Physioinfo.co.za
Management of Patellofemoral PainTargeting Hip, Pelvis, and Trunk Muscle
Function: 2 Case Reports
Catherine L. Mascal, PT, BSc1Robert Landel, DPT, OCS2Christopher Powers, PT, PhD3 Study Design: Case report.
Objective: To describe an alternative treatment approach for patellofemoral pain.
Background: Weakness of the hip, pelvis, and trunk musculature has been hypothesized to
influence lower-limb alignment and contribute to patellofemoral pain. Two patients who had a
Patellofemoral pain (PFP) is recognized asone of the most com-mon chief complaint of patellofemoral pain and demonstrated lack of control of the hip in the frontal disorders encountered and transverse planes during functional movements were treated with an exercise program by orthopaedic physical thera- targeting the hip, pelvis, and trunk musculature.
pists.28,59 Despite its prevalence, Methods and Measures: The patients presented in these 2 case reports did not exhibit obvious
however, the etiology of this pain patellar malalignment or tracking problems; however, on qualitative assessment, both demon-strated excessive hip adduction, internal rotation, and knee valgus during gait and while syndrome and specific treatment performing a step-down maneuver. In addition, both patients exhibited weakness of the hip of this condition remain vague abductors, extensors, and external rotators, as demonstrated by hand-held dynamometry testing.
and controversial.
Treatment in both cases occurred over a 14-week period and focused on recruitment and The premise behind most treat- endurance training of the hip, pelvis, and trunk musculature. Functional status, pain, muscle force ment approaches is that PFP is the production, as well as subjective and objective assessment of lower-extremity kinematics during result of abnormal patellar track- gait and a step-down maneuver were assessed preintervention and postintervention.
ing and/or malalignment. Given Results: Both patients experienced a significant reduction in patellofemoral pain, improved
as such, interventions are often lower-extremity kinematics during dynamic testing, and were able to return to their original levels focused locally, and typically in- of function. Gluteus medius force production improved by 50% in patient A and 90% in patient B, clude quadriceps strengthening, while gluteus maximus force production improved 55% in patient A and 110% in patient B.
patellar taping, patellar bracing, Objective kinematic improvements in the step-down task also were demonstrated in patient A.
stretching, and soft tissue mobiliza- Conclusion: Assessment and treatment of the hip, pelvis, and trunk musculature should be
tion.6,19,46,59 Despite the longevity considered in the rehabilitation of patients who present with patellofemoral pain and demonstrate of such treatment approaches, abnormal lower-extremity kinematics. J Orthop Sports Phys Ther 2003;33:642-660. with papers as early as 1922 advo- Key Words: case study, knee pain, lower-extremity rehabilitation, therapeutic
cating quadriceps strengthening exercises,35 intervention outcomeshave been mixed.2,11,29,30 In addi-tion, the 2001 Philadelphia Panel systematic review failed to find a 1 Staff Physical Therapist, Kern and Associates Physical Therapy, Santa Monica, CA. At the time these sufficient number of high-quality cases were managed, Catherine Mascal was a resident in the Orthopaedic Physical Therapy Residency randomized control trials to rec- Program at the University of Southern California, Los Angeles, CA. ommend any clinically important 2 Associate Professor of Clinical Physical Therapy, Department of Biokinesiology and Physical Therapy, benefit from exercise, massage, University of Southern California, Los Angeles, CA.
3 Associate Professor and Director, Musculoskeletal Biomechanics Research Laboratory, Department of heat, or combined therapies for Biokinesiology and Physical Therapy, University of Southern California, Los Angeles, CA. patients with PFP.44 Send correspondence to Christopher M. Powers, Department of Biokinesiology and Physical Therapy, One possible reason for the rela- University of Southern California, 1540 E. Alcazar Street, CHP 155, Los Angeles, CA 90089-9006. E-mail: tively poor outcomes associated [email protected] methods described in this paper are standard care for patients seen in this clinic. Therefore, with the treatment of PFP may be Institutional Review Board approval was not necessary for these case reports. related to the assumption that Journal of Orthopaedic & Sports Physical Therapy subluxation is the result of the patella moving on the quadriceps strengthening exercises. She also was femur. While this may be the case during non–weight- given a neoprene support that she wore regularly bearing activities in which the femur is fixed (eg, while working as a waitress. Radiographic work-up during knee extension in sitting), recent evidence included axial view radiographs taken in June 2001 suggests that subluxation during weight-bearing activi- that were unremarkable. The severity of pain had ties may be the result of the femur rotating under- gradually become worse over the previous 2 years, neath the patella in the transverse plane.60 Therefore, however, she was not taking pain medication. She a treatment program that addresses the control of described no other ipsilateral or contralateral lower- femoral motion may play a role in the treatment of extremity symptoms.
certain patients with PFP.
Patient B described a 2-year history of right patel- When treating patients with PFP who demonstrate lofemoral pain. The onset of symptoms was insidious, lack of control of hip adduction and internal rotation with no known precipitating event. The severity of during weight-bearing activities such as walking and the condition had progressed to the point that she descending stairs, one goal may be to optimize had fallen 3 times over the last 18 months due to a muscle function to control these motions, as such painful giving-way of her knee. She took Naproxen movement can result in genu valgus, an increase in only when the pain was severe (approximately 2 to 3 the dynamic Q angle, and greater lateral forces acting times a week). She had not undertaken any previous on the patella.9,21-23,40,45 With this in mind, it also physical therapy treatment. Work-up included axial would appear reasonable to strive for optimal func- view radiographs taken in March 2002 that were tion of the abdominal, pelvis, and spinal musculature, unremarkable. She described no other ipsilateral or as it is theorized that this is an important factor when contralateral lower-extremity symptoms.
addressing lower-extremity muscle strength train-ing.10,18,47,50 To date, no patient outcomes have been described for an intervention focusing on control ofhip and pelvis motion in individuals with PFP.
Patient A's symptoms were described as an inter- The purpose of these 2 case reports was to illus- mittent sharp pain in the right retropatellar region.
trate that an exercise program focusing primarily on She stated that walking for 2 hours, or descending 2 the hip, pelvis, and trunk musculature could have a flights of stairs exacerbated her pain. Alleviating positive effect on PFP, functional status, and lower- factors included ice, rest, and a neoprene knee limb positioning during gait and a step-down task. As support. Her activity level included 3 days a week at one of the hallmark signs of PFP is an exacerbation college, with prolonged periods of sitting in class, and of symptoms during stair descent,9,24 2 patients are working as a waitress in a restaurant for 3 other days presented who reported pain and the inability to during the week. Typically, her symptoms occurred control motion at the hip during this activity.
after working for 2 hours, at which time she wouldstart wearing the neoprene support. Patient A did not participate in any regular physical exercise, but stateda desire to start jogging, which she had not done for the previous 4 to 5 years.
