114 John Bachynsky, "Pharmacy in a New Age – A Milestone Study," in Canadian Pharmacists Association 1907-2007 -100 Years of Leadership in Pharmacy (Ottawa: Canadian Pharmacists Association, 2007), 26.
or authority beyond their technical speciality.115 Pharmacists worried that they might be
downgraded from professionals to technicians.
The academic world still saw pharmacy as an incomplete profession, just as
Abraham Flexner had in 1915. In an article titled, "Incomplete Professionalization: The
Case of Pharmacy", Denzin and Mettlin use Carr-Saunders and Wilson's definition of a
profession as an "occupation which is based upon specialized intellectual study and
training, the purpose of which is to supply skilled service or advice to others for a definite
fee or salary." They further specify that professions organize themselves into
professional groupings, develop special codes of ethics, engage in formalized
recruitment patterns, establish formal institutions to transmit the knowledge of
the occupation, develop social organizations to insure the perpetuation of the
profession through time and finally, take on the characteristics of self-governing,
autonomous institutions.116
Denzin and Mettlin argued that pharmacy constituted an incomplete profession
because they failed to abide by the requirement of a profession that "you do not
advertise" and failed to recruit "truly committed persons who would … commit their
lives to the altruistic goals and values of the profession." They claimed that pharmacists
also failed to control the object of their profession, the drug, or create a "systematic body
of scientific knowledge which can only be learned by socialization in their own
institutions.117 The authors quote pharmacists as saying their "the professional profile is
hazy and soft."118 Hospital pharmacists referred to retail pharmacists as "garden hose
115 Freidson, "Theory of Professionalism," 126.
116 A.M. Carr-Saunders and P.A. Wilson, The Professions, (Oxford: Clarendon Press, 1933) quoted in Norman K. Denzin and Curtis J. Mettlin, "Incomplete Professionalization: The Case of Pharmacy," Social Forces Vol 46 No 3 (March 1968), 375.
117 Ibid., 376-7.
druggists", highlighting the non-professional nature of products sold in drugstores.119
Denzin and Mettlin recognized that pharmacists possessed some aspects of
professionalism, codes of ethics, formal education, and specialized skills as well as
segments, such as hospital pharmacy that did not advertise. To professionalize, the
authors claimed, pharmacists would have to stop treating drugs as a product and start
treating the dispensing of drugs as a service. In practical terms, this meant adding a
uniform service fee to the cost of the drug, rather than marking the cost of the drug up by
a percentage, a system paralleling the Fuller Method. Denzin and Mettlin felt that this
would be difficult as the public saw pharmacists as "counters and pourers" and
pharmacists lacked credibility with the medical profession in the goal to be seen as
"experts on drugs." They quoted the "American Druggist's" statement that "the public
recognizes that the pharmacist has considered himself a merchant and they think … a
prescription is a commodity, a product, so why not, they say, buy it at the discount
house." 120 While pharmacists were professionals in a statutory sense, many observers
saw them as businessmen more than health professionals.
Throughout the 1950s and into 1960s, pharmacist's professional moral continue to
decline. Deborah Savage argues that the success of an organization depends on having
"practiced organizational routines" that underlie the existence of their core competences
and capabilities. "No matter how brilliant the plan, an organization that has the wrong set
of complementary capabilities will be unable to implement it."121 In the 1960s,
pharmacists' practiced organizational routines had become "pouring and counting" while
the core competence for which they were trained remained compounding prescriptions.
119 Ibid., 376. 120 Ibid., 378. 121 Savage, "Professions in Theory," 133.
These "pour and count" activities, performed on a daily basis, now formed the capability
of the organization but were out of sync with their core competency. The legitimacy and
dependence underlining their authority in the past had been embedded in the core
competency of compounding prescriptions. This competency had been recognized as
specialized knowledge only acquired by pharmacists, qualifying it as a distinct
competency. No other group could compound prescriptions as well as they could. The
declining usefulness of this specialized knowledge diminished their claim to legitimacy.
Likewise, the public dependence on pharmacist's compounding skills diminished.
Neither legitimacy nor dependence could be replaced by pharmacists whose skills
appeared to be nothing more than "pouring and counting." The result was a diminished
reputation; therefore the pharmacist's fear that they had lost prestige was an accurate
assessment. To turn this loss of authority around pharmacists' dynamic capabilities would
be tested. Could they reconfigure their competencies to address the changes that had
occurred in their professional environment? The next two chapters explore attempts by
pharmacists in British Columbia, in the mid 1960s, to alter the dynamics of their
profession. Like pharmacists throughout North America, they were expressing concerns
about their profession's future.
British Columbia pharmacist, Ben Gant, echoed Emile Coderre (as quoted to start
this chapter), and in fact, went much further with his address titled "Pharmacy: A Dying
Profession." While Coderre worried that pharmacists were "losing … prestige", Gant
worried whether the profession would survive at all. Gant recognized that "the
professional function of the Pharmacist [had changed] from a manual art in which the
ability to compound mixtures and pills etc. established his professional identity, to one of
knowledge in the complete use of drugs and their inherent dangers." He believed that
pharmacists had "become vulnerable to those outside the profession who … sought to
immortalize the count and pour philosophy as the sole professional responsibility of the
Pharmacist." Gant knew that in order to survive, pharmacists had to change; "the
continued existence of society and any organization within it is dependent upon their
capability to adapt to any changes which may influence their environment." The changes
he envisioned would come with the acceptance that pharmacy "is no longer a manual art"
and its refocus on two areas where pharmacists should be responsible for drug
interactions, the dispensary for prescriptions and the front store for over-the-counter
drugs. Gant rejected the notion that "possible interactions and other therapeutic
misadventures … [were] the physician's responsibility." Pharmacists would be able to
"live up to our professional responsibility" only when they were allowed to utilize "this
knowledge to the benefit of those people in our community."122
The opening statement in the submission by the Study Committee on Pharmacy in
British Columbia to the Pharmacy Planning Commission (both reports to be examined in
detail in chapters three and four), contained the words that struck a familiar tone,
"Pharmacy is in trouble." The authors argued that all pharmacists would agree that the
public image of pharmacy had been "slipping for decades." Its professional status had
been chipped away as the profession remained "caught between the dichotomy of
commercialism and professionalism." Everyone, they declared, "is of one voice that
something must be done, and right now, if the profession is to survive." These
pharmacists were also concerned about another aspect of survival, recruitment of new
122 UBC-SM-CPBC, Box 13-21, Ben Gant Address, "Pharmacy: A Dying Profession."
members of the profession. Recruitment to the pharmacy program at the University of
British Columbia had fallen below the "level necessary to sustain the service which the
public has a right to require of Pharmacy" and this was because pharmacy had "lost its
lustre for the young." Although all pharmacists agreed that something needed to be
done, the committee believed that "there is no unanimity … as the methods to be
employed … as the instrument … for furthering the interests of Pharmacists."123 The
next two chapters will provide a case study that examines how pharmacists in British
Columbia attempted to reconstruct their profession.
123 UBC-SM-CPBC, Box 12A-12, Submission of the Study Committee on Pharmacy in British Columbia to
the Pharmacy Planning Commission January 1967, 1.
Chapter Three
It is important that the pharmacist should recognize that he has become a
Pharmaceutical Chemist with powers and rights in the province of British
Columbia and is a responsible professional person. Nobody need hire him;
no one undertakes to give him a position, but the Association and the
University have given him a Certificate that he may carry with him wherever
he may go, subject to the laws of the land wherever he may travel.
The Pharmaceutical Association of the Province of British Columbia (the
Association) was established as a corporate body, by the British Columbia legislature,
with the passage of The Pharmacy Act on April 20, 1891.125 The overall mandate of the
Association is to oversee the practice of pharmacy in British Columbia. Pharmacists
must be licensed with the Association before they are entitled to practice pharmacy in the
province. In 1966, when British Columbia pharmacists created the planning commission
that forms the basis of the case study examined in this thesis, the Association's
administration included a council of six councillors elected, by the membership, from six
geographical districts throughout British Columbia plus four elected from Greater
Vancouver. Paid staff included a Registrar/Secretary-Treasurer, an Executive
Secretary/Inspector plus four clerical staff. The councillors elected an executive
committee of five members, one of whom was elected president. The president
appointed three council committees, discipline, finance and legislation and the council
selected six committees, drug advisory, economics, education, health services,
professional relations, and public relations. Special committees were appointed as
124 UBC-SM-CPBC, Box 12A-10, PPC Report, 139.
125 Raison, Brief History of Pharmacy, 46. In 1974, the name was changed, by statute, to the College of Pharmacists of British Columbia. It still exists under that name. The British Columbia Professional
Pharmacists Society then took over the title of British Columbia Pharmacy Association. The College is mandatory, the Association is voluntary.
needed for specific projects. The council appointed a Board of Trustees, four CPhA
delegates and recommended a board of examiners to be officially appointed by the
Lieutenant-Governor.
The federal government is responsible for approving new drugs for sale in Canada
through the Food and Drugs Act and Regulations in which they designate a list of
prescription-only drugs (Schedule F & G).126 Provinces also develop prescription-only
drug schedules, which must include all Schedule F & G drugs, but which may also
include any other drugs, as deemed necessary by the provincial association.127 In 1966,
British Columbia's Pharmacy Act included Schedule A, part I which listed prescription-
only drugs (including all Schedule F and G drugs), Schedule A, part II which listed items
that could be sold without a prescription but which required a signature in a poison
register, Schedule A, part III which listed over-the-counter (OTC) drugs that could only
be sold in pharmacies and Schedule B which listed drugs that could be sold by any
person. Drugs that were listed in the federal government's Proprietary and Patent
Medicine Act could also be sold by any person.
In addition to their mandatory membership in the Association, many pharmacists
belonged to voluntary local professional pharmacy organizations. These included the
Lower Mainland Pharmacists Association (LMPA), Okanagan Pharmacists Association
and the South Vancouver Island Pharmacists' Association (SVIPA). In September 1965,
the SVIPA gave notice to the Association of a resolution which they subsequently
presented to council in November. It requested that a province wide committee, made up
of four practicing pharmacists from each district, be set up to provide a "thorough
126 Department of Justice,(June 19, 2010).
127 Thus, when a drug is removed from Schedule F or G by the federal government it does not become available without a prescription until it is removed from the provincial schedule.
analysis of the situation in pharmacy especially regarding the security of the profession
and the protection of the public health." This resolution was received positively by
council and they recommended that a Pilot Committee of eight members be formed - two
employers and two employees from each of the SVIPA and LMPA. The pilot committee
would expand upon the areas of reference referred to in the resolution, as well as
recommend whether a commission approach or a committee representative of all areas of
the province should be adopted. Council appointed an outside chairman for the pilot
committee and a meeting was arranged at the offices of the Association for March 9,
On February 28 1966, Association councillor for Victoria, Jack Johnston,
informed Association Registrar Douglas Denholm that the SVIPA committee members
objected to the terms set out by the Association on four grounds, the selection of an
outside chairman, the terms of reference, the expectation that the pilot committee would
report to the Association and the site of the meeting (the Association offices).129
The council decided that they were willing to accede to all points with the exception that
the Pilot Committee must report back to the Association. In the view of council, this was
an Association funded and appointed committee and was therefore responsible to all the
membership, not just themselves. Subsequent to that decision, the SVIPA and LMPA
informed council that it had decided to continue meeting "at an informal level" outside
the jurisdiction of the Association. All expenses would be paid out of their own
128 UBC-SM-CPBC, Box 23-38, Resolution of council for the consideration of the BCPhA Annual Meeting, June 1966, 160-161.
129 UBC-SM-CPBC, Box 12A-9, Letter to BCPhA council by Registrar Denholm, March 3, 1966.
130 UBC-SM-CPBC, Box 23-38, Resolution of council for the consideration of the BCPhA Annual Meeting,
Renamed and reformulated as the "Study Committee on Pharmacy in British
Columbia" (Study Committee), - nine additional members from around the province were
added- the committee proceeded to carry on without support from the Association. In the
report they produced, the Study Committee stated that they had examined all provincial
legislation pertaining to professions in British Columbia and met with individuals and
groups throughout the province. Their twenty page report detailed the problems that
faced pharmacists which, they believed, centered on issues such as economics,
negotiating and bargaining, employer-employee relations and enforcement of standards
related to unethical trade practices. These were problems, the committee believed, that
were beyond the scope of the legislative authority that the Pharmacy Act gave the
Association. This lack of jurisdiction had created a communication gap between
pharmacists and the Association. They quoted a LMPA committee report that "there
exists the feeling that the association offices operate in an ivory tower atmosphere."131
The solution proposed by the Study Committee was a second pharmacist
organization (the Society) that would deal exclusively with the problem areas that they
had previously discussed. This would allow the Association to concentrate on its role as
"protector of the public interest" and leave the Society to protect the interests of
pharmacists.132 The report outlined a detailed plan for the Society, including potential
districts, voting procedures and committee structures. The Study Committee suggested
that the Association could collect mandatory fees, in addition to the annual Association
fees, that could be passed on to the Society. Thus, although the Society would be
June 1966, 161.
