Nefhs 2014-hurley-feline uri






Kate F. Hurley, DVM, MPVMKoret Shelter Medicine Program DirectorCenter for Companion Animal HealthUniversity of California, Daviswww.sheltermedicine.comwww.facebook.com/sheltermedicine
7/162 (4%)
31/60 (52%)
Pedersen, N. C., R. Sato, et al. (2004). "Common virus infections in cats,
before and after being placed in shelters, with emphasis on feline enteric
coronavirus." J Feline Med Surg 6(2): 83-88.
Drazenovich, T. L., A. J. Fascetti, et al. (2009). "Effects of dietary lysine supplementation on upper respiratory and ocular disease and detection of infectious organisms in cats within an animal shelter." Am J Vet Res 70(11): 1391-1400.
Mycoplasma C. felis
Herpes Bordetella
Veir, J. K., R. Ruch-Gallie, et al. (2008). "Prevalence of selected infectious organisms and
comparison of two anatomic sampling sites in shelter cats with upper respiratory tract disease." J
Feline Med Surg 10(6): 551-557.
Spindel, M. E., J. K. Veir, et al. (2008). "Evaluation of pradofloxacin for the treatment of feline
rhinitis." J Feline Med Surg 10(5): 472-479.
Bannasch, M. J. and J. E. Foley (2005). "Epidemiologic evaluation of multiple
respiratory pathogens in cats in animal shelters." J Feline Med Surg 7(2):
109-119.
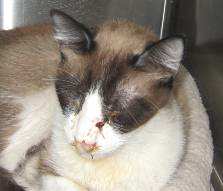
• Herpesvirus causes
vast majority of "endemic" shelter URI
• Calicivirus and
Bordetella are sporadic problems in shelters, may be more commonly associated with pet cat and sanctuary URI
• Chlamydia is rare but
problematic when it occurs
• Mycoplasma is common
and important secondary player
Carrier state common
Carrier state common
Stress associated
Not stress associated
Rarely vaccine resistant
Often vaccine resistant
• STRESS• Pregnancy/birthing• Moving from cage to
• Housing change
induced shedding in 18 - 83%
• Introduction of new
cats – especially intact
• Infection activated in
cats negative after 2
Gaskell, R. M. and R. C. Povey (1977). Vet Rec 100(7): 128-133.
steroid treatments
Maggs, D. J., M. P. Nasisse, et al. (2003). Am J Vet