Patient B's symptoms were described as an inter- Patient A was a 20-year-old female with a body mass mittent throbbing right retropatellar pain that was index (BMI) of 22 (normal weight). She was a aggravated by stair descent. Alleviating factors in- part-time student and also worked three 10-hour days cluded rest and Naproxen. Patient B stated that she a week as a waitress in a restaurant. Patient B was a enjoyed walking for 30 to 45 minutes, 3 to 4 times a 37-year-old female with a BMI of 27 (somewhat week; however, she had not been able to do this for overweight). She worked full time as an accounts the last 3 weeks due to the increased severity of her assistant in a hospital finance department.
Patient A's goals were to commence a jogging History of Presenting Condition
program and to be able to work at the restaurantpain free, without the use of her neoprene support.
Patient A described a history of right patel- Patient B's goals were to return to her previous level lofemoral pain, which commenced after traumatically of walking, go dancing once a week, and ascend/ dislocating her patella twice, 9 and 2 years prior. In descend stairs pain free.
both instances, the mechanism was described as anawkward fall onto a twisted knee, and the patella was TESTS AND MEASURES
self-reduced following the trauma. After the lastdislocation in November 2000, she underwent an As regular clinical service was being provided for unsuccessful course of physical therapy that consisted these 2 patients, both were exempt from requiring of a progressive aerobic walking program and Institutional Review Board approval.
J Orthop Sports Phys Ther • Volume 33 • Number 11 • November 2003 Patellofemoral Joint Examination
Prior to treatment, both patients completed a Examination of the patellofemoral joint included self-administered functional assessment tool that has static and dynamic patellar positional tests that have been validated for the evaluation of patellofemoraljoint disorders (Appendix).33 This questionnaire is been described elsewhere.9,18,61 Although these pro- used to qualitatively assess an individual's functional cedures have been shown to demonstrate poor-to-fair status and patellofemoral pain experienced during intertester reliability,17 the purpose of using them in specific functional tasks. The maximum total score of these case reports was to identify any gross positional this assessment tool is 100, with higher scores indicat- abnormalities. Assessment of static patellar position ing greater levels of function with lower levels of and orientation was performed for medial/lateral pain. The preintervention function scores were 76 glide, medial/lateral rotation, and anteroposterior and 70 for patient A and patient B, respectively.
and lateral tilt, as described by McConnell.18 Assess-ment of dynamic patellar tracking was performedduring non–weight-bearing knee extension (45°-0°).
Neither patient demonstrated any obvious anomalies Both patients used a 10-cm visual analogue scale in terms of static patellar alignment or dynamic (VAS) to indicate the greatest amount of pain during their most pain-provoking activities, with 0 represent- Clinical tests that have been described to assess ing no pain and 10 representing the worst pain patellofemoral dysfunction also were performed.29 imaginable. This method of evaluation has been These included the patellar compression test54 and shown to be both reliable and valid for measuring the apprehension (Fairbanks) test.14 Passive patellar pain.13,48,53 The initial VAS score for patient A was mobility was examined and compared to the unaf- 5/10 after walking for 2 hours, and 4/10 after fected side. Symptom reproduction was evaluated climbing 2 flights of stairs. The initial VAS score for during resisted knee extension at various knee flex- patient B ranged from 7/10 while descending a ion angles and palpation was performed for single step to 10/10 on descending an entire flight. A retinaculum tenderness. Patient A presented with a VAS score of 8/10 was reported for walking 2 miles.
positive compression and apprehension test, and painwith resisted knee extension from 10° to 0° of knee Differential Diagnostic Screening
flexion. She had normal passive patellar mobility.
Patient B had slight pain on patellar compression and Active, passive, and accessory mobility of the moderate tenderness with palpation of the right rearfoot, tibiofemoral joint, hip joint, and lumbar medial retinaculum. She had pain on resisted knee spine were assessed. Clinical tests as described in extension from 20° to 0° knee flexion, and had Magee36 were carried out to eliminate these struc- normal passive patellar mobility with slight pain at tures as potential sources of the subjects' symptoms.
end range medial and lateral translation.
This screening examination revealed no abnormali- Quadriceps strength was assessed using a Microfet2 ties and both patients demonstrated a full pain-free hand-held dynamometer (Hoggan Health Industries, range of knee motion. Negative test results were also Inc., Draper, UT). This method of measuring muscle found for the following conditions: ligamentous insta- strength has been validated and the intertester reli- bility of the knee; intracapsular knee pathology; ability has been shown to be good to excellent.3-5 patellar tendonitis; pes anserine bursitis; iliotibial Quadriceps muscle strength testing was performed in band friction syndrome; and referred pain from the the position recommended by Kendall31; however, the hip, sacroiliac region, or lumbar spine.
knee was maintained in 30° of flexion to avoid TABLE. Hand-held dynamometry, preintervention and postintervention results. Values given are the average of 3 trials. Numbers in pa-
rentheses are subjective muscle strength ratings based on an isometric break test where 5/5 is maximal strength (ie, unable to ‘‘break''
the muscle's isometric hold).38
Patient A
Patient B
Force (N)
Force (N)
Force (N)
Force (N)
Hip lateral rotator group Hip medial rotator group J Orthop Sports Phys Ther • Volume 33 • Number 11 • November 2003



quadriceps inhibition due to pain. Resistance was
and external rotators of the hip, and the abdominal
given at the distal tibia, 10 cm proximal to the lateral
musculature. Muscle strength testing of the hip was
malleolus, and the average of 3 trials was recorded.
performed using a hand-held dynamometer in test
Preintervention force results are presented in the
positions described by Kendall.31 Subjectively, both
Table. Patient A was subjectively assigned a manual
patients demonstrated significant weakness of the
muscle test grade of 3+/5, while patient B was
ipsilateral gluteus medius (grade 3+/5 in both cases),
assigned a manual muscle test grade of 4/5.
and gluteus maximus (grade 4⫺/5 and 3+/5 forpatients A and B, respectively). In addition, signifi-
cant ipsilateral weakness of the hip lateral rotatorswas observed in patient A (grade 3+/5). The force
Lower-extremity alignment was assessed qualitatively
and quadriceps values recorded with the hand-held
in a relaxed standing posture. Neither patient dem-
dynamometer during these muscle tests are presented
onstrated significant rearfoot varus/valgus or genu
in the Table.