131 UBC-SM-CPBC, Box 10-32, Report of Study Committee on Pharmacy in British Columbia (hereafter SC Report), 4.
132 UBC-SM-CPBC, Box 10-32, SC Report, 10.
voluntary, the fees would be mandatory. Additionally, both organizations could share
office staff and offices as well as hold joint annual meetings. Linkage, between the two
organizations, had the potential to create a conflict of interest. Since the Association was
mandated by the legislature to safeguard the public and the Society looked after the
interests of pharmacists, their goals might not always be compatible. Finally, the new
Society would set up a permanent Planning Commission to deal with problems in the
long term and formulate new standards of practice and a Code of Ethics.133 Ethics are an
example of a potential conflict of interest. An ethical code is created to ensure that
professionals act in the best interest of the public; the Society was mandated to look after
the interests of pharmacists.
The interactions that surrounded the SVIPA's resolution to the Association
highlight the divisions amongst British Columbia pharmacists at this time. The SVIPA
was not looking to work from within the Association saying that "it was necessary to
protect the council and the Association by not involving the Pharmacy Act or its
custodians in any official capacity."134 Their report shows that they believed that the
Association played a central role in pharmacists' problems. For that reason they wanted
the freedom to investigate these problems, free from any Association input or control.
When the Study Committee's report was released it revealed that their goal was a new
pharmacy organization, the Society, designed to take over the functions that they believed
the Association would not or could not address. While they did envision a planning
commission it would be part of, and controlled by, the Society, not the Association. They
did not want to report to the Association because they felt their responsibility was to the
133 UBC-SM-CPBC, Box 10-32, SC Report, 12.
134 UBC-SM-CPBC, Box 10-32, SC Report, 1.
membership of the Association, not council. They wanted to, and did, report to the
Association only when they had finalized their report and believed they had majority
support from pharmacists in the province. Jack Johnston, councillor for South Vancouver
Island, made it clear that some members of the SVIPA wanted their committee to retain
independence from the Association, stating "right from the start there were certain
members of the SVIPA who wanted to keep this entirely separate from council and they
pressed that."135
In June 1966, the Study Committee invited council to a presentation of their
findings.136 At that meeting the Study Committee presented their report and requested
that council approve their proposals in principle and to direct the Study Group to prepare
a draft constitution and bylaws of a second pharmacy association. Council declined to
respond citing two reasons. Firstly, they noted that, although they spent considerable
time examining the report, the substantial proposals they contained required more time.
Secondly, they wanted advice from their solicitor on both requests. They did promise to
discuss the report further at council meetings scheduled at the end of June, after the
closing of the Association's annual meeting.137
At the Association's annual meeting, held immediately after the Study Committee
presented their report, council tabled a four page summary of the previous seven months
activities surrounding the resolution. Council expressed that they were impressed with the
report but were somewhat dismissive in their praise. "It is obvious" they said, " that a
great deal of thought has been directed by the pharmacists on the Study Group to many of
135 UBC-SM-CPBC, Box 23-38, Discussion on SVIPA-LMPA Pilot Committee, BCPhA Annual Meeting, June 1966, 110.
136 UBC-SM-CPBC, Box 12A-12, Letter from D. Denholm to C. Hoffman, June 7, 1966.
137 UBC-SM-CPBC, Box 23-38, Resolution of council for the consideration of the BCPhA Annual Meeting, June 1966, 162.
the problems facing our profession, many of which are currently under study by Council
or Committees of the Association" (emphasis added). Council stated their belief that the
solution proposed by the Study Committee, namely a new pharmacy organization, was
"based on inconclusive evidence and is premature." They did not believe that a new
organization could solve pharmacists' problems more easily than they could. Rather than
accept the findings of the Study Committee, council submitted their own resolution for a
Planning Commission to the annual meeting. Citing "now evident widespread interest",
council entered a motion that "immediate steps be taken to appoint a Planning
Commission" designed to "produce the answers required to ensure the profession's
future, if not its very existence."138
The language in their report reveals council's attempts to take back control from
the Study Committee. Although nominally praising their report, they diminished its
importance by stating that the problems that they were studying were already being
handled by the Association. The Study Committee's report was presented to council as a
final report. They believed that their province wide committee had done a thorough job
and had presented the solution to pharmacists' problems. The solution would be the
formation of a second pharmacy organization and implementation should proceed as soon
as possible. The Association disagreed; the solution proposed was unsatisfactory and
premature. A Pharmacy Planning Commission (the Commission), under their control,
was the only method that would produce a satisfactory answer. It appears that the
disagreement was not whether action of some sort was needed, but the form that action
should take. The lines of battle were drawn and as the annual meeting progressed, the
138 UBC-SM-CPBC, Box 23-38, Resolution of council for the consideration of the BCPhA Annual Meeting, June 1966, 162-3.
membership would be called on to decide the mechanics of the actions that would be
Members of the Association provided their input at annual meetings through
Syndicate Discussions; a procedure that had been in use since 1963. Members of the
Association participated in an appraisal of various areas of pharmaceutical practice "with
a view to providing guidance and leadership to the Association."139 In 1966, council's
resolution was assigned to Syndicate Two, under the title "Pharmacy Organizations in
B.C." Four meetings were held over three days, with 35-45 pharmacists at each meeting.
The two main topics of discussion were council's resolution and the Study Committee's
recommendation of a second pharmacy organization. The syndicate voted to support
council's resolution with four dissenting votes, three of which came from members of the
Study Committee.140 It was noted that "urgent study was required." Discussion about a
second pharmacy organization brought "lively discussion." The majority wanted
continued study, to supplement that done by the Study Committee, jointly with the
Association but some wanted the Study Committee to continue separately and only liaise
with the Association. Some were opposed to the immediate formation of the new
organization until it had been carefully studied in consultation with legal counsel.
It was generally agreed that "urgency, extreme urgency" was required in the
follow-up of the Study Committee report and that council and the syndicate saw
pharmacists' problems in the same light. The solution was not unanimous with some
feeling that the "formation of a separate organization for the welfare of Pharmacy could
have severe repercussions and public criticism." In the final meeting of the syndicate, it
139 UBC-SM-CPBC, Box 13-4, Syndicate Discussions, BCPhA Annual Meeting, June 1964.
140 UBC-SM-CPBC, Box 23-38, Syndicate Discussion #2, BCPhA Annual Meeting, June 1966, 186.
was moved and carried that the Commission should include the report of the Study
Committee in its deliberations. The last speaker in the meetings was John Turnbull,
executive director of the CPhA, who asked the delegates "to bear in mind that the rest of
Canada was watching us very carefully."141
When the time came to address the council's resolution amongst the full
Association membership, discussion was lengthy. Five members of the Study Committee
brought proxies with them, giving them twenty four votes of the eighty that would be
cast. Syndicate Two's amendment that the Commission should consider the report of the
Study Committee was passed, after some discussion. Much more discussion centered on
the amendment proposed by Stan Fyfe, a member of the Study Committee. His
amendment put significant time restrictions on the completion of the Commission. It
stipulated that the Commission be formed by October 1966 and report their findings to
council and all interested pharmacists by March 1967. Further, the amendment stipulated
that the members of the commission and its terms of reference "be acceptable to
practicing pharmacists through district meetings." This amendment prompted
considerable discussion. Many argued the time restrictions would hamper the
effectiveness of the committee. As one member noted "you would certainly be tying
council's hands by providing time limitations." Many pharmacists were concerned about
the practicality of canvassing the pharmacists in such a large province, within the
prescribed time period.142
Objections to time restrictions and the ratification of the commission members
and terms of reference were all made by members of council. Gant's determination that
141 Ibid., 186-7.
142 Ibid., 190-2.
these restrictions showed a lack of confidence in council was probably quite accurate.
Those who spoke in favour of the motion were all members of the Study Committee.
Charlie Burr summed up the general feeling of that faction:
I think time has gone on for years where we have sat in on committees. We have
had results of surveys, and we have a lot of basic facts to go on and I think we are
putting pressure on ourselves as well as Council and it is absolutely essential with
some of the main problems that Pharmacy is going to be faced with that we come
up with definite plans for the future. … Our grass roots are hollering for it.143
The amendment, and thus the resolution, was finally passed with a margin of
fifty-six votes to twenty-four. Clearly, the membership was divided on the issue of time
and ratification restrictions, not on the concept of a planning commission or the inclusion
of input by the Study Committee. The majority agreed, however, that the issues were
urgent and that the commission should have grass roots support and input. The SVIPA
and the Study Committee had challenged the authority of the Association. Although they
had not been successful in achieving immediate implementation of their preferred
solution, the Society, they were able to ensure that all aspects of the Commission would
receive grassroots input, in a timely fashion.
On the last day of the Association's 1966 annual meeting, council convened all
afternoon to resolve the Commission's logistics including the selection of a chairman and
commission members as well as the drafting of terms of reference.144 The choice of
chairman presented the least difficulties since the resolution had put that fully in the
hands of council. After considerable discussion on the size and make-up of a search
committee it was decided that the Executive Committee should conduct the search and
143 Ibid., 191-3.
144 See Appendix E for final wording of the Pharmacy Planning Commission resolution.
submit their candidate to council in September for approval.145 The more complicated
and contentious issue was developing terms of reference for the commission. The tension
in this discussion was between councillors who wished to dictate the direction of the
Commission and those who feared that the membership would not accept their authority.
In the end, the compromise suggestion adopted was that the Executive Committee would
draw up specific terms of reference using the Registrar's reports, committee reports and
recommendations from Association members and study groups. A draft of their terms of
reference would be edited and approved by a workshop of ten non-council pharmacists
from all districts, prior to final ratification by council in September. The workshop did
take place on August 28 with nine non-council pharmacists taking part and producing the
fourth draft of the terms of reference.146
The final decision was the make-up of the Commission members. Consensus was
reached that an ideal commission would include an employee, employer, government and
hospital pharmacist plus an educator belonging to the Association and one person
representing the other health professions.147 A motion was passed that the Commission
should be made up of no less than four or more than six persons, to be selected by the
Executive committee and ratified by council.148 This went directly against the resolution
passed at the annual meeting which specified that "this Planning Commission and the
terms of reference be acceptable to all practicing pharmacists through district
meetings."149 In an information letter, on the progess of the Pharmacy Planning
Commisson, sent to all members of the Association on August 15, 1966, the membership
145 UBC-SM-CPBC, Box 12A-10, Notes from BCPhA Council meeting, June 26, 1966, 60.
146 UBC-SM-CPBC, Box 13-23, Notes from BCPhA Council meeting, August 28, 1966.
147 UBC-SM-CPBC, Box 12A-10, Notes from BCPhA Council meeting, June 26, 1966, 61.
149 See Appendix E for copy of resolution.
was told that the "suggestions for the membership of the Commission will be prepared by
the Executive for presentation to the District Meetings."150 It appears that council had
relented and did allow some input from the districts on the makeup of the Commission's
District meetings were organized for the membership between September 1st and
8th,1966. This was to discuss the terms of reference and potential members of the
commission. On September 11, council held a special meeting to finalize the chairman,
membership and terms of reference of the commission. The Executive Committee gave a
full account of their search for a chairman and council ratified their candidate, Dean
E.D.MacPhee. Input from the district meetings were incorporated into the draft produced
by the August pharmacist workshop and a finalized version of the Terms of Reference
was passed by council. Twelve candidates for membership on the committee were
discussed, with the consensus being that the most important criterea would be "the ability
to understand and interpret the problems of pharmacy." Since Dean MacPhee had
requested that the commission have only three members, their original decision to have
between four and six members was abandoned. Council voted by secret ballot and the
new commissioners were Murray Dykeman,151 John Dyck, and Trevor Watson. The
Pharmacy Planning Commission was now established, one month ahead of the schedule
imposed by the annual meeting's resolution.152 Although council had been irritated by
the constricting and untrusting nature of the resolution passed at the annual meeting, it
did abide by the basic intent of the resolution in the selection of the Commission's
150 UBC-SM-CPBC, Box 13-23, Letter from BCPhA to membership, August 15, 1966. 151 Murray Dykeman had been Council candidate for chairmanship of the Pilot Committee that never happened. 152 UBC-SM-CPBC, Box 1-23, BCPhA Council Meeting Minutes, September 11, 1966.
membership and terms of reference, acknowledging the importance of grass roots
Earl MacPhee, chairman of the Commission, had been Dean of Commerce and
Business Administration and Dean of Financial and Administrative Affairs at U.B.C and
also taught in the Faculty of Commerce. MacPhee previously had a career in business as
Managing Director for various British companies from 1929 to 1950; he had no previous
experience with pharmacy but all three commissioners were pharmacists. The
Commission travelled around the province meeting with pharmacists in each of the seven
Association districts. Twenty eight meetings were held in eighteen locations with a total
attendance of 443 pharmacists or thirty-seven percent of the 1210 registered pharmacists
in British Columbia. Attempts were made to schedule meetings that maximized
attendance; taking into consideration store hours and geography. Attendance was evenly
distributed between urban and rural areas while employers (sixty-five percent) were over-
represented compared to employees (twenty-five percent).153 The striking difference in
attendance between employers and employees may have had several sources. Employers
were likely in the prime of their career and certainly had a greater financial interest in the
outcome. Also, many stores were two pharmacist operations; it would have been more
likely that the employee would have been left to run the store while the employer
attended the meeting. Nonetheless, it is clear that pharmacists in British Columbia
supported the Commission and, therefore, did feel there was an urgent need to address the
problems facing the profession.
153 UBC-SM-CPBC, Box 12A-10, PPC Report, p.iii. Note: Ironically, District One, South Vancouver Island, had the second lowest attendance (32%), despite being the driving force behind formation of the Commission.