varus/valgus. There also was no observable squinting
Tests to ascertain neuromuscular control of pelvic
of the patellae, which is indicative of femoral antever-
motion have been described in detail by Sahrmann50
sion. This was confirmed by performing Craig's test
and Farrell.15 Four of these tests were performed and
in prone.36 Limb length (as measured from the
included: (1) evaluation of the patient moving from
anterior superior iliac spine to the medial malleolus)
double- to single-limb stance, noting signs of pelvic
was assessed bilaterally in the supine position and was
drop and observing the lateral translation of the
found to be equal when measured to the nearest 0.5
pelvis; (2) maintenance of a static bridge position
against a manual rotational displacement force ap-plied to the pelvis in the transverse plane; (3)
evaluation of the patients' ability to prevent pelvictilting in the frontal plane during a single-hip abduc-
Gait Observational gait analysis was performed as
tion motion in a sidelying position; and (4) preven-
the patients walked at a self-selected pace along a
tion of pelvic motion in the transverse plane during
10-m walkway. Both patients demonstrated normal
an abduction/external rotation movement of the hip
sagittal plane motion of the ankle, knee, and hipjoints. Abnormalities were noted, however, in thefrontal and transverse planes. During stance phase onthe affected side, the following deviations were ob-served: (a) excessive hip adduction during weightacceptance, (b) excessive internal hip rotation inearly midstance, and (c) notable contralateral pelvicdrop during midstance. These deviations were evi-dent in both patients. Neither demonstrated excessiveor prolonged subtalar joint pronation or excessivetibial internal rotation during the stance phase ofgait.
Step-Down Task Patients also were evaluated dynami-
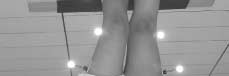
cally during an activity that required greater demandson the lower-extremity muscles. The step-down taskinvolved observing each patient stepping down slowlyfrom a 20.4-cm-high (8-in) step during a 3-secondperiod. Both patients demonstrated significant hipadduction and slight internal rotation of the stancelimb and an appreciable contralateral pelvic drop. Inboth cases, this motion resulted in substantial valgusat the knee (Figure 1).
Muscle Strength Examination: Hip and Abdominal
Musculature
Based on the significant frontal and transverse
plane deviations at the hip during the dynamicexamination, a decision was made to assess the
FIGURE 1. Photograph of patient A demonstrating marker place-
strength of the hip and trunk muscles. These in-
ment and experimental setup. Prior to the intervention, substantial
cluded the gluteus maximus, gluteus medius, internal
knee valgus was observed during this procedure.
J Orthop Sports Phys Ther • Volume 33 • Number 11 • November 2003
in hook lying. Spinal or pelvic motion during tests (3
and 4) was evaluated by palpating the anterior
superior iliac spines (ASIS). Both patients demon-
strated poor control of motion as demonstrated bysignificant observable and palpable translation of the
pelvis during all of the above tests.
In addition to the physical examination, patient A
Musculoskeletal Biomechanical Research Laboratoryat the University of Southern California. The purpose
of this testing was to document lower-extremity kine-matics during the step-down maneuver and to pro-
vide objective data for posttreatment comparison.
Hip Rotation Angle (degrees)
Three-dimensional kinematics of the lower extrem-
ity were obtained using methodology described in
previous publications.51,52 Data were obtained whilepatient A performed a step-down maneuver from a
20.4-cm-high (8-in) step with the symptomatic side as
the supporting limb (Figure 1). The patient was
instructed to perform this maneuver slowly over thecourse of 3 seconds. Three trials of data were
collected and averaged for analysis. Variables of
interest were hip adduction, hip internal rotation,and contralateral pelvic drop. When averaged across
the entire stance phase, patient A demonstrated 1.4°of hip internal rotation, 8.7° of hip adduction, and
3.9° of contralateral pelvic drop during the step-down
test (Figure 2).
Hip Adduction Angle (degrees)
Given the subjective and objective information
obtained in the examination, it was our impressionthat neither patient demonstrated significant abnor-
malities specific to the patellofemoral joint that couldaccount for subjective complaints of PFP. Both pa-
tients, however, demonstrated significant weakness of
the hip and abdominal musculature, and a reduced
ability to control hip and pelvis motion during
dynamic testing. We theorized that this poorneuromuscular control was responsible for the in-
creased internal rotation/adduction of the hip ob-
served during gait and the step-down maneuver, and
that these femoral motions may have contributed to
the PFP symptoms.45 Therefore, it was our hypothesis
that exercises focused on addressing the documented
muscular weaknesses and abnormal movement pat-
terns would aid in pain resolution, improve func-
tional status, and result in improved gait kinematics
Pelvic Obliquity (degree) -5
during level walking and the step-down maneuver.
Foundations for Treatment
FIGURE 2. Kinematic plots demonstrating patient A's lower-
extremity motion (preintervention and postintervention) during the
Both patients were scheduled to attend physical
step-down task. (A) Hip internal rotation. (B) Hip adduction. (C)
therapy once or twice a week over a 3-month period.
Frontal plane pelvic motion of the contralateral pelvis.
J Orthop Sports Phys Ther • Volume 33 • Number 11 • November 2003



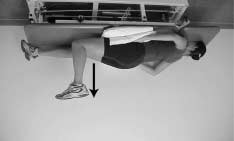
FIGURE 3. Non–weight-bearing exercises performed with the spine
maintained in a neutral position (weeks 0-6). (A) Alternate hip andknee flexion/extension motions. (B) Gluteus medius exercises involv-ing hip abduction/external rotation. (C) Progression of gluteusmedius exercise. Placing the uppermost knee in extension increasesthe lever arm. The hip should be held in less than 25° externalrotation and slight extension. (D) Gluteus maximus strengtheningwas facilitated by extending the hip with the knee held in greaterthan 90° of knee flexion. Anterior pelvic tilt palpated by thepatient's fingers on the anterior superior iliac spine indicates endrange active hip extension. (E) Hip abductor and external rotatorstrengthening was progressed by assuming a quadruped startingposition and performing an external rotation/abduction/extension
motion of the lower extremity against gravity.
The patients were educated regarding their conditionand the intended treatment approach and realisticgoal setting was discussed.
Both patients were placed on an exercise program
initially focused on controlling pelvic motion whileperforming active lower-extremity movement. Accord-ing to Nadler et al,41 it is important to establishsatisfactory lumbopelvic control to ensure that theproximal attachment site for the hip abductors andlateral rotators is stable. Such stability is thought to
promote greater torque production by these muscles
during exercise and minimize frontal-plane motion(ie, contralateral pelvic drop or spinal side flexion)during single-limb stance activities.
The hip muscles (particularly gluteus maximus and
medius, hip abductors, and lateral rotators) wereprogressively strengthened first in the non–weight-bearing position, then in the weight-bearing position,using functional movement patterns. By focusing onthe maintenance of a stable pelvis while introducingactive hip motions, it was thought that proprioceptiveawareness also would be enhanced.15,50,58
Specific recommendations for muscle strength
training are controversial and a variety of trainingprotocols have been established. It is generallyagreed, however, that an exercise load that causesfatigue after 10 to 15 repetitions for 2 to 3 sets,performed 3 times a week for 6 to 12 weeks, will leadto improved muscle strength.16,32,47
Based on these parameters, a progression criterion
for the proposed exercise program was formulated.
When the patient could perform a specific exercise(or a 10-second isometric muscle contraction), for 2
sets of 15 repetitions, while maintaining a neutral
spinal position, the exercise would be progressed byincreasing resistance. Both patients were given ahome exercise program that they were to performtwice daily. The home program paralleled the exer-cises given in the clinic, and each patient was deemedready to commence a new exercise at home when thepatient was able to correctly carry out the movementin the clinic with minimal verbal prompts.
As muscle strength and motor control improved,
patients were progressed to complex coordinatedmotor patterns involving functional activities. At this
time, they gradually reinstituted their previous in-
J Orthop Sports Phys Ther • Volume 33 • Number 11 • November 2003
volvement in identified sport and social activities.
their ASIS ipsilateral to the side of lower-extremity
Specific details concerning the various exercises em-
motion. This was done to ascertain when pelvic
ployed are discussed below.
rotation occurred. The patients were instructed tostop when movement was felt. Throughout the re-
Non–Weight-Bearing Exercise (Weeks 0-6)
maining exercise progressions, the patients were con-tinually encouraged to maintain a static pelvic
Prior to initiating the dynamic strengthening pro-
position, with emphasis being placed on the patients
gram of the hip musculature, the patients were
self-monitoring their performance using tactile and
taught to perform isometric contractions of the
visual (mirror) feedback.
abdominals, gluteus medius, and gluteus maximus.
Performing the sidelying hip abduction exercise
Abdominal strengthening exercises were performed
with an extended knee initially increased the resis-
in a hook-lying position as described by Taylor and
tance of the previously described exercise (Figure
O'Sullivan.58 A pressure cuff provided feedback of
3C). To isolate the gluteus medius and minimize
the spinal position during the hook-lying exercise.
tensor fascia lata activity, the hip was maintained in a
The cuff was placed between the lumbar spine and
slightly extended position and externally rotated to
the treatment table and inflated slightly. The patients
less than 25°.43 Care was taken that the pelvis and
were asked to maintain a stable pressure reading
lumber spine remained stable throughout, ensuring
(interpreted as minimal spinal motion), while per-
isolation of the movement to the hip joint.
forming concurrent hip and knee flexion with alter-
During this time, gluteus maximus exercises were
nate legs (Figure 3A). Following principles of motor
also given in a prone position over a pillow with the
learning and skill acquisition,62 the pressure cuff
knee held in at least 90° flexion (Figure 3D).50
feedback was provided at a reduced schedule and
Patients were instructed to extend their slightly exter-
gradually removed.
nally rotated hip until they felt approximation of the
Isometric strengthening exercises for the gluteus
ASIS on the pillow indicating an anterior tilt of the
medius were performed in sidelying with the hips
pelvis and lumbar spine extension. Throughout the
and knees slightly flexed to minimize contribution
range of motion, the patients were encouraged to
from the tensor fascia lata (TFL). The TFL was
focus on contraction of the gluteal muscles and
judged to be contributing excessively when there was
minimize activity of the hamstrings.
palpable activity in the muscle belly during the
When patients were able to perform 2 sets of 15
exercise. Initially, patient B had great difficulty in
repetitions of the above exercises, they were pro-
minimizing TFL activity. She was, therefore, in-
gressed to the quadruped position to perform hip
structed to initiate her isometric gluteus medius
external rotation/abduction, and hip extension (Fig-
contractions in sidelying in front of a wall with her
ure 3E). The demand was further increased by
feet against it, so that by applying slight pressure to
applying an external load using either Theraband
the wall, active hip extension was encouraged,
(Hygenic Corporation, Akron, OH) tied around the
thereby reinforcing the gluteus medius contraction.
thighs, or a soft weight around the ankles. The
Isometric gluteus maximus exercises were per-
amount of weight was increased, using the guidelines
formed as described by Sahrmann.50 This involved
mentioned previously, in 1-lb (0.5-kg) increments.
lying in prone with 1 knee flexed to 90°. The patientswere instructed to contract the ipsilateral gluteal
Weight-Bearing Exercise (Weeks 6-10)
muscle, while keeping the leg as relaxed as possible,thus minimizing hamstring muscle activity.
Once the patients were able to isolate the muscles
When a stable spinal position could be maintained
of interest during non–weight-bearing exercises, they
while performing concurrent hip and knee flexion
were progressed to weight-bearing exercises, which
with alternate legs, and the progression criteria were
included isometric and dynamic exercises in single-
achieved for isometric gluteus maximus and medius
limb stance. At this time the patients were introduced
contractions, the patients were progressed to dynamic
to the concept of neutral lower-extremity alignment
exercises. This occurred at week 3 for patient A, and
as described by McConnell.38 This involved alignment
week 4 for patient B. The subsequent program of
of the lower extremity such that the ASIS and knee
dynamic hip-strengthening exercises for the lateral
remained positioned over the second toe, with the
rotators and the abductors of the hip predominately
hip positioned in approximately 10° of external
targeted the gluteus medius and maximus.
Gluteus medius exercises were done in sidelying,
The patients were then instructed to stand next to
with hips and knees flexed, performing hip abduc-
a wall with the stance limb furthest from the wall.
tion with external rotation, while maintaining a
They were asked to contract their transversus
neutral spinal position by coactivating the transversus
abdominus and gluteal muscles and then to assume a
abdominus (Figure 3B). The patients were instructed
single-limb stance position by flexing the contralateral
to keep both feet together and lift the uppermost
knee with the hip in a neutral position (Figure 4A).
knee as high as possible, while concurrently palpating
Patients then performed isometric external rotation
J Orthop Sports Phys Ther • Volume 33 • Number 11 • November 2003
of the stance leg while concurrently pushing the bent
the trunk stability musculature and more springs
leg into the wall. No movement of the pelvis was
increasing the lower-extremity demand. Postural
allowed, as confirmed by palpating the ASIS. In
alignment and symmetrical strengthening were em-
addition to challenging the abductors and external
phasized during all exercises.55 To target the hip
rotators of the unsupported leg, this exercise also
abductors and trunk muscles, the patients stood on
required the stance leg to maintain relative hip
the Clinical Reformer, assuming a neutral lower-
abduction despite the creation of an adduction
extremity alignment, with 1 foot on the carriage.