In addition to the pharmacist meetings, the Commission received input from many
other sources. Written submissions were received from thirty-one individuals, many of
them pharmacists as well as the Hospital Pharmacists, the Faculty of Pharmacy and the
Study Committee. Additionally, they consulted with forty-eight individuals, including
Association council members and staff, health administrators, academics, provincial and
federal government officials, and the wholesale drug industry. They met with physicians,
veterinarians, nurses, teachers and consulted with various pharmacy organizations. The
Commission also examined thirteen reports and surveys prepared in British Columbia
since 1961 including submissions by the Association to the Royal Commission on Health
Services (Royal Commission) in 1962 and reports on Continuing Education (1965),
Dispensing Costs (1965), the Commercial-Professional Balance (1965), student
enrolments (1966) and the Welfare Drug Program (1966).154
The Commission polled the opinions of a wide cross section of pharmacists and
the wider health care community. Their report shows that they listened closely to the
views of pharmacists. The authors noted a "growing feeling of discontent and
unhappiness amongst Pharmacists … in such proportions that could not escape our
attention."155 The opinions of many different aspects of pharmacy were considered. For
example, students were noted as primarily being concerned with their professional
image.156 In terms of influence, however, two groups seem to predominate. The
Commission noted that the "opinions expressed were primarily those of the ownership
group" because, as we have seen, the majority of those attending were employers.157
154 Ibid., iv-vii.
Their concerns dominated the commission's five recommendations that involved
commercial considerations. The second group who were able to exert considerable
influence was the representatives of the Faculty of Pharmacy. Many of the seven
recommendations on educational reform came through input by the Dean and other
faculty members.
The Commission report notes that the thirteen reports and surveys examined had
"not had time to fructify in any major way."158 They also note that investigations had
been carried out by other Canadian pharmaceutical organizations. Association president,
Bernie Brown, had made the Association's position clear that they did not want a report
that merely summarized all previous reports. Rather, they wanted to achieve a "searching
look at our own profession."159 The commissioners were aware of the hopes that British
Columbia pharmacists had for practical solutions to their problems. They hoped that the
Association would "debate, commend or, if necessary, condemn such findings" because
they were "the problems of the next ten or even twenty years" more the "the issues of
today." Everybody involved in this Commission seemed to be on the same page, this was
a call to action, not an opportunity to create another study to be left to collect dust on a
The report produced by the Commission was organized into thirteen chapters.
Chapter One presents the thirty-five recommendations of the Commission, categorized by
chapter.161 Recommendations fall generally into three categories, those that increase the
scope of practice for pharmacists, those that increase the professional image of
159 UBC-SM-CPBC, Box 12A-10, Notes from BCPhA Council meeting, June 26, 1966, 65.
160 UBC-SM-CPBC, Box 12A-10, PPC Report, v-vi.
161 See Appendix F for copy of recommendations.
pharmacists and those concerned with economics. Many of the recommendations can be
viewed within more than one of these general categories, education was critical to both
increasing their scope of practice and their professional image. Pharmacists' attempt to
increase their scope of practice was also a key factor in their quest to improve their
professional image.
Chapter Two gives a broad history of pharmacy from Babylonian times to British
Columbia in the twentieth century, then proceeds to recent statistics relating to pharmacy;
new students admitted to pharmacy in each province, statistical relationships between
pharmacists, pharmacies and the general population in each province and the number,
total value and individual cost of prescriptions filled in Canada, as well as the number of
pharmacist licenses issued in British Columbia over the previous ten years. The next
section of this chapter looks at pharmacists' image from various points of view, the
University of British Columbia, pharmacists, students and private enterprise. The last
section looks at the relationship between the Faculty of Pharmacy and the Association.162
Each of the last eleven chapters covered a different area of concern to
pharmacists. The topics covered were as follows:
The Role of the Pharmacist
Professional and Commercial Services
Pharmacist Utilization and Remuneration
Pharmacy Organization
Economic Considerations
Relationship to Other Health Professions and Health Care Plans
Relationships with Government
Relationships with Suppliers
Chapter Thirteen
Legislation and By-Laws163
162 UBC-SM-CPBC, Box 12A-10, PPC Report, 1-16.
Each of these chapters was divided up into sub-categories within the broader topic.
The Commission noted that the loss of compounding and the concurrent rise of
prefabricated medications had "affected our function." Along with this loss was a
"lessening of our own respect for the art which was the basis of pharmacy practice for the
last three decades. The application of merchandising techniques to the pricing … of
medications has affected both our identity and function."164 The Commission sought to
replace the loss of that compounding function, which had previously constituted
pharmacists' core competency, by expanding their scope of practice as medication
The Commission had noted that physicians were being overwhelmed by the
volume of drug information sent to them by manufacturers regarding the adverse effects
of drugs, but they were also told "that the physicians were not really expecting the
pharmacist to be his consultant on drugs."165 It would take time to increase their scope of
practice by positioning themselves as drug consultants to physicians. It would not be
possible until pharmacists could demonstrate to physicians that they possessed legitimacy
through specialized knowledge. The ethical prohibition on labelling prescriptions with
composition was still in effect and this would make it difficult to extend their
consultation role to prescription medications.166 This prohibition involved a tacit
agreement between pharmacists and physicians; an agreement that pharmacists did not
want to unilaterally alter. Robert Buerki has argued that pharmacists are more self-
conscious about their public image than other health professionals: a claim that, he says,
166 Pharmacists would not routinely label prescriptions with their composition, without physician permission, until 1972. They only started to do so after receiving the support of physicians.
sociologists have put down to a "massive inferiority complex borne of a functional
subservience to medicine."167 That lack of confidence may have inhibited their will,
despite the fact that, as an independent licensed professional, the agreement was not
The Commission stated that "although not in a position to diagnose or prescribe,
the pharmacist often learns early of health problems and situations, and is well equipped
to advise the patient pertaining to the particular way in which medicine should be used or
recommend that self-treatment be discontinued and medical advice sought."168 The
members consulted felt that "pharmacists should become consultants to the public about
the use of drugs in their health needs."169 Pharmacists would be able, because of their
training, "to evaluate and advise, to create proper thinking about self-medication."170 The
Commission therefore developed recommendations that focused on increased pharmacist
involvement in counselling customers, now termed patients, in selecting appropriate
over-the-counter (OTC) medications and the education needed to facilitate that
One of the obstacles that pharmacists faced, as consultants on OTC drugs, was the
physical layout of most drugstores. The general feeling amongst pharmacists was that
"there was no professional reason to promote the use of such items, as they are not just
merchandise, but are potent drug forms, required by law to be sold only under the
supervision of a pharmacist." The Commission found that these products were sold, in
most cases, in self-service areas of the stores and were promoted in a similar manner to
167 Buerki, "Public Image," 72.
168 UBC-SM-CPBC, Box 12A-10, PPC Report, 22.
other non-professional drugstore products.171 Dean Matthew, from the Faculty of
Pharmacy, pointed out that "it is difficult to distinguish the interior of the average
pharmacy from a super market. All of those items which come with the legal definition of
drugs might easily been segregated in a clearly marked area."172 The Commission
recommended that OTC items that were restricted to sale in a pharmacy (Schedule A part
III) be "removed from public access and placed within an area under the personal
supervision of a licensed pharmacist."173 Their idea was to create a professional area
inside the pharmacy. Customers would leave the non-professional area of the drugstore
and enter a separate professional "office" that housed the dispensary and OTC drugs.
The Commission noted that "idealists have told us that pharmacy must divest
itself of its commercial involvement if it wishes to survive as a recognized profession."
This solution was not realistic; "the drugstore is here to stay." The practical solution lay
in the "separation and identification of the professional aspects."174 In focusing on the
physical aspects of the distribution of drugs, the Commission says, the pharmacist has
"lost sight of his responsibility to protect and advise the public on the use of drugs."175
Provincial legislation gave pharmacists the exclusive right to sell these medications
(Schedule A Part III) and along with this monopoly came the responsibility and
opportunity for pharmacists to use their training. If pharmacists failed to provide
professional consultation to the public when they purchased OTC medications, there
could be no justification for the retention of their monopoly. Expanding their drug
consulting role in this manner did not impact directly on the pharmacist-physician
171 UBC-SM-CPBC, Box 12A-10, PPC Report, 35.
173 Recommendation One, Appendix F.
174 UBC-SM-CPBC, Box 12A-10, PPC Report, 49.
relationship and was one that pharmacists believed was necessary and desired by the
public. It had the added advantage of being provided free of charge to the public.
The Commission made a number of other recommendations that would
complement the removal of pharmacy-only OTC medications from public access. They
recommended that if a pharmacy locked the professional area of the store, the pharmacy
should still be able to sell non-professional products, without a pharmacist being on duty.
This would allow one pharmacist stores in isolated areas to comply with the
recommendation while still serving the public with non-professional products and
services.176 A second corollary recommendation was the restriction on the advertising of
pharmacy-only OTC products. Since advertising was best handled at a national level,
because of the countrywide nature of many company's advertising campaigns, it was
recommended that the Association request that the CPhA lobby the Food and Drug
Directorate to tighten advertising controls on these medications. The Commission felt
that OTC drugs should not be advertised in the same way as patent medicines, sold by
non-pharmacies.177
The Commission recommended that inspections by the Association be
improved.178 In some areas of the province, the Commission was told, non-pharmacies
were openly selling pharmacy-only OTC's. This practice was a direct challenge to the
monopoly granted to pharmacists. Since the Association was responsible for enforcing all
provisions of the Pharmacy Act, "our inattention to proper enforcement could well result
in a loss of authority in this area." 179 If the Commission's recommendation to restricted
178 Recommendation Nineteen, Appendix F.
179 UBC-SM-CPBC, Box 12A-10, PPC Report, 36.
access of pharmacy-only OTC's was enacted, while at the same time they were readily
available in non-pharmacies, the public could reasonably question the necessity of the
The Commission recognized that increasing the amount of time that pharmacists
spent counselling the public on their OTC selections could have an impact on their other
professional duties. For that reason, the Commission recommended that a category of
Non-Professional Assistants (NPA) be created to handle clerical duties in the pharmacy.
This could have multiple benefits for the pharmacists since his "time will be more
productive and more rewarding if used to advise the public on the use of medicines than
if used to type labels and make entries in registers and reports."180 To achieve maximum
professional efficiency, pharmacists "must start to utilize lay help to assist … in
providing this professional service."181 Creating a category of Non-Professional
Assistants would allow pharmacists to control the professional functions that were
restricted to pharmacists as well as those duties that could be done by non-professionals.
It was hoped that by decreasing the non-professional duties performed by the pharmacist
their professional image would increase as well as make pharmacy more attractive to
potential recruits.
In order to be better qualified to provide increased counselling services to the
public, pharmacists needed to update the education they received. The Commission
recommended that the Faculty of Pharmacy become more aware of the "needs of
community and hospital practice and re-orient themselves to the importance of these
aspects of the practice of Pharmacy."182 Specifically, it was recommended that the
physical sciences be reduced and a greater emphasis be placed on biological sciences.
This would enable the student to be better prepared for changing patterns of patient care.
The study of Pharmacognosy should be drastically reduced and the student should be
exposed to clinical practice while an undergraduate.183 The clinical practice should be
practical and involve members of the profession in community practice.184 The Faculty
of Pharmacy presented a brief to the Commission in which they expressed the concern
that there had been a "lack of active study within the profession to define its role in
society and to clarify the present and future occupational roles of the pharmacist."185 It
was noted that pharmacy was the only health profession that did not have a clinical
component in its education. "If the pharmacist is to be a participating member of the
health team, he must have clinical exposure and experience."186 While it may be difficult
for pharmacists to quickly gain the trust of physician's, this clinical training could have
immediate effects on their interactions with the public, through counselling on OTC
It was recognized that education through the Faculty was primarily focused on
future pharmacists and that this did not address educational deficiencies of practicing
pharmacists. Additionally, it was recognized that pharmacy was a constantly changing
profession. For these two reasons, it was recommended that the existing continuing
education program, deemed to be inadequate, should be improved.187
182 Recommendation Eleven, Appendix F.
183 Recommendation Twelve, Appendix F.
184 Recommendation Thirteen, Appendix F.
185 UBC-SM-CPBC, Box 12A-10, PPC Report, 77.
187 Recommendation Sixteen, Appendix F.
If implemented, all of these recommendations would help expand pharmacists'
scope of practice and legitimize a new core competency as medication consultants. This
would eventually require that pharmacists counsel patients on OTC drugs and
prescriptions as well as acting as a drug consultant for physicians. In the short term, OTC
drug counselling would provide the first step along the path to this goal. The second two
goals could only be achieved after their educational goals were completed and their
ethical code was updated. A core competency as medication consultation experts was an
essential ingredient in pharmacists' goal to improve their professional image.
The Commission also recommended some measures that could directly enhance
the professional image of pharmacists. Improvements in public relations with the public,
more pharmacist control of the Association and ensuring that every hospital in the
province could access pharmacy services would all help pharmacists' image. A concerted
effort to recruit quality candidates to the Faculty of Pharmacy would pay future
dividends; up until this time the dropout rate had been very poor and this had been
blamed on failure to recruit quality candidates. New district organizations were
encouraged but more importantly, the Commission recommended the formation of a
Society that "would concern itself with the promotion of Pharmacy in the interests of
pharmacists." The Commission also endorsed the Fuller Method of prescription pricing;
cost plus professional fee. To aid this method of pricing, they recommended accounting
systems that would allow a pharmacy to isolate the costs incurred by the dispensary from
the costs of the entire drugstore.
The Society would also be instrumental in advancing the economic issues
recommended by the Commission. Mechanisms to increase administrative awareness,
carry out negiotiations between pharmacists and manufacturers, wholesalers and
government would fall under their jurisdication. Also permanent employer-employee
committees that would deal with employment issues and salary would be their
responsibility. This would leave the Association responsible only for the provisions of
the Pharmacy Act.
All of the effort expended by the Commission and its participants would be
wasted if pharmacists failed to act upon their recommendations. Chairman MacPhee had
a clear message for pharmacists; they had been given rights and powers by legislation but
the direction of their professional growth was in their hands. They should not expect to
be granted authority they had not earned. It was in their hands to take the
recommendations of the Commission and either accept, modify, or reject their findings
and create the profession they wanted.
Chapter Four
We pharmacists sometimes feel that we are alone in facing the
increasing complexities and demands of a society whose attitudes
and complexion have undergone such marked change in the past
decade. There is good reason to believe that the fault is our own by
not keeping pace with society in its rapidly increasing degree of
sophistication.
BCPhA Registrar Douglas Denholm, June 1967188
The Pharmacy Planning Commission submitted their report to the Association's
annual meeting in June 1967, having completed their investigations within the time frame
stipulated the previous year.189 MacPhee summarized their main findings and finished by
saying, "some of our findings will be acceptable; some of the arguments which have been
advanced will cause some debates over the year ahead."190 Pharmacists were assigned
the task of evaluating the recommendations, through the use of syndicate discussions.
They took their role seriously, with meetings held over two days. Although some
objections were raised, the pharmacists attending the syndicates were in favour of the
majority of the thirty-five recommendations. The two recommendations that placed
highest in priority were the removal of OTC's from public access and the formation of
new pharmacy organization, the Society. These two recommendations signalled
pharmacist's intentions to use the Commission to increase their scope of practice by
developing a new core competency as well as increase their professional status. Many
other recommendations would help with both those goals.
A special council committee was struck, in July 1967, to investigate removing
OTCs from public access. The committee was asked to define the terms "public access"
188 UBC-SM-CPBC, Box 23-38, Registrar Report, D. A. Denholm, BCPhA Annual Meeting, June 1967, 84.
189 This timeframe seems to have come to as surprise to Chairman MacPhee who noted in his report that "I had not realized that your intent was to complete this study in a period of eight months."
190 UBC-SM-CPBC, Box 23-38, Report of Dean MacPhee, BCPhA Annual Meeting, June 1967, 135.
and "personal supervision" as well as prepare a list of the drugs that would be affected.
A motion to amend By-law 44(3) was tabled at the March 1968 council meeting as
All drugs and preparations … restricted to sale by licensed pharmaceutical
chemists shall be … offered for sale in an area
of the pharmacy which is under the personal supervision of a licensed pharmacist and not open to public access.191
The key phrase was "not open to public access" as it was interpreted to mean that a
physical barrier would prevent the public from access to these drugs. The professional
area would occupy a separate room; a professional office within the pharmacy. When
patients entered this "office" they would be aware that they were now accessing health
professionals. All non-professional activities would take place outside of this office.
There was some opposition to this amendment for a number of reasons. Firstly, the
renovations necessary would entail considerable expense for most pharmacies, as well as
increased staffing and a potential loss of sales (estimated at 25%). Secondly, the public
might object "on the basis that it reduced competition." Thirdly, there was concern over
an adequate phasing in period. Councillor Dyck reminded council that this
recommendation had been placed in the Immediate Action category in July 1967 but, in
view of the objections, it was included as a Syndicate discussion at the 1968 annual
The Syndicate was in favour of the amendment but advised council that they
should "proceed with caution realizing more research, public relations, and inter and
intra-professional relations are needed at this time."193 The committee agreed that
191 UBC-SM-CPBC, Box 27-1, BCPhA Council meeting, March, 1968, 39.
192 Ibid., 38-42.
193 UBC-SM-CPBC, Box 10-33, Syndicate Two Report, BCPhA Annual Meeting, June 1968.
research needed to be done to "establish the fact that the proposal was essential to the
public interest and not inimical to the pharmacist's interest."194 The research would be
done by a literature search for adverse reactions from OTC drugs and inquiries with the
B.C. Medical Association, who had done a similar study. The result of their research was
released to the membership at the June 1969 annual meeting. No evidence could be
found of adverse reactions that had resulted from the indiscriminate use of OTC drugs.
Although they believed that adverse reactions did exist, but were not documented, they
were forced to recommend that council not proceed with legislative removal of OTCs
from public access. Pharmacists did not have the authority to restrict access to OTC
drugs because they could not demonstrate that it would advance the public's interest.
The committee recommended that efforts be continued to educate pharmacists on
the professional distribution of OTC drugs. Consciousness had been raised concerning
the need to fulfill a professional responsibility by providing professional input in the sale
of OTC drugs. Alternate means of distinguishing the professional area of a pharmacy
from non-professional areas were discussed. The Professional Relations Committee
suggested, at the 1971 annual meeting, that the OTC area be marked with signs that
created a separate area with the drugstore.195 This method was eventually adopted and
required unique signs that distinctly delineated the professional area. All OTC drugs had
to be kept within this area, which could extend no further than twenty-four feet from the
dispensary, in order that they could be under the direct supervision of a pharmacist.
Despite being unable to remove OTC drugs from public access, pharmacists
continued to act on other recommendations that could further their efforts to claim
194 UBC-SM-CPBC, Box 27-1, BCPhA Council meeting, October, 1968, 10.
195 UBC-SM-CPBC, Box 23-39, Professional Relations Committee Report, BCPhA Annual Meeting, June 1971, 27.
legitimacy as drug information consultants. A committee investigating Non-professional
Assistants (NPA) was appointed by council, in March 1968, and syndicate discussions
were organized at that year's annual meeting. By October 1968, the committee produced
a comprehensive manual, which detailed those duties which must be performed by the
pharmacist and those which could be performed by Non-professional Assistants. The
committee noted that although the use of NPA's would improve the utilization of
pharmacist manpower by freeing them from technical activities, it would also provide
them more time for public and interprofessional consultation. This would have the added
benefit of "enhancing his status with the public and other health professions."196 When
patients entered the professional area of a pharmacy they would encounter pharmacists
who performed professional duties and Non-Professional Assistants for technical duties.
This would mimic the physician's office where the physician was assisted by a non-
professional who made appointments and managed files. The manual that was produced
by this committee was of interest to the CPhA who noted that "the B.C. manual [would]
be used as a basis for study of the subject by the CPhA and constituent bodies."197
In order for pharmacists to be fully recognized as drug information consultants,
the Commission had recommended that their educational requirements be updated, both
at the University and through continuing education. The Faculty had presented a brief to
the Commission that showed their willingness to re-evaluate the curriculum provided by
UBC. The Commission noted that "the Faculty recognizes that the present organization
of the curriculum leaves much to be desired and are presently in the process of … [a]
196 UBC-SM-CPBC, Box 27-1, BCPhA Special Committee on Non-Professional Assistants, October 1968.
197 UBC-SM-CPBC, Box 1-13, CPhA Delegates Report, August 1969, 9.
revision of the course of studies."198 The Pharmacy Act gave the Association
responsibility for education; prior to the founding of the Faculty of Pharmacy at UBC, the
Association was directly involved in the education and examination of pharmacists.199
The Association proposed to the Dean that a Joint Advisory Committee be formed with
representatives from practicing pharmacists, as well as the Faculty. This proposal was
agreed to by both sides and the Joint Advisory Committee on Curriculum was appointed,
in January 1968. The Faculty made changes to the curriculum to incorporate a clinical
program for fourth year students, to be implemented in September 1968. The Faculty
also decreased, by fifty percent, instructional time devoted to pharmacognosy.200 It was
replaced by a one hundred percent increase in pharmacology, as well as the addition of
anatomy and pathology. The curriculum now included basic science in first year, basic
medical science in second year, pharmaceutical science in third year and clinical
pharmacy in fourth year. The Dean believed that new graduates would have
sophisticated knowledge in biology, chemistry, biochemistry, microbiology, physiology,
anatomy, pathology and pharmacology to the "point where he is oriented to the patient in
the diseased state." This, he stated, will allow pharmacists to "play its part effectively in
two areas – drug distribution and in drug information both to the patient and to the
Continuing Education was transferred from the Association to the Faculty. After
the adoption of the Commission's report, in-depth continuing education courses were
offered in hospital pharmacy, medicinal chemistry, general pharmacy and pharmacology;
198 UBC-SM-CPBC, Box 12A-10, PPC Report, 81.
199 UBC-SM-CPBC, Box 2-5, British Columbia Pharmacy Act 1925, 5(1) (a), 3.
200 Pharmacognosy is the study of medicines derived from natural sources.
201 UBC-SM-CPBC, Box 27-1, BCPhA Council Minutes, October 1968, 48-53. The Dean also noted that the increase in emphasis on medical and pharmaceutical science necessitated a reduction in students receiving a broader education, a result that he regretted.
each being two or three day courses. Future plans included education in clinically
oriented subjects such as unit dose systems and family record plans.202 Pharmacists in
British Columbia had made the first steps needed to create a new professional core
competency as drug information experts. Pharmacists had accepted the necessity to
separate professional areas from non-professional areas within the pharmacy. This was
an essential precursor to making themselves available to the public; facilitating effective
and consistent counselling of OTC medications. The use of Non-Professional Assistants
would reduce technical tasks and increase available time for professional services. Co-
operation between the Association and the Faculty had resulted in rapid changes to the
university curriculum and these changes would allow pharmacists to be more clinically
educated and integrated with other health practitioners. Acting as drug consultants for
physicians would require credibility and that would take time. Nonetheless, pharmacists
had taken the first steps that were necessary. Counselling patients on prescription
medications would also take time, as several obstacles still stood in their way.
Pharmacists' professional activities had been restricted by the ethical prohibition
on disclosing or discussing therapeutic and composition information since the 1920s.
British Columbia pharmacists realized that this prohibition could no longer be supported,
if the profession was to advance. In June 1967, the Professional Relations Committee
issued a "strong recommendation" at the Association's annual meeting that their
committee or a special committee be instructed to draw up a new, modern code of
ethics.203 The Professional Relations Committee reported, to the 1968 annual meeting,
that the Society was also working on a Code of Ethics. Subsequently, a Joint
202 See sample in Appendix D.
203 UBC-SM-CPBC, Box 23-38, Report of Professional Relations Committee, Pharmaceutical Association of the Province of British Columbia Annual Meeting and Convention June 1967, 39-40.
Association-Society Committee was appointed to prepare a study and evolve a single
Code of Ethics for the two organizations. The Joint Committee presented a draft Code
of Ethics to council in October 1968 and recommended that it be distributed to all
members for acceptance. They suggested that 75% approval would indicate acceptance
by the membership.204 John Moran reported to council, in March 1969, that 600 replies
had been received of which the vast majority expressed approval (see Appendix G).205
This code had been achieved by a democratic consensus amongst its membership.
Whereas the Code of Ethics adopted in 1923 was detailed, in the code adopted in
1969 specifics were conspicuously absent. The new code made no mention of
therapeutics, symptoms or composition. Instead, those clauses were replaced by the
pledge to "provide the highest level of patient care possible by the use of my skill, and
judgment and by co-operation with other members of the health sciences."206 This
opened the door for pharmacists to access their knowledge to counsel patients, if they
believed it would provide benefits for the patient. Whereas, the 1923 code would only
allow pharmacists to disclose as much information as allowed by the physician, this code
put the judgment in the hands of the pharmacist. In 1923, the power had been in the
hands of the physician and in 1969, the decision rested with the pharmacist, thus both
codes were paternalistic. Patients were still not in control of information concerning their
treatments. Pharmacists pledged co-operation with fellow health practitioners, however,
so before they could start providing information to prescription patients, they would have
to come to an agreement with physicians.
204 UBC-SM-CPBC, Box 27-1, Report the Joint Association-Society Code of Ethics Committee, BCPhA council meeting October 1968, 39-40.
205 UBC-SM-CPBC, Box 27-2, Joint Association-Society Code of Ethics Committee, BCPhA Council Meetings March 1969, 64.
206 See Appendix G.
In 1971, British Columbia pharmacists amended their by-laws to allow
pharmacists the right to provide therapeutic information to patients, but not therapeutic or
medical advice. The committee argued that the use of Family Record Cards and "an
increasing number of questions from the public" meant that pharmacists "must give
therapeutic information."207 At the same time pharmacists were invited to attend the
pharmacy committee of the British Columbia Medical Association (BCMA) to discuss
the labelling of prescriptions with its composition. The BCMA declined to agree to
changes at that time, therefore labelling remained at the discretion of the prescriber, for
the time being. By July 1972, after several discussions and acknowledgment of "pros and
cons in both directions", the pharmacy committee reversed themselves. Consequently,
the BCMA supported legislation that would require pharmacists to label all prescriptions
unless specifically requested not to do so by the physician.208 The path was now clear
for pharmacists to provide drug information to patients about their prescriptions; all legal
and ethical obstacles had been removed. Pharmacists could now claim to be drug
information experts for both OTC and prescription drugs.