torque by the body's center of mass during single-
They were then instructed to perform a double hip
abduction movement against light resistance while
When the patients were able to perform 2 sets of
maintaining a level pelvic position and neutral lower-
fifteen 10-second repetitions of this exercise without
extremity alignment (Figure 4C).
excessive motion of the pelvis or lower extremity,
Using the stated progression criteria, the patients
simultaneous upper-extremity exercises in single-limb
were instructed to maintain a neutral lower-extremity
stance were added. The exercise initially involved
alignment while in single-limb stance, and to rotate
ipsilateral upper-extremity activities and was then
the upper body and trunk medially against resistance
progressed to include the contralateral arm.
provided by Theraband (Figure 4D). This task pro-
Evidence suggests that performing exercises in
duced relative external rotation of the hip performed
single-limb stance enhances gluteus medius activity,20
in a weight-bearing position.
and carrying a load in the arm contralateral to thestance limb leads to higher gluteus medius EMGactivity than if applied on the ipsilateral side.42
Functional Training (Weeks 10-14)
Patients were given a combination of fast upper-extremity activities, such as ball throws against a wall,
To reinforce the concept of maintaining neutral
alternate biceps curls, and rowing exercises, using
lower-extremity alignment during functional tasks, the
Theraband and pulley systems (Figure 4B) to provide
patients were introduced to shallow-squatting activi-
light resistance. Throughout these tasks, the patients
ties. These were initially performed on the Clinical
were instructed to maintain neutral lower-extremity
Reformer, using a leg press motion (Figure 5A). The
and pelvis alignment, palpating the ASIS of the
benefit of utilizing the Clinical Reformer is that it
stance limb using the free hand to monitor motion.
allows the subject to perform a weight-bearing activity
At week 8, weight-bearing exercises for the abduc-
with a load significantly less than body weight. This
tors and external rotators of the hip were added.
will lessen joint reaction forces,7,37 especially if per-
These were undertaken using the Clinical Reformer
formed in knee flexion ranges less than 45°.57 The
Pilates exercise equipment (Current Concepts Corp.,
exercise was then progressed by securing Theraband
Sacramento, CA). This device consists of a horizon-
around the distal aspect of the thighs to encourage
tally moving carriage on which the patient can lie,
activation of the external hip rotator/abductor mus-
kneel, sit, or stand. Resistance is provided using
culature throughout the range of hip flexion/
springs, with fewer springs increasing the demand on
extension movement, and to provide proprioceptive
FIGURE 4. Weight-bearing exercises (weeks 6-10). (A) Isometric hip abduction performed in weight bearing against a wall. (B)
Upper-extremity activities performed in a single-leg stance. (C) Bilateral standing hip abduction performed on the Clinical Reformer. The
patient's right leg is on a platform that moves to the right against spring resistance as she concurrently pushes both legs apart against
resistance, while maintaining a stable pelvic position. (D) Holding Theraband and rotating the body medially while maintaining a static
lower extremity produces relative external rotation at the hip.
J Orthop Sports Phys Ther • Volume 33 • Number 11 • November 2003
input. The spring resistance to the leg press maneu-
ver was then gradually increased as symptoms andstrength gains dictated. When the patients couldconsistently demonstrate neutral lower-extremityalignment bilaterally throughout the semisquat activ-ity against the maximum spring resistance for 2 setsof 15 repetitions, they were progressed to a single-legsquat while maintaining the required neutral align-ment of the lower extremity (Figure 5B). When theprogression criterion was achieved, they then pro-gressed to the same motion in standing, first with adouble- and then a single-leg squat exercise. At this
time, patient A was able to perform a double- and
single-leg shallow squat to 40° symptom free, andpatient B was able to perform the double-leg shallowsquat to 40° symptom free, with mild discomfort (VASscore, 2/10) on the single-leg squat. Once the pa-tients were able to control a single-leg shallow squatin standing, they were given shallow lunging exercises(Figure 5C) from 0° to 45° knee flexion, usingTheraband, as described above, around the anteriorlunging thigh to promote activity of the hip abduc-tors and external rotators. Both patients also beganan aerobic conditioning exercise program using astair-climbing machine (ClimbMaster, Tetrix Fitness
Equipment, Irvine, CA) and were instructed to main-
tain the neutral lower-extremity alignment duringstair-climbing activities.
As the patients' pain resolved, interventions were
targeted at improving their functional limitations toachieve their stated goals. At week 8, when patient Awas able to perform a shallow unilateral squat symp-tom free, and had no pain on stair climbing, shecommenced a progressive independent running/walking program. At week 9, when patient B was ableto perform a single-leg stance activity demonstratingneutral lower-extremity alignment of the stance limbduring contralateral lower- and upper-extremity activi-ties, she was encouraged to return to her walkingprogram.
Both patients were re-evaluated at week 14, 3
months after the commencement of the treatmentprogram. Patient A had undergone 14 visits, whilepatient B had undergone 18 visits.
The postintervention functional assessment scores
increased from 76 to 85 and from 70 to 84 forpatients A and B, respectively.
FIGURE 5. Functional training (weeks 10-14). (A) Double-limb
squat performed on the Clinical Reformer. (B) Single-limb squat
Patient A reported no pain on walking or standing
performed on the Clinical Reformer. (C) Lunges using Theraband
during her 10-hour work shift and she no longer
around the affected leg were used to encourage external rotation
required her neoprene support. In addition, she was
and abduction of the hip throughout the range of motion.
J Orthop Sports Phys Ther • Volume 33 • Number 11 • November 2003
now able to ascend and descend stairs without pain,
had no feelings of weakness in her knee, and wasable to run 2 to 3 miles without discomfort. She
Postintervention kinematic analysis of the step-
occasionally experienced a tight feeling in the right
down maneuver was performed on patient A, as
knee during a full squat to reach into low cupboards
described earlier. When compared to pretreatment
at work, but this did not limit her activity.
values, improvements were noted in all motions
Patient B described a significant reduction in her
(Figure 6). Specifically, average hip internal rotation
pain level. She was now able to ascend and descend a
during stance improved from 1.4° of internal rotation
flight of stairs symptom free with occasional discom-
to 2.6° of external rotation; hip adduction was
fort (2/10) only if she had been on her feet for a
obser ved to decrease from 8.7° to 2.3°; and
considerable time. She could walk for 45 minutes and
contralateral pelvic drop was reduced from 3.9° to
could perform house-cleaning chores that involved
1.1° (Figure 2). These objective measurements were
squatting without difficulty or pain.
in agreement with the clinical observations notedearlier.