The second area of priority for pharmacists was the formation of a new pharmacy
organization, with a mandate to protect the interests of pharmacists. Pharmacists
Bedford Bates and Donald Hoffman were charged with overseeing the inauguration of
the British Columbia Professional Pharmacists Society (BCPPS).209 As recommended by
the Commission financing would be voluntary, not mandatory as suggested by the Study
Committee. The Society was given jurisdiction over recommendations that concerned
207 UBC-SM-CPBC, Box 23-39, Professional Relations Committee Report, BCPhA Annual Meeting, June 1971, 28. See Appendix D for an example of a Family Record Card.
208 UBC-SM-CPBC, Box 13-4, BCMA New-Views-Reports July 1972.
209 Bedford Bates was co-owner of McGill & Orme Prescriptions along with Ron Stocks. Ron Stocks had
purchased his shares from William McGill in 1955. Stocks was one of the original members of the SVIPA who had pushed the BCPhA to form the Pharmacy Planning Commission.
mainly economic matters such as separate accounting for dispensaries, improved
administration instruction, salary and working conditions and negotiations with
government and suppliers. The Commission had also recommended that the Association
restrict its activities to the requirements of the Pharmacy Act, when the Society was
functional.210 At the time of the inaugural meeting of the Society, on June 12, 1968, over
fifty percent of British Columbia pharmacists had joined the new organization.211 An
Association-Society liaison committee was formed to ensure effective communication
between the two groups. Special committees were formed immediately to develop a
Code of Ethics and to negotiate with the government on welfare prescriptions.212
Payments for welfare prescriptions were hotly contested in 1968. The Association's
failure to find a satisfactory resolution was an important factor in the Study Committee's
call for a second pharmacy organization.
Pharmacists had been in a running battle with the provincial government over the
reimbursement of Welfare prescriptions. The Association had been unable to update the
pricing agreement with the province that had been in effect since 1954. One of the issues
was that the province would not accept a pricing policy that included fee for service.
Even more worrying was the two tiered pricing method employed by manufacturers;
prices to community pharmacies was substantially higher than those to government
funded organizations such as hospitals. The provincial government had been directing
physicians to send expensive prescriptions to the Provincial Dispensaries. Pharmacists
were concerned that this trend would increase and jeopardize their ability to make their
living filling prescriptions. In June 1967, the council tabled a proposal at the annual
210 Recommendations Five, Eight, Nine, Ten, Twenty, Twenty-five, Thirty-Two and Thirty-Four, Appendix F.
211 UBC-SM-CPBC, Box 27-1, Registrar Report, D. Denholm, BCPhA Annual Meeting, June 1968, 38.
212 UBC-SM-CPBC, Box 27-1, Association-Society Liaison, BCPhA Annual Meeting, June 1968, 74-75.
meeting to call the provincial government's bluff and threaten to discontinue prescription
service to Welfare patients. When this was put to a vote, it was defeated seventeen to
fifteen. Pharmacists feared that this might backfire and encourage the government to
increase the use of Provincial Dispensaries. Additionally, some felt that refusing service
to a specific group would not be good for pharmacists' public reputation. As one
pharmacist stated, "we have had enough trouble in the past with our relationship with the
public." As an alternative, Stan Fyfe from the Study Committee moved that the matter be
referred to the inaugural committee of the Society and in the mean time council should
continue negotiations. This motion passed by a majority of nineteen to zero.213 Turning
this issue over to the Society, even before it was officially formed, showed the confidence
the members had in the new organization and also the type of issues they wanted it to
The Welfare prescription issue also highlights an important reason why the
Pharmacy Planning Commission had successfully instigated so many substantive
changes, while other attempts had failed. Credit should be given to the individuals that
participated in the Commission and its implementation. There were clearly many strong
willed characters who promoted changes throughout these years. But strong individuals
cannot account for the extent of the changes seen at this time. The pharmacists involved
were not new to the profession; they had been involved in British Columbia pharmacy for
many years. The Welfare prescription issue defined the fears of pharmacists that their
profession might disappear or be reduced to a technical function. Registrar Denholm had
213 UBC-SM-CPBC, Box 23-38, Annual Meeting Minutes, BCPhA Annual Meeting, June 1967, 194-5.
214 Ironically, the issue of Welfare prescriptions was the first major challenge that the Society dealt with when it formed. Their solution was to level a $1.00 surcharge on all welfare prescriptions. They were sued by the federal government for price fixing since they had advocated that all pharmacies participate. They fought the lawsuit unsuccessfully and were levied a $10,000 fine, a substantial amount in the late 1960s.
put the blame on the profession by suggesting that pharmacists had not kept "pace with
society in its rapidly increasing degree of sophistication."215 Dean MacPhee put the onus
on pharmacists to take charge of their profession. Fear is a great motivator and
pharmacists were worried enough about their future to overcome any disagreement over
tactics to find effective ways to recreate their profession. While the accomplishment was
driven by the force of a few key individuals, the degree of success was only possible with
the collective acceptance of change by the majority of the profession. Achieving public
acceptance as drug information experts could only be possible if practicing pharmacists
actively made themselves available to the public for consultation on OTC drugs. The
result was an increase in their scope of practice through the addition of a core
competency as drug information experts. The long term effect was increased
professional respect, with the public and other health professionals.
215 UBC-SM-CPBC, Box 23-38, Registrar Report, D. Denholm, BCPhA Annual Meeting, June 1967, 84.
Conclusion
The profession of pharmacy has reconstructed their professional role within the
Canadian health care system since achieving statutory professional status in the
nineteenth century. While health care throughout North America has evolved over that
time period, pharmacists have been forced to realign their practices in order to maintain
their position has experts on medications. Pharmacists have been able to adapt to
changing situations by redefining and expanding their core competencies.
In the late nineteenth century, community pharmacists displayed four
competencies; compounding, manufacturing, diagnosing and prescribing. None of these
competencies could be considered distinct as each was performed by at least one other
group. Pharmacists were recognized in the nineteenth century as legitimate practitioners
of all four practices, as shown by the public who accessed their services. Not all
competencies were recognized by physicians, who argued that pharmacists did not have
the necessary specialized training to diagnose or prescribe (counter prescribing).
Pharmacy elites tried to control counter prescribing unsuccessfully, using pharmacy
ethics. The public, however, was dependent upon counter prescribing pharmacists for
economic and accessibility reasons. Pharmacists were also aided by the public's
acceptance of self-medication as a valid treatment option. The public afforded the
legitimacy and exhibited the dependency that gave pharmacists the authority to resist
opposition. Resistance was important to pharmacists because counter prescribing
enhanced their financial stability. Although manufacturing had diminished since the
middle of the century, pharmacists were extensively trained to isolate drugs from natural
or chemical sources and that skill remained an important role in their profession.
Compounding physicians' prescriptions made up a financially small but professionally
important competency.
These four competencies were crucial to pharmacists' survival in the late
nineteenth century and thus formed their core competencies. In combination, they created
a capability that extended from manufacturing raw materials to the preparation and
distribution of drugs. Pharmacists were able to interact with society through direct
relationships with a self-medicating public as well as indirectly through physicians'
prescriptions. Health practitioners, in the nineteenth century, operated independently in a
rough and tumble era with few regulations on practitioners or their practices. Similarly,
each member of the public would choose their health practitioner based on the reputation
of the individual. They may choose a physician to treat their medical conditions but
might alternatively choose a pharmacist, homeopath or naturopath. Their choice would
often be based on the individual reputation of the health practitioner, rather than their
medical specialty.
In the early twentieth century, societal attitudes towards medicine shifted and the
pharmaceutical manufacturing industry strengthened. Manufacturing at the community
pharmacy level faded into insignificance with its resultant loss as a core competency.
The backlash against patent medicines and self-medication shifted medical authority
toward physicians. Governments were now increasingly regulating medications; opium
became the first of many drugs that could only be obtained after consulting a physician
and receiving a prescription. As physician authority increased, pharmacist authority
waned. Pharmacists had capitalized on the public's self-medication habits but had lost its
legitimacy to diagnose and prescribe when society turned away from self-medication and
towards the authority of physicians. Physicians were now increasingly seen as the only
legitimate profession that could diagnose and prescribe and the public's dependence on
them grew. Pharmacists' loss of three core competencies along with the spectre that
modern scientific medicine might eliminate the need for drugs, left pharmacists worried
that their profession might not survive. Abraham Flexner's verdict that they were a
branch of medicine, not a profession left pharmacists struggling to revitalize their
professional with an education that was thirty years out of date and an ethical code that
had been ignored for decades. Pharmacists' dynamic capability, its ability to reconfigure
to rapidly changing environments, was tested.
Pharmacists used a revised Code of Ethics, adopted from the APhA in the 1920s,
to configure pharmacist's professional focus. This code included detailed instructions
that covered many activities that pharmacists carried out daily. Pharmacists should
refrain from discussing treatments or symptoms with patients and only disclose the
composition of a prescription upon the request of the prescribing physician. This ruled
out counter prescribing and, along with the loss of manufacturing, left pharmacists with
only one remaining core competency, compounding. What remained of a pharmacist's
authority was now deeply imbedded in the authority of physicians. The revamping of
medical education, early in the century, had resulted in fewer, better educated physicians
and this improved their economic opportunities. Although some prescriptions were still
being compounded in the physician's office, especially in rural areas, most were now
filled by pharmacists. Although reduced to one core competency, that competency could
now be considered distinct to the pharmacy profession. As a profession they accepted
ethical restrictions on divulging drug information; acting together to protect their core
competency, compounding. Pharmacists' dynamic capability had successfully adapted
their competencies to meet changing circumstances.
Like manufacturing previously, compounding disappeared as a core competency
after World War II. Pharmacists were now seen by the public as "pourers and counters"
and, as noted by Elenbaas and Worthen, overeducated and underutilized. They were now
in danger of losing the right to claim any core competencies that could qualify them as
professionals. Pharmacists still retained a drug distribution role but that role now seemed
more technical than professional and they were saddled with an ethical code that
prohibited them from any involvement beyond drug distribution. By the 1960s, some
pharmacists were ignoring their ethical code by providing prescription counselling but
these were isolated cases. While pharmacists all over North America faced the same
challenges, British Columbia pharmacists undertook to remake their profession, in the
mid 1960s. The Pharmacy Planning Commission, sparked by pressure from a local
pharmacy organization, started the process that allowed pharmacists in British Columbia
to incorporate a new core competency as drug information experts.
When the Pharmacy Planning Commission (the Commission) was formed in
1966, pharmacist's authority was at low ebb. Their previous experience with
reformulating their profession had required them to adapt to the loss of core
competencies. They now sought to add a core competency. This would not be as simple
as unilaterally declaring themselves drug information experts; they did not have sufficient
authority. Pharmacists saw that there were three avenues they could explore to
disseminated drug information. Firstly, they could act as drug consultants to physicians.
The Commission found, however, that physicians did not believe that pharmacists could
exercise legitimacy as drug consultants, primarily because of deficiencies in their
education. Secondly, pharmacists could counsel their patients about their prescription
medications. Unfortunately, pharmacy ethics still prohibited pharmacists from discussing
prescriptions with their patients and only allowed them to divulge the name of the drug
with the physician's consent.216 Pharmacists had a tacit agreement with physicians
concerning prescription information and they did not want to unilaterally alter that
agreement. Acting as drug experts in both areas was beyond pharmacists' authority in
Offering OTC drug consultations to the public was the only avenue that
pharmacists could access immediately. The Commission believed that the public was
looking for help when making OTC medication choices and would welcome a
pharmacist's expert opinion, if pharmacists were accessible. This was an opportunity for
pharmacists to regain a role in assisting the public to self-medicate that they had lost
decades earlier. Society was dependent upon pharmacists through legislation as many
OTC medications could only be purchased in a pharmacy. Legislative dependence was in
jeopardy, however, because pharmacies were routinely selling these medications with no
involvement by pharmacists. By creating a professional area within the pharmacy,
pharmacists could add professional dependence to legislative dependence. The
alternative might be a severe blow to their professional status; if they failed to retain their
monopoly. To protect their monopoly and its legally assigned authority, the Commission
specifically recommended that a full time inspector be hired to ensure that non-
216 This practice was not changed until 1972.
pharmacies did not sell restricted OTC drugs. Maintaining their monopoly would ensure
that OTC drug consultation was a distinct competency. Shifting their education to
include clinical programs with direct involvement with patients along with continuing
education efforts would add to the legitimacy of their specialized training. Increasing
both legitimacy and dependency would allow pharmacists the authority to claim, at least
in one area, a core competency as drug information experts.
The limitations of authority can be seen in pharmacists' failure to create the
professional area in pharmacies envisioned by the Commission. Pharmacists did not
have the authority to arbitrarily remove a freedom enjoyed by the public, in this case
access to OTC drugs, unless they could prove that it was in the public's interest. This is
one of the key features of professionalism, as noted by Parsons and others; professionals
put the public's interests ahead of their own. Even though pharmacists believed that
there was potential harm to the public from the misuse of OTC drugs, they could not find
specific cases in the literature that showed the public being harmed by them. With
evidence lacking, a move to restrict the public's access would be seen as in pharmacists'
interest, not the public. Without that authority, pharmacists were forced to back down
from their plan. Despite being unable to restrict public access pharmacists did raise
awareness, amongst the profession, about the importance of engaging with the public
during the sale of OTC medications. Those medications were subsequently concentrated
close to the dispensary to facilitate consultation. That shift allowed pharmacists to be
seen, by the public, as drug information experts.
The Commission was a groundbreaking event for British Columbia pharmacists
and was important to pharmacy for several reasons. Firstly, they tackled issues that were
critical to pharmacists; core competency, education and organizational structure.
Secondly, pharmacists in British Columbia were able to effectively act upon the
recommendations to make substantive changes to their profession. This stands in contrast
to studies, in Canada and the United States, that had failed to trigger the changes that
pharmacists required. Thirdly, the Commission allowed British Columbia to set
professional standards that other jurisdictions sought to emulate. Executive director of
the CPhA John Turnbull foreshadowed the Commission's importance, at the
Association's annual meeting in 1966, when he told delegates that they should "bear in
mind that the rest of Canada was watching us very carefully."217
British Columbia's Commission pre-dated commissions that followed similar
patterns in the United States and Canada. John S. Millis was chancellor emeritus of Case
Western Reserve University with a background in physics and mathematics; he had no
pharmacy experience. He led the Millis Commission on Pharmacy in the United States
whose mandate was to "determine the scope of pharmacy services in health care and
project the educational processes necessary to insure that these services are obtained."218
Their report, released in December 1975, found that pharmacy education should include
contact with other healthcare professionals, at the bedside of the patient, not isolated
behind the prescription counter. This would integrate pharmacists into the healthcare
team, and allow them to use their knowledge to ensure appropriate medication use by
patients; clinical pharmacy would be the primary focus.219 Elenbaas and Worthen argue
that clinical pharmacy went through a period of implementation and evaluation in the
1980s and 1990s, culminating in the emergence of pharmaceutical care, "a covenantal
217 UBC-SM-CPBC, Box 23-38, Syndicate Discussion #2, BCPhA Annual Meeting, June 1966, 186-7.
218 Sonnedecker, History of Pharmacy, 254.
219 Elenbaas and Worthen, "Transformation of a Profession," 156-7.
relationship between a patient and a pharmacist in which the pharmacist performs drug
use control functions (with appropriate knowledge and skill) … to the patient's
In Canada, the CPhA embarked on a study similar to the Millis Commission with
the formation of the Commission on Pharmaceutical Services, in 1967. Their mandate
was broadly similar to the Millis Commission and British Columbia's Commission.
They were asked to explore the occupational, organizational and economic aspects of
pharmacy as well as recruitment and educational requirements. The chairman was Dr
John B. MacDonald, Professor in the Faculty of Dentistry and Past President of U.B.C.,
along with prominent pharmacists from across Canada. The CPhA was aware of British
Columbia's Commission, and its significance, having remarked that it was a "first" for
B.C. pharmacists in their journal the previous year.221 As noted earlier, CPhA Executive
director John Turnbull had told pharmacists when the Commission was formed that all
Canada was watching them. Their report was released in June 1971, with ninety-seven
recommendations that were as broad as their terms of reference. A major section of their
report dealt with the occupational role of the pharmacist. The use of non-professional
assistants was recommended; the CPhA would provide individual provinces with training
and occupational guidelines. The importance of patient contact and the monitoring of
medications through the use of patient medication records were emphasized. Many of
their suggestions were later imbedded in the concept of pharmaceutical care.222
Examination of British Columbia's current Code of Ethics shows the shift in focus
220 Elenbaas and Worthen, "Transformation of a Profession," 165. 221 Canadian Pharmaceutical Journal Vol 99 No 8 (August 1966), 285.
222 Bachynsky, "Pharmacy in a New Age," 29.
toward patients.223 It is significant that British Columbia's Commission was able to
achieve similar results in advance of both national efforts.
It is possible to identify a number of innovations emanating from the Commission
that influenced pharmacy in the rest of Canada. The SVIPA original goal of a second
pharmacy organization (the Society) came at a time when pharmacist advocate
organizations did not exist in Canada. Previously, each province had one licensing body
to enforce their Pharmacy Act and to handle issues that affected the interests of
pharmacists, such as economics. This created an obvious conflict of interest and the
development in British Columbia of one organization to look after the interests of the
public and another to look after the interests of pharmacists was critical. Ontario was also
developing an organization, the Ontario Pharmacists Association, at the same time while
other provinces followed suit over the succeeding decades. In August 1969, the Society's
employment code was directed by the CPhA to pharmacy organizations across Canada
for their study. Following the Commission's recommendation that Non-Professional
Assistants (NPA) be used to allow pharmacists to restrict their efforts to professional
duties, British Columbia developed a comprehensive manual detailing the duties that a
pharmacist must perform and those that a NPA could perform. In August 1969, this
manual was recommended by the CPhA for use as a basis for study by the provinces and
the CPhA. At the same time, the Code of Ethics developed in the aftermath of the
Commission, was recommended by the CPhA for adoption by the provinces.
Pharmacists were now able to break away from the constraining ethical code that
prevented them from seeking legitimacy as drug information experts. Although still
223 See Appendix G for British Columbia's 2009 Code of Ethics.
paternalistic, it set the stage for a truly fiduciary code to follow in the 1990s; one that put
patients at the front rather than health professionals. On the development of practical
university based clinical training and continuing education for practicing pharmacists, it
was noted that "B.C. stands well in the forefront of developments in both fields." 224
Progress in the adoption of Fee for Service pricing, the Fuller Method, was aided
by the endorsement of the committee. The number of pharmacies using the method
increased from 69.5% in September 1967 to 85% in January 1968.225 This answered a
key question that had hampered pharmacists' claim as full professionals: charging for a
service rather than selling a product.
Pharmacists in British Columbia have recognized the importance to the work that
was done by the individuals involved in the Pharmacy Planning Commission and its
aftermath. Commission members John Dyck and Trevor Watson were made honourary
members for life of the British Columbia Professional Pharmacists Society as were
Donald Hoffman, entrusted by the Commission to implement the Society and Peter Bell,
the Society's first executive director. They make up four of the sixteen pharmacists with
this honour. The Society has honoured the final member of the Commission by creating
the Murray Dykeman Mentorship Award. They have also created the Ben Gant
Innovative Practice Award to honour the Association councillor who was active in the
creation and implementation of the Commission.
The Pharmacy Planning Commission produced practical recommendations that
British Columbia pharmacists implemented resulting in improved profession status. The
Commission used the same format that would be followed later at the national level in
224 UBC-SM-CPBC, Box 1-31, CPhA Delegate Report, August 1969, 9 & 13.
225 UBC-SM-CPBC, Box 27-1, Economic Committee Report, Pharmaceutical Association of the Province of British Columbia Annual Meeting and Convention June 1968, 13.
both Canada and the United States. All three commissions used a non-pharmacist
academic as their chairman with practicing pharmacists as members and all consulted
pharmacists, government, academics and the public in their deliberations. British
Columbia accomplished their commission in 1967; the CPhA would not release their
report until 1971 and the Millis Commission in 1975. This put British Columbia at the
forefront in taking effective action that would allow their profession to advance over the
following decades. The actions they proposed started pharmacists on the path to a new
core competency, as drug information experts, in the only area they could control at the
time, OTC drugs. As the recommended educational curriculum improved to include
clinical programs, pharmacists were able to integrate themselves fully into the health care
team. This allowed them the legitimacy to increase their influence to counselling on
patient prescriptions. Pharmacists who had once been ethically prohibited from
counselling on prescriptions eventually became legally required to counsel on all
prescriptions. By the 1990s, pharmaceutical care had become mainstream professional
practice. As physicians became more comfortable with the specialized knowledge offered
by pharmacists, they were able to accept them as viable drug consultants for their
practices. Pharmacists now had the clinical education, integrated with patients and other
health professionals, which could command physicians' respect. For most of the
twentieth century, pharmacists were unable to divulge drug information to the public.
The Pharmacy Planning Commission helped British Columbia pharmacists reconstruct
their profession to allow the addition of drug information expert as one of their core
competencies and enhance its professional image. This thesis has followed the path that
transformed pharmacy from a profession with legal status but lacking other professional
characteristics to recognition as a full profession.
Archival Sources
University of British Columbia Special Collections, "College of Pharmacists of British
Columbia: An Inventory of their Records." Boxes 1-27. These records include
minutes from council and annual general meetings, correspondence, commission
reports and submissions, some BC Professional Pharmacist Society records, exam
results, legislation plus assorted documents from 1891 to 1983.
McGill & Orme Prescription Records, currently held by Steve Dove at 861 Richmond
Avenue, Victoria, B.C. These contain business records, newspaper clippings,
photographs, prescription files from 1931, 1941 and 1947, and historical notes
prepared by William McGill.
Secondary Sources
Akers, Ronald. "The Professional Association and the Legal Regulation of Practice." Law
and Society Review Vol. 2 No. 3 (May, 1968): 463-482.
Anderson, Lee. Iowa Pharmacy 1880-1905: An Experiment in Professionalism. Iowa
City: University of Iowa Press, 1989.
Bachynsky, John. "Pharmacy in a New Age – A Milestone Study." In Canadian
Pharmacists Association 1907-2007 -100 Years of Leadership in Pharmacy
Ottawa: Canadian Pharmacists Association, 2007, 25-30.
Buerki, Robert. "The Historical Development of an Ethic for American Pharmacy."
Pharmacy in History Vol. 39 No. 2 (1997): 54-72.
Buerki, Robert. "The Public Image of the American Pharmacist in the Popular Press."
Pharmacy in History Vol. 38 (1996): 62-78.
Buerki, Robert and Vottero, Louis D. Foundations of Ethical Pharmacy Practice.
American Institute of the History of Pharmacy, Madison, Wisconsin, 2008.
Canadian Pharmaceutical Journal, July 1881 - August 1966. Clark, R.J. "Professional Aspirations and the Limits of Occupational Autonomy: The
Case of Pharmacy in Nineteenth-Century Ontario." Canadian Bulletin of Medical
History Vol. 8,(1991): 42-63.
College of Pharmacists of British Columbia,
College of Pharmacists of British Columbia,
Cowan, David L. "Pharmacists and Physicians: An Uneasy Relationship." Pharmacy in History Vol. 34 (1992): 3-16. Denzin, Norman and Mettlin, Curtis. "Incomplete Professionalization: The case of
Pharmacy." Social Forces Vol. 46 No. 3 (Mar, 1968): 375-381.
Department of Justice Elenbaas, Robert M. and Dennis B. Worthen. "The Transformation of a Profession: An
Overview of the 20th Century." Pharmacy in History Vol. 51, No. 4 (2009): 151-181.
Flexner, Abraham. Medical Education in the United States and Canada. North Stratford:
Ayer Company Publishers Inc, 2003 reprint edition.
Freidson, Eliot. Professional Dominance: The Social Structure of Medical Care. New
York: Atherton Press Inc, 1970. Freidson, Eliot. "Theory of Professionalism: Method and Substance." International
Review of Social and Behavioural Sciences Vol. 9 No. 1 (1999): 117-129. Gidney, R., and W. Millar. Professional Gentlemen: The Professions in Nineteenth-Century
Ontario. Toronto: University of Toronto Press, 1994. Herzberg, David. "Will Wonder Drugs Never Cease!." Pharmacy in History Vol. 51 No
2 (2009): 47-56.
Huisman, Frank. "Medical Histories." In Locating Medical History: The Stories and
Their Meanings ed. by Frank Huisman and John Harley Warner. Baltimore: The
Johns Hopkins University Press, 2004, 1-30.
Kluge, Eike-Henner W. Biomedical Ethics: In a Canadian Context. Scarborough:
Prentice-Hall Inc, 1992.
Malleck, Daniel. "Its Baneful Influences are too Well Known: Debates over Drug Use in Canada, 1967-1908." Canadian Bulletin of Medical History Vol 14 (1997): 236- 288. Malleck, Daniel J. "Professionalism and the Boundaries of Control: Pharmacists,
Physicians and Dangerous Substances in Canada, 1840-1908." Medical History
Vol. 48, (2004): 175-198.
Malleck, Dan. "Pure Drugs and Professional Druggists: Food and Drug Laws in Canada,
1870s- 1980." Pharmacy in History Vol. 48 No. 3 (2006): 103-110.
Merriam Webster Dictionary, <http://www.merriamwebster.com/dictionary/therapeutics> Parsons, Talcott. The Social System. London: Tavistock Publications Limited, 1952.
Raison, Arnold (ed). A Brief History of Pharmacy in Canada. Toronto: Canadian
Pharmaceutical Association, (1969).
Savage, Deborah Anne. "The Professions in Theory and History: The Case of
Pharmacy." Business and Economic History Vol. 23, No. 2 (Winter, 1994): 129-
Schondelmeyer, Stephen. "Recent Economic Trends in American Pharmacy." Pharmacy
in History Vol. 51 No 3 (2009): 103-133.
Sonnedecker, Glenn. Kremers and Urdang's History of Pharmacy. American Institute of
the History of Pharmacy, Madison, Wisconsin, 1976. (1986 Paperback Edition)
Shortt, S.E.D. "Physicians, Science, and Status: Issues in the Professionalization of
Anglo-American Medicine in the Nineteenth Century." Medical History Vol. 27
(1983): 51-68. Starr, Paul. The Social Transformation of American Medicine. New York: Basic Books
The Daily Colonist, 15 April 1880 – 11 March 1891. The Financial Post, April 6, 1963. Victoria Daily Times, 7 November 1930.