Patellofemoral Joint Examination
Re-evaluation of patient A's right patellofemoral
joint demonstrated a negative apprehension test, but
These case reports describe 2 patients with chief
mild pain with patellar compression. She demon-
complaints of PFP who responded favorably to a
strated pain-free isometric resisted knee extension in
strengthening program targeting the trunk, pelvis,
non-weight-bearing; however, some tightness was ex-
and hip musculature. Clinically relevant results were
perienced at 20° of flexion. Patient B still demon-
achieved without treatment strategies commonly em-
strated a mild positive patellar compression test with
ployed for the patellofemoral joint (ie, taping, vastus
slight pain elicited and mild medial retinacular ten-
medialis oblique strengthening, or stretching re-
derness, but no pain on isometric resisted knee
gimes). This suggests that the underlying cause of
extension at 20° to 0°. She had full pain-free passive
PFP in certain individuals may not be restricted tothe patellofemoral joint.
range of patella mobility.
Carson and James9,25 discussed the relevance of
considering lower-extremity kinetic chain factors
Muscle Strength Assessment
when evaluating and treating patients with a chiefcomplaint of knee pain. In addition, research by
Re-evaluation of muscle strength using the hand-
Beckman and Buchanan,1 Bullock-Saxton,8 and
held dynamometer revealed significant improvements
Jaramillo et al26 has demonstrated that weakness
in both patients (Table). Patient A demonstrated
proximal to the symptomatic area is often present
strength gains in all muscle groups, most notably the
with distal lower-extremity pathologies. This weakness,
ipsilateral lateral rotators of the hip (317%), gluteus
however, may be a precursor to the pathology or the
result of subsequent motor control changes.27 Never-
quadriceps (20%). Similarly, patient B demonstrated
theless, by addressing the identified weak proximal
strength gains in the gluteus maximus (110%),
musculature in the patients in these cases, improve-
gluteus medius (90%), the hip lateral rotator group
ments were noted in both subjective and objective
(15%), and quadriceps (10%).
It should be noted that during the exercise pro-
gram, patients were continuously encouraged to
monitor their performance of each motion. Suchtraining would facilitate motor learning of correct
Gait Based on observational assessment, both pa-
movement patterns, which may be distinct from
tients demonstrated improved gait kinematics at the
control of motion due to muscle strength alone.49 It
hip in the frontal and transverse planes. In general,
is, therefore, possible that the observed improve-
there was less hip adduction during weight accep-
ments in lower-extremity kinematics could have been
tance, and a decrease in both hip internal rotation
the result of a combination of muscle strength and
and contralateral pelvic drop during midstance.
improved motor control of motion.
Step-Down Task Both patients demonstrated signifi-
Both patients initially had a chief complaint of pain
cant improvements during the step-down maneuver.
during stair ascent/descent and prolonged walking,
Both had a reduction in adduction/internal rotation
and demonstrated poor control of the lumbopelvic/
of the stance limb, less knee valgus, and a smoother
hip region during these activities. McFadyen39 and
motion into hip flexion. Neither patient experienced
Soderberg56 concluded that the gluteus medius plays
pain during, or after, the step-down maneuver.
an important role in hip and pelvic stability during
J Orthop Sports Phys Ther • Volume 33 • Number 11 • November 2003
FIGURE 6. Computer-generated skeletal representation of patient A's lower-extremity kinematics. (A) Prior to intervention. (B) Postinterven-
tion. Reduced hip adduction and internal rotation of the hip can be observed in B.
stair descent, especially during the last 85% of the
that this difference was clinically meaningful. For
stance phase. In the preintervention test, patient A
example, hip adduction would move the patella
demonstrated excessive hip adduction during the last
medially with respect to the ASIS, thereby increasing
80% of stance phase, suggesting inadequate strength
the dynamic Q angle.45 Theoretically, any decrease in
of the gluteus medius. As can be seen by the
the hip adduction angle could result in a decrease in
postintervention data (Figure 2B), hip adduction was
the dynamic Q angle, thereby reducing the lateral
reduced, especially during the last 80% of the step-
force acting on the patella.45
down cycle, suggesting an improved control of this
The gluteus maximus muscle has been shown to be
a powerful external rotator of the hip,12 and the
Although the measured changes in hip adduction
function of its upper fibers have been found by Lyons
during the step-down maneuver were relatively small
et al34 to be similar to that of gluteus medius during
(6.4° averaged across the stance phase), we believe
gait and stair ascent. The substantial changes found
J Orthop Sports Phys Ther • Volume 33 • Number 11 • November 2003
in preintervention and postintervention muscle
2. Bizzini M, Childs JD, Piva SR, Delitto A. Systematic
strengths and kinematic data evaluating hip external
review of the quality of randomized controlled trials for
rotation (Figure 2A) indicate that the gluteus
patellofemoral pain syndrome. J Orthop Sports PhysTher. 2003;33:4-20.
maximus may play an important role in the control
3. Bohannon RW, Andrews AW. Interrater reliability of
of hip motion during gait and single-limb support
hand-held dynamometry. Phys Ther. 1987;67:931-933.
4. Bohannon RW. Intertester reliability of hand-held
The efficacy of quadriceps strengthening for PFP
dynamometry: a concise summary of published re-
has been described by several authors,11,29,30 and an
search. Percept Mot Skills. 1999;88:899-902.
argument could be made that in undertaking the
5. Bohannon RW. Reference values for extremity muscle
above exercise program, strength changes in the
strength obtained by hand-held dynamometry fromadults aged 20 to 79 years. Arch Phys Med Rehabil.
quadriceps group may have also contributed to the
decrease in symptoms. While this may be the case, it
6. Brody LT, Thein JM. Nonoperative treatment for patel-
should be noted that the strength gains in the
quadriceps were significantly less than in the other
muscle groups. Therefore, the resultant improvement
7. Buff HU, Jones LC, Hungerford DS. Experimental deter-
in the eccentric step-down activity and associated pain
mination of forces transmitted through the patello-
are unlikely to be solely due to changes in quadriceps
femoral joint. J Biomech. 1988;21:17-23.
8. Bullock-Saxton JE. Local sensation changes and altered
hip muscle function following severe ankle sprain. Phys
The patients studied in these 2 case reports were
Ther. 1994;74:17-28; discussion 28-31.
selected based on their clinical presentation of sus-
9. Carson WG, Jr., James SL, Larson RL, Singer KM,
pected proximal weakness, as suggested by observa-
Winternitz WW. Patellofemoral disorders: physical and
tional tests of gait and stair descent, and the lack of
radiographic evaluation. Part I: Physical examination.