Warner, John Harley. "Grand Narrative and its Discontents: Medical History and the Social Transformation of American Medicine." Journal of Health Politics, Policy and Law Vol 29 No 4-5 (August-October: 2004): 757-780.

Appendix A226
226 McGill & Orme Archives, Letters.


Appendix B227
These labels (with the exception 1933 and 1948) were saved because they had humorous errors in their directions not because they were missing composition details. Note that in most cases there was not enough room on the label to add drug names. Patient's last
names have been removed for privacy reasons.
227 McGill & Orme Archives, Labels.
Appendix C228
Prescription Survey
In February 2010, I examined two files of prescription filled at McGill & Orme Prescriptions in Victoria. One set included 978 prescriptions filled between March 23 and July 28, 1931 and the second included 975 prescriptions filled between February 26 and March 6, 1947. These prescription files are from my private collection. My survey sorted and counted the prescriptions in the following categories;
1931 1947
1. Total prescriptions surveyed
2. Total Compounded Prescriptions
3. Prescriptions filled with commercially manufactured products. -
4. Prescriptions containing morphine -
5. Prescriptions containing opium -
6. Prescriptions containing heroin -
7. Prescriptions containing cocaine -
8. Prescriptions with ingredients that required a physician's order
9. Prescriptions filled per day
Discussion
Category Two
Category two contains prescriptions compounded with one to nine ingredients.
Prescriptions with one ingredient included items such as Tincture of Opium, which may
have been purchased from a manufacturer or compounded locally. Since McGill & Orme
were still locally compounding products that were available commercially in the 1970s, I
believe that most of these products would have been compounded locally.
Category Three
Category three contains prescriptions for commercially manufactured products. In 1931
they were mainly either manufactured tablets, capsules or hypodermic tablets (Luminal
tablets) or patent medicines (Lavoris). McGill & Orme compounded tablets and capsules
in 1931 but they were counted in this category if the manufacturer was recorded on the
prescription or if it was a standard manufactured dose. Compounded tablets and capsules
with two or more ingredients were included in category one. In 1947, manufactured
products came in more dosage forms including tablets, capsules, topical creams,
ophthalmic ointments, vaginal creams, injectables and nasal mists.
Category Eight
Category eight includes prescriptions that could only be dispensed on a physician's order.
In 1931, that only included prescriptions for morphine, heroin, opium and cocaine. In
1947, that list included morphine, heroin, opium, cocaine plus aminopyrine,
amphetamine, aureomycin, barbituric acid, cinchophen, neochinchophen,
228 McGill & Orme Archives, 1931 and 1947 prescription files.
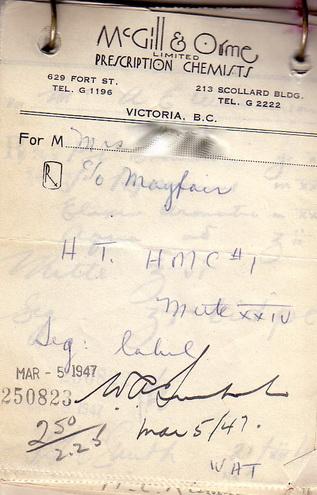

desoxyephedrine, methedrine, ortho-dinitrophenol, penicillin, pervertin, phenytoin,
streptomycin, sulphonamides, tetraethylthiuram, thiouracil, thyroid, thyroxin and
urethane.
Miscellaneous Information
1. The physician instruction "label" was found on only one prescription in 1931
(Rx1014) and one prescription in 1947 (250823). This notation instructed the pharmacist to include the composition of the physician's order on the patient's prescription label.
2. In 1931, physicians sometimes included designations in the directions that would
identify the prescription without listed the ingredients. Examples include: Rx 1377 – THE TABS One tablet three times daily before meals
Rx 1126 – THE DROPS As directed
3. Physicians would occasionally add "clinical therms" to the prescription such as
Rx1843 - "Keep in mouth for full two minutes." These instruct the pharmacists to pass this information on to patients. Unless requested, pharmacists were not supposed to give any additional instructions to the patient.
4. The following drugs in the 1931 prescription file would not be prescribed in 2010.
Calomel (Mercurous Chloride), Strychnine, Arsenic and Cannabis. Synthetic cannabis (nabilone) is used in 2010 to treat nausea resulting from cancer chemotherapy.
5. Four homeopathy prescriptions were filled in 1947. 6. Antibiotic prescriptions accounted for 130 out of 975 prescriptions in 1947.
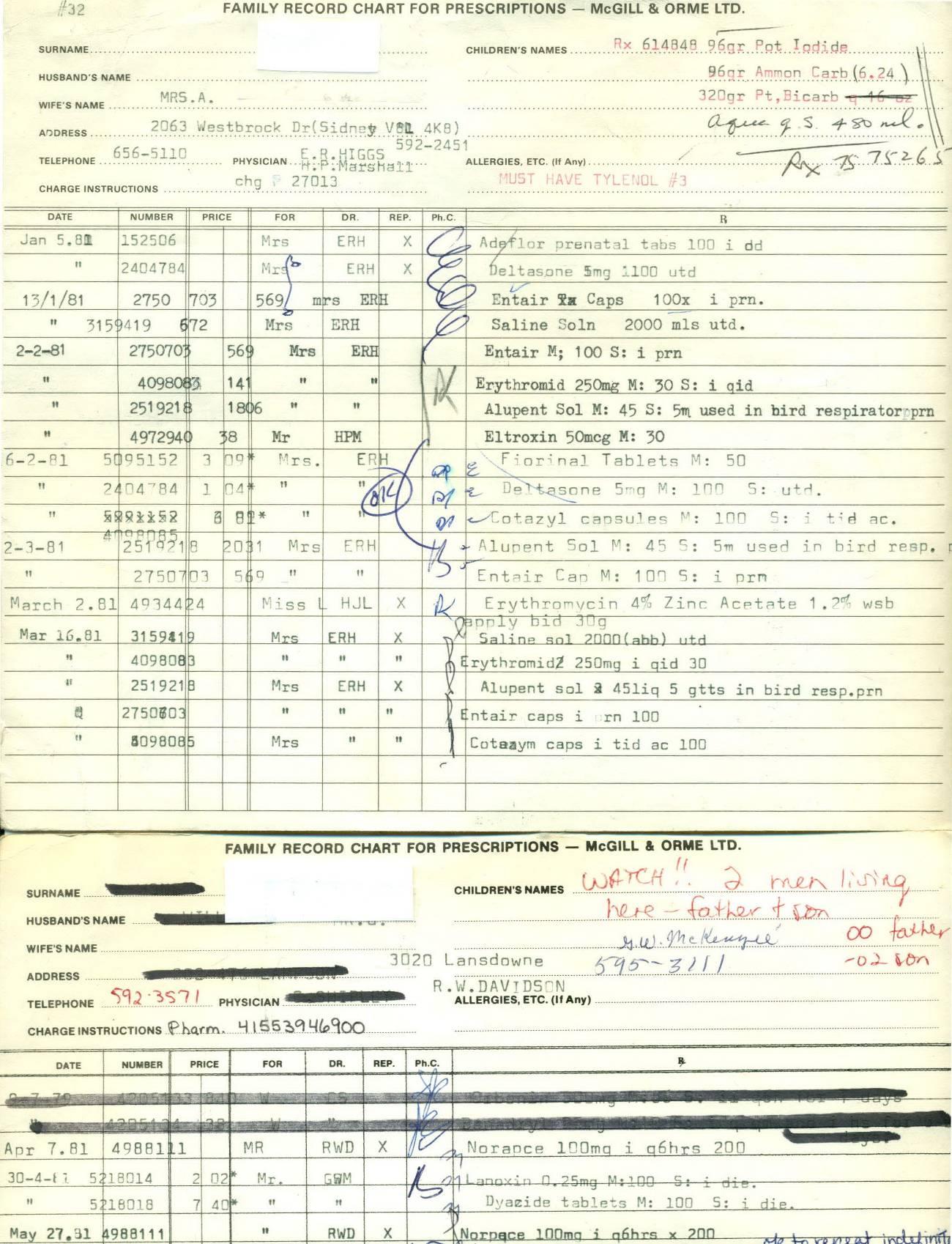
Appendix D229
229 McGill & Orme Archives, Family Record Chart.
Appendix E
Pharmacy Planning Commission – Resolution of the 1966 BCPhA Annual Meeting
That: the 1966 Annual Meeting of the Pharmaceutical Association of the Province of
British Columbia recommends to council that immediate steps be taken to appoint a
Planning Commission by the time of the October 1966 council Meeting. This
Commission is to receive briefs from interested individual pharmacists, groups of
pharmacists, associations, etc. Such Commission is to consist of all facets of our
professin with consultants and advisors. The chairman to be appointed at the discretion of
council. Also, that this Planning Commission and the terms of reference be accetable to
all practicing pharmacists through district meetings. Further, that this Commission be
instructed to report their findings to a meeting of the council and all interested
pharmacists at the tme of the March 1967 meeting of council and, further, to include in its
deliberations the Report of the Study Group on Pharmacy in British Columbia under the
auspices of the South Vancouver Island Pharmacists' Association and the Lower
Mainland Pharmacists' Association as submitted to council on Sunday, June 19th,
Pharmacy Planning Commission – Terms of Reference
General The Commission shall inquire into and report upon all aspects of the practice of
pharmacy, the provision of pharmaceutical services to the public and the organizational
structure of the profession within the province of British Columbia, making such
recommendations as it sees fit respecting the service provided to the public, the status of
the pharmacist and the profession's organizational structure.
Specific Without limiting the generality of the foregoing, the Commission shall inquire into
and report upon:
230 UBC-SM-CPBC, Box 12A-10, PPC Report, i.
a) The organizational structure of the Association and its functions, both statutory
and representative, including a consideration of the need and/or advisability of
extending them or establishing other organizations to separate the functions.
b) The relationship between the "profession" of pharmacy and the "business" of
pharmacy (i.e., the professional-commercial balance), including an assessment of
the utilization of the pharmacist's professional services and education.
c) The economics of providing professional pharmacy services (without reference to
the cost of the drug itself).
d) The relationships between employer and employee pharmacists, including a
consideration of remuneration to, and other conditions of employment of,
employed pharmacists and registered students.
e) Manpower sources and requirements, including the recruitment, enrollment and
training of pharmacy students and the registration of pharmacists from outside the
f) Communications and relationships between the Council of the Association and
pharmacists and pharmacy students.
g) Communications and relationships between pharmacists and themselves.
h) The relationships between pharmacists and physicians and other health
professionals at the practising, organizational and educational levels.
i) The relationships between pharmacists, as represented by the Association, and
departments of government.
j) The relationships, current and potential, between pharmacists, as represented by
the Association, and insuring agencies providing drugs and pharmaceutical
services as benefits in health care plans.
k) The relationships between pharmacists individually and collectively (the
Association) and the pharmaceutical manufacturing and wholesaling industries.231
231 UBC-SM-CPBC, Box 12A-10, PPC Report, ii.
Appendix F
Pharmacy Planning Commission Recommendations
Chapter 4 – Professional and Commercial Services
1. The Commission recommends that all medicinal products that are restricted to
sale in a pharmacy be removed from public access and placed with an area under
the personal supervision of a licensed pharmacist.
2. If a physical barrier were installed sufficient to prevent all access to a dispensary
and restricted OTC area, we recommend that pharmacists be allowed to lock the
pharmacy department and leave the balance of the operation open, without the
supervision of a pharmacist.
3. We recommend that our Association, through CPhA, urge the Food and Drug
Directorate to create effective legislation regarding advertising of drug products.
4. On the question of proliferation in pharmacies, we have concluded that there can
be no form of control of the professional-commercial balance by regulatory
5. We recommend that all pharmacies institute a separate accounting procedure for
the professional department.
Chapter 5 – Pharmacist Utilization and Remuneration
6. We do not find that there is a shortage of pharmacists in the province at the
present time, but we recognize that this situation may not continue. We
recommend that recruitment activitiy be intensified, to attract the most capable
7. It is obvious that there is under-utilization of the competency of the pharmacist
and that this is having a detrimental effect on such things as remuneration, and job
8. Employees must develop a full awareness of the administrative problems of an
operation, so that a "professional partnership" may develop. The benefits and
rewards of such a partnership should be enjoyed by both parties.
9. We have concluded that a starting salary for pharmacists of approximetly $7,200
would be fair. We recommend a salary scale which, over the first six years of
practice would result in a basic salary of $10,000 per annum for employed
10. We recommend the development of a permanent negiotiation procedure to be
concerned with remuneration and working conditions for all pharmacists.
Chapter 6 – Education
11. We recommend that the Faculty become more aware of the needs of community
and hospital practice and re-orient themselves to the importance of these aspects
of the practice of Pharmacy.
12. We recommend curriculum revisions in the following area:
1. A reduction in the emphasis placed on the physical sciences and an
increased emphasis toward the biological sciences, to better prepare the
student for the changing patterns of patient care.
2. Drastic changes in the emphasis placed on pharmacognosy.
3. Development of a program of clinical exposure at the undergraduate level.
13. We recommend development of a program of practical experience for
undergraduates which would involve the profession in the training of students.
14. We recommend that the Faculty establish a Department of Pharmacy
Administration to better prepare the undergraduate to function in our present retail
distribution system.
15. We recommend that the Faculty continue to assist in all programs of recruitment.
16. We recommend immediate attention to be given to the inadequacies of our present
Continuing Education program.
17. We recommend that Pharmacy ensure the provision of pharmacy service in all
hospitals and related institutions.
Chapter 7 - Pharmacy Organization
18. We recommend that the members of Council involve themselves more in
interpreting Council actions to the membership through more attention to their
district organizations, and that the President assume a prominent role in directing
the affairs of the Association.
19. We recommend improved inspection services to ensure public safety and
standards of practice.
20. We recommend that the BCPhA restrict its activities to those which are justified
within the confines of the Pharmacy Act.
21. We recommend that the Council of BCPhA give consideration to providing
adequate reimbursement of the expenses of the President, and increased
remuneration for Councillors.
22. We recommend that there be four Council meetings annually and that they be
held in January, March, June and September.
23. We recommend that District 7 be divided as follows:
1. Burnaby-Richmond-Steveston to elect one councillor
2. North and West Vancouver, Sechelt and Squamish to elect one councillor.
3. The City of Vancouver to elect two councillors.
24. We recommend that the By-laws of the Association be amended to declare the
Dean of the Faculty of Pharmacy as a member of the Council.
25. We recommend the formation of a Society which would concern itself with the
promotion of Pharmacy in the interests of pharmacists. The financing for such an
organization must be on a voluntary basis. We have recommended a procedure to
assist immediate implementation of this recommendation.
Chapter 8 – Communication
26. We recommend the formation of vigorous local organizations in all areas with
the inititative being provided by pharmacists in the individual districts.
27. We recommend a properly conceived and financed attack on our public relations
Chapter 9 – Economic Considerations
28. We recommend that pharmacists pay particular attention to the resolution of
CPhA that when dispensing a prescription by its proper name, (we) continue to
consider the interests of the patient and use a drug having both high quality and
reasonable price and that . a brand name of a drug product does not necessarily
confer reasonable price nor is it the sole guide of quality.
29. We recommend that pharmacy take the initiative in encouraging physicians to
adopt generic nomenclature for prescriptions. This would remove a major
stumbling block which has restricted pharmacy in its attempt to provide
economical prescription service.
30. We recommend that cost plus professional fee be the method used for determining
prescription prices.
Chapter 10 – Health Care Plans
31. We conclude that it would be unwise for Pharmacy to attempt to establish its own
drug insurance program. We recommend that Pharmacy support the developmetn
by other carriers of Extended Health Benefits which include prescription
coverage, and that we maintain liason to ensure the maintenance of equitable
Chapter 11 – Governments
32. We recommend that in negiotiations with governments involving the economics
of the profession there be a greater degree of consultation with and involvement
of practicing pharmacists.
33. We recommend that the proposed alterations in the regulations applying to the
distribution of veterinary drugs and medicated feeds be implemented, and that the
provisions of the Pharmacy Act as they apply to this field be enforced
Chapter 12 – Suppliers
34. We recommend that pharmacists individually and collectively pursue solutions to
the problem of the costs of merchandise as they apply at the wholesale and
manufacturer's level, with particular attention to the attitudes of certain
Chapter 13 – Legislation and By-laws
35. We recommend certain alterations in the fee structure of the statutory
organization.232
232 UBC-SM-CPBC, Box 12A-10, PPC Report, ix-xiii.
Appendix G
Principles of Pharmaceutical Ethics (adopted by APhA August 17, 1922)
(Adopted by CPhA in 1923 as the basis of a Canadian Code of Ethics)
Chapter 1 The Duties of the Pharmacist in Connection with his Services to the
Public
Pharmacy has for its primary object the service which it can render to the public in
safeguarding the handling, sale, compounding and dispensing of medicinal substances.
The practice of pharmacy demands knowledge, skill and integrity on the part of those
engaged in it. Pharmacists are required to pass certain educational tests in order to qualify
under the laws of our States. The States thus restrict the practice of pharmacy to those
persons who by reason of special training and qualifications are able to qualify under
regulatory requirements and grant to them privileges necessarily denied to others. In
return the States expect the Pharmacist to recognize his responsibility to the community
and to fulfill his professional obligations honourably and with due regard for the physical
and moral well being of society. The Pharmacist should uphold the approved legal
standards of the United States Pharmacopoeia and the National Formulary for articles
which are official in either of these works, and should, as far as possible, encourage the
use of these official drugs and preparations and discourage the use of objectionable
nostrums. He should sell and dispense only drugs of the best quality for medicinal use
and for filling prescriptions. He should neither buy, sell nor use substandard drugs for
uses which are in any way connected with medicinal purposes. The Pharmacist should be
properly remunerated by the public for his knowledge and skill when used in its behalf in
compounding prescriptions, and his fee for such professional work should take into
account the time consumed and the great responsibility involved as well as the cost of the
ingredients. The Pharmacist should not sell or dispense powerful drugs and poisons to
persons not properly qualified to administer or use them, and should use every proper
precaution to safeguard the public from poisons and from all habit-forming medicines.
The Pharmacist, being legally entrusted with the dispensing and sale of narcotic drugs
and alcoholic liquors, should merit this responsibility by upholding and conforming to the
laws and regulations governing the distribution of these substances. The Pharmacist
should seek to enlist and merit the confidence of his patrons and when this confidence is
won it should be jealously guarded and never abused by extortion or misrepresentation or
in any other manner. The Pharmacist should consider the knowledge which he gains of
the ailments of his patrons and their confidences regarding these matters, as entrusted to
his honour, and he should never divulge such facts unless compelled to do so by law. The
Pharmacist should hold the health and safety of his patrons to be of first consideration: he
should make no attempt to prescribe or treat diseases or strive to sell drugs or remedies of
any kind simply for the sake of profit. He should keep his pharmacy clean, neat and
sanitary in all its departments and should be well supplied with accurate measuring and
weighing devices and other suitable apparatus for the proper performance of his
professional duties. It is considered inimical to public welfare for the Pharmacist to have
any clandestine arrangement with any Physician in which fees are divided or in which
secret prescriptions are concerned. The Pharmacist should primarily be a good citizen,
and should uphold and defend the laws of the State and nation. He should inform himself
concerning the laws, particularly those relating to food and drug adulteration and
sanitation and should always be ready to co-operate with the proper authorities having
charge of the enforcement of the laws. The Pharmacist should be willing to join any
constructive effort to promote the public welfare and he should regulate his public and
private conduct and deeds so as to entitle him to the respect and confidence of the
community in which he practices.
Chapter 2 The Duties of the Pharmacist in His Relation to the Physician
The Pharmacist even when urgently requested so to do should always refuse to prescribe
or attempt diagnosis. He should, under such circumstances, refer applicants for medical
aid to a reputable legally qualified Physician. In cases of extreme emergency as in
accident or sudden illness on the street in which persons are brought to him pending the
arrival of a Physician such prompt action should be taken to prevent suffering as is
dictated by humanitarian impulses and guided by scientific knowledge and common
sense. The Pharmacist should not, under any circumstances, substitute one article for
another, or one make of an article for another in a prescription without the consent of the
Physician who wrote it. No change should be made in a Physician's prescription except
such as is essentially warranted by correct pharmaceutical procedure, nor any that will
interfere with the obvious intent of the prescriber, as regards therapeutic action. He
should follow the Physician's directions explicitly in the matter refilling prescriptions,
copying the formula upon the label or giving a copy of the prescription to the patient. He
should not add any extra directions or caution or poison labels without due regard for the
wishes of the prescriber, providing the safety of the patient is not jeopardized. Whenever
there is doubt as to the interpretation of the Physician's prescription or directions, he
should invariably confer with the physician in order to avoid a possible mistake or an
unpleasant situation. He should never discuss the therapeutics effect of a Physician's
prescription with a patron nor disclose details of composition which the Physician has
withheld, suggesting to the patient that such details can be properly discussed with the
prescriber only. Where an obvious error or omission in a prescription is detected by the
Pharmacist, he should protect the interests of his patron and also the reputation of the
Physician by conferring confidentially upon the subject, using the utmost caution and
delicacy in handling such an important matter.
Chapter 3 The Duties of Pharmacists to Each Other and to the Profession at Large
The Pharmacist should strive to perfect and enlarge his professional knowledge. He
should contribute his share toward the scientific progress of his profession and encourage
and participate in research, investigation and study. He should associate himself with
pharmaceutical organizations whose aims are compatible with this code of ethics and to
whose memberships he may be eligible. He should contribute his share of time, energy
and expense to carry on the work of these organizations and promote their welfare. He
should keep himself informed upon professional matters by reading current
pharmaceutical and medical literature. He should perform no act, nor should he be a party
to any transaction which will bring discredit to himself or to his profession or in any way
bring criticism upon it, nor should be unwarrantedly criticise a fellow Pharmacist or do
anything to diminish the trust reposed in the practitioners of pharmacy. The Pharmacist
should expose any corrupt or dishonest conduct of any member of his profession which
comes to his certain knowledge, through those accredited processes provided by the civil
laws or the rules and regulations of pharmaceutical organizations, and he should aid in
driving the unworthy out of the calling. He should not accept agencies nor objectionable
nostrums nor allow his name to be used in connection with advertisements or
correspondence for furthering their sale. He should courteously aid a fellow Pharmacist
who may request advice or professional information, or who in an emergency, needs
supplies. He should not aid any person to evade legal requirements regarding character,
time or practical experience by carelessly or improperly endorsing or approving
statements relating thereto. He should not imitate the labels of his competitors nor take
any other unfair advantage of merited professional or commercial success. When a bottle
or package of a medicine is brought to him to be refilled, he should remove all other
labels and place his own thereon unless the patron requests otherwise. He should not fill
orders which come to him by mistake, being originally intended for a competitor. He
should deal fairly with manufacturers and wholesale druggist from whom he purchases
his supplies; all goods received in error or excess and all undercharges should be as
promptly reported as are shortages and overcharges. He should earnestly strive to follow
all proper trade regulations and rules, promptly meet all obligations and closely adhere to
all contracts and agreements.233
The Code of Ethics of Pharmacists in British Columbia
(drafted by Joint Association-Society Code of Ethics Committee: adopted March 1969) I, Pharmacist Name
Do hereby promise to accept those responsibilities vested in me as a Pharmacist in
the pursuit of fulfillment of the health needs of my community.
That I will place above all other considerations, my regard and concern to provide
the highest level of patient care possible by the use of my skill, and judgment and by co-
operation with other members of the health sciences.
That I will strive to attain the highest degree of personal quality, attitude and
objectivity, all of which will result from constant vigilance in practicing my profession
That I will participate in programs of continued study throughout my professional
life, in order to keep abreast of new advances in pharmaceutical practice and technique
and in order to maintain a high level of competence in working with other health
practitioners. 233 "Principles of Pharmaceutical Ethics," Canadian Pharmaceutical Journal, Vol LVII No. 2 (Sep 1923): 18 & 24.
That I will seek to be regarded by the public, my colleagues, members of the other
health professions and my business associates as a law-abiding citizen, evidenced by
compliance and performance.
That I will actively support to the best of my ability, organizations engaged in the
provision of high standards of pharmaceutical service and professional behaviour,
thereby contributing to the advance of the public health.
Signed by Pharmacist234
Schedule A – Code of Ethics Adopted 2009
All pharmacists practicing in British Columbia are governed by a Code of Ethics. By
entering the profession of pharmacy, every pharmacist commits to moral norms of
conduct. We assume a professional commitment to the health and well-being of every
one of our patients.
Pharmacists respect the professional relationship with the patient and acts with honesty,
integrity and compassion.
Pharmacists honour the individual needs, values and dignity of the patient.
Pharmacists support the right of the patient to make personal choices about pharmacy
Pharmacists provide competent care to the patient and actively supports the patient's right
to receive competent and ethical care.
Pharmacists protect the patient's right of confidentiality.
Pharmacists respect the values and abilities of colleagues and other health professionals.
234 UBC-SM-CPBC, Box 27-1, Report the Joint Association-Society Code of Ethics Committee, BCPhA council meeting October 1968, 39-40.
Pharmacists endeavour to ensure that the practice environment contributes to safe and
effective pharmacy care.
Pharmacists ensure continuity of care in the event of job action, pharmacy closure or
conflict with moral beliefs.235
235 College of Pharmacists of British Columbia, "Code of Ethics",
> (June 21, 2010).
Source: http://www.cahp.ca/documents/Masters%20Thesis%20Submission%20Copy%20August%2018.pdf
Microsoft word - sangalli_lamieri.docx
A spatial econometric model for productivity and innovation in the manufacturing industry: the role played by geographical and sectorial distances between firms° Ilaria Sangalli*, Marco Lamieri** Abstract The paper assesses spillovers from total factor productivity (TFP) in the Italian
grstiftung.ch
20 Wissen FREITAG, 15. MÄRZ 2013 / WWW.20MINUTEN.CH 15 Jahre Viagra: Er steht und steht Den Augen trauenBASEL. Optische Täuschungen können ganz schön für Verwir- NEW YORK. Viagra ist das Potenzmittel überhaupt. nicht gegen Herz-Kreislauf-Er- gen bringt Pfi zer es im März rung sorgen. Basler Wissen- Dabei war das Präparat ursprünglich zur Behandlung