Clin Orthop. 1984;165-177.
localized patellofemoral joint static positional faults
10. Clark MA. Core stabilization training in rehabilitation.
and dynamic tracking problems. As always, careful
In: Prentice WE, Voight ML, eds. Techniques in
selection of the appropriate patient for a particular
Musculoskeletal Rehabilitation. New York, NY:
intervention is important in achieving successful out-
comes. With this in mind, we feel that the described
11. Dehaven KE, Dolan WA, Mayer PJ. Chondromalacia
patellae in athletes. Clinical presentation and conserva-
treatment approach should be considered in the
tive management. Am J Sports Med. 1979;7:5-11.
management of patients with PFP who present with
12. Delp SL, Hess WE, Hungerford DS, Jones LC. Variation
similar clinical findings. This may be especially true
of rotation moment arms with hip flexion. J Biomech.
of those patients in whom a traditional course of
treatment has not produced satisfactory results.
13. Downie WW, Leatham PA, Rhind VM, Wright V,
Branco JA, Anderson JA. Studies with pain rating scales.
Ann Rheum Dis. 1978;37:378-381.
14. Fairbank HAT. Derangement of the knee in children and
adolescents. Proc Roy Soc Med. 1937;30:427-432.
These case reports present 2 patients with PFP who
15. Farrell JP, Koury M, Caroline DT. Therapeutic exercise
for back pain. In: Twomey LT, Taylor JR, eds. Physical
demonstrated abnormal kinematics at the hip and
Therapy of the Low Back. New York, NY: Churchill
who responded favorably to an exercise program
specifically targeting the hip, pelvis, and trunk muscu-
16. Franklin BA, Whaley MH, Howley ET. ACSM's Guide-
lature. Further research is indicated to better define
lines for Exercise Testing and Prescription. Philadelphia,
the relationship between proximal hip muscle weak-
PA: Lippincott Williams and Wilkins; 2000.
17. Fitzgerald GK, McClure PW. Reliability of measure-
ness and PFP, and to identify patients who will best
ments obtained with four tests for patellofemoral align-
respond to this treatment approach.
ment. Phys Ther. 1995;75:84-90; discussion 90-82.
18. Grelsamer RP, McConnell J. The Patella: A Team
Approach. Gathersburg, MD: Aspen Publishers; 1998.
19. Henry JH. Conservative treatment of patellofemoral
subluxation. Clin Sports Med. 1989;8:261-278.
The authors wish to thank Yu-Jen Chen, PT, MS,
20. Hodges PW, Richardson CA. Contraction of the ab-
for assisting in the collection and processing of the
dominal muscles associated with movement of the
kinematic data, and the staff at USC Physical Therapy
lower limb. Phys Ther. 1997;77:132-142; discussion142-134.
Associates, where these patients received their care.
21. Huberti HH, Hayes WC. Patellofemoral contact pres-
sures. The influence of q-angle and tendofemoral con-tact. J Bone Joint Surg Am. 1984;66:715-724.
22. Hvid I, Andersen LI. The quadriceps angle and its
relation to femoral torsion. Acta Orthop Scand.
1982;53:577-579.
1. Beckman SM, Buchanan TS. Ankle inversion injury and
23. Inman VT. Functional aspects of the abductor muscles
hypermobility: effect on hip and ankle muscle
of the hip. J Bone Joint Surg Am. 1947;53:577-579.
electromyography onset latency. Arch Phys Med
24. Insall J. Current Concepts Review: patellar pain. J Bone
Joint Surg Am. 1982;64:147-152.
J Orthop Sports Phys Ther • Volume 33 • Number 11 • November 2003
25. James SL, Bates BT, Osternig LR. Injuries to runners. Am
45. Powers CM. The influence of altered lower-extremity
J Sports Med. 1978;6:40-50.
kinematics on patellofemoral joint dysfunction: a theo-
26. Jaramillo J, Worrell TW, Ingersoll CD. Hip isometric
retical perspective. J Orthop Sports Phys Ther.
strength following knee surgery. J Orthop Sports Phys
46. Powers CM. Rehabilitation of patellofemoral joint disor-
27. Jenkins W, Bronner S, Mangine RE. Functional evalua-
ders: a critical review. J Orthop Sports Phys Ther.
tion and treatment of the lower extremity. In:
Brownstein B and Bronner S, eds. Functional Movement
47. Prentice WE. Impaired muscle performance: regaining
in Orthopaedic and Sports Physical Therapy: Evalua-
muscular strength and endurance. In: Prentice WE,
tion, Treatment, and Outcomes. New York, NY:
Voight ML, eds. Techniques in Musculoskeletal Reha-
Churchill Livingstone; 1997:191-229.
bilitation. New York, NY: McGraw-Hill; 2001:59-72.
28. Kannus P, Aho H, Jarvinen M, Niittymaki S. Computer-
ized recording of visits to an outpatient sports clinic.
48. Price DD, McGrath PA, Rafii A, Buckingham B. The
Am J Sports Med. 1987;15:79-85.
validation of visual analogue scales as ratio scale
29. Kannus P, Natri A, Paakkala T, Jarvinen M. An outcome
measures for chronic and experimental pain. Pain.
study of chronic patellofemoral pain syndrome. Seven-
year follow-up of patients in a randomized, controlled
49. Rose DJ. A Multilevel Approach to the Study of Motor
trial. J Bone Joint Surg Am. 1999;81:355-363.
Control and Learning. Boston, MA: Allyn and Bacon;
30. Kannus P, Niittymaki S. Which factors predict outcome
in the nonoperative treatment of patellofemoral pain
50. Sahrmann S. Diagnosis and Treatment of Movement
syndrome? A prospective follow-up study. Med Sci
Impairment Syndromes. St. Louis, MO: Mosby; 2002.
Sports Exerc. 1994;26:289-296.
51. Salsich GB, Brechter JH, Farwell D, Powers CM. The
31. Kendall FP, McCreary EK, Provance P. Muscles, Posture,
effects of patellar taping on knee kinetics, kinematics,
and Pain. Baltimore, MD: Williams and Wilkins; 1993.
and vastus lateralis muscle activity during stair ambula-
32. Kisner C, Colby LA. Therapeutic Exercise: Foundations
tion in individuals with patellofemoral pain. J Orthop
and Techniques. Philadelphia, PA: F. A. Davis; 1996.
Sports Phys Ther. 2002;32:3-10.
33. Kujala UM, Jaakkola LH, Koskinen SK, Taimela S,
52. Salsich GB, Brechter JH, Powers CM. Lower extremity
Hurme M, Nelimarkka O. Scoring of patellofemoral
kinetics during stair ambulation in patients with and
without patellofemoral pain. Clin Biomech (Bristol,
34. Lyons K, Perry J, Gronley JK, Barnes L, Antonelli D.
Timing and relative intensity of hip extensor and
53. Scott J, Huskisson EC. Graphic representation of pain.
abductor muscle action during level and stair ambula-
tion. An EMG study. Phys Ther. 1983;63:1597-1605.
35. Macausland WR, Sargent AF. Recurrent dislocation of
54. Scuderi GR. Surgical treatment for patellar instability.
the patella. Surg Gynecol Obstet. 1922;35:35-41.
Orthop Clin North Am. 1992;23:619-630.
36. Magee DJ. Orthopedic Physical Assessment. Philadel-
55. Siler B. The Pilates Body. New York, NY: Broadway;
phia, PA: W. B. Saunders; 1997.
37. Maquet PGJ. Biomechanics of the Knee: With Applica-
56. Soderberg GL, Dostal WF. Electromyographic study of
tion to the Pathogenesis and the Surgical Treatment of
three parts of the gluteus medius muscle during func-
Osteoarthritis. New York, NY: Springer-Verlag; 1984.
tional activities. Phys Ther. 1978;58:691-696.
38. McConnell J. Patellofemoral joint complications and
57. Steinkamp LA, Dillingham MF, Markel MD, Hill JA,
considerations. In: Ellenbecker TS, ed. Knee Ligament
Kaufman KR. Biomechanical considerations in patel-
Rehabilitation. New York, NY: Churchill Livingstone;
lofemoral joint rehabilitation. Am J Sports Med.
39. McFadyen BJ, Winter DA. An integrated biomechanical
58. Taylor JR, O'Sullivan P. Lumbar segmental instability:
analysis of normal stair ascent and descent. J Biomech.
pathology, diagnosis, and conservative management. In:
Physical Therapy of the Low Back. New York, NY:
40. Messier SP, Davis SE, Curl WW, Lowery RB, Pack RJ.
Churchill Livingstone; 2000:201-247.
Etiologic factors associated with patellofemoral pain in
59. Thomee R, Augustsson J, Karlsson J. Patellofemoral pain
runners. Med Sci Sports Exerc. 1991;23:1008-1015.
syndrome: a review of current issues. Sports Med.
41. Nadler SF, Malanga GA, Bartoli LA, Feinberg JH,
Prybicien M, Deprince M. Hip muscle imbalance and
60. Ward SR, Powers CM, Fredericson M, Guillet M,
low back pain in athletes: influence of core strengthen-
Shellock FG. The influence of medial femoral rotation
ing. Med Sci Sports Exerc. 2002;34:9-16.
42. Neumann DA, Cook TM. Effect of load and carrying
on lateral patellar tilt during weight bearing and non
position on the electromyographic activity of the
weight bearing movements. Med Sci Sports Exerc.
gluteus medius muscle during walking. Phys Ther.
61. Wilk KE, Davies GJ, Mangine RE, Malone TR. Patel-
43. Neumann DA, Soderberg GL, Cook TM. Comparison of
lofemoral disorders: a classification system and clinical
maximal isometric hip abductor muscle torques be-
guidelines for nonoperative rehabilitation. J Orthop
tween hip sides. Phys Ther. 1988;68:496-502.
Sports Phys Ther. 1998;28:307-322.
44. Philadelphia Panel evidence-based clinical practice
62. Winstein CJ. Knowledge of results and motor learning—
guidelines on selected rehabilitation interventions for
knee pain. Phys Ther. 2001;81:1675-1700.
J Orthop Sports Phys Ther • Volume 33 • Number 11 • November 2003
Functional assessment tool for patellofemoral joint
disorders (from Kujala et al,33 with permission from
(a) No difficulty (10)
the Arthroscopy Association of North America).
(b) Slight difficulty (7)(c) Constant pain (2)
Kujala Questionnaire for Patellofemoral Joint Pain
8. Prolonged sitting with the knees flexed
(a) No difficulty (10)
(b) Pain after exercise (8)
(c) Constant pain (6)
Duration of symptoms:
(d) Pain forces to extend knees temporarily (4)
For each question, circle the latest choice (letter)
which corresponds to your knee symptoms.
(b) Slight and occasional (8)
(b) Slight or periodical (3)
(c) Interferes with sleep (6)
(d) Occasionally severe (3)
(e) Constant and severe (0)
(a) Full support without pain (5)
(c) Weight bearing impossible (0)
(b) After severe exertion (8)
(c) After daily activities (6)
(a) Unlimited (5)
(d) Every evening (4)
(b) More than 2 km (3)
11. Abnormal painful kneecap (patellar) movements
(a) No difficulty (10)
(b) Occasionally in sports activities (6)
(b) Slight pain when descending (8)
(c) Occasionally in daily activities (4)
(c) Pain both when descending and
(d) At least 1 documented dislocation (2)
(e) More than 2 dislocations (0)
12. Atrophy of thigh
(a) No difficulty (5)
(b) Repeated squatting painful (4)
(c) Painful each time (3)
13. Flexion deficiency
(d) Possible with partial weight bearing (2)(e) Unable (0)
(a) No difficulty (10)
(b) Pain after more than 2 km (8)(c) Slight pain from start (6)(d) Severe pain (3)(e) Unable (0)
J Orthop Sports Phys Ther • Volume 33 • Number 11 • November 2003
Source: http://www.physioinfo.co.za/UserFiles/Case%20study.pdf
Angol.cdr
Róbert Torontáli: Intensive Krav-Maga I. Zsuzsa Fritz: Hevruta Tradition Community November 07. Friday, 17:00 - 18:30 November 08. Saturday, 11:30 - 12:45 Robert Torontáli, technical director of Intensive Krav-Maga Europe is running a very useful Experience the ancient method of text study. In pairs or in small groups juxtapose texts from the
Microsoft word - adrenal insufficiency and addison
Adrenal Insufficiency and Addison's Disease What is adrenal insufficiency? Adrenal insufficiency is an endocrine—or hormonal—disorder that occurs when the adrenal glands do not produce enough of certain hormones. The adrenal glands are located just above the kidneys. Adrenal insufficiency can be primary or secondary. Primary adrenal insufficiency, also called Addison's disease, occurs when the adrenal glands are damaged and cannot produce enough of the hormone cortisol and often the hormone aldosterone. Addison's disease affects one to four of every 100,000 people, in all age groups and both sexes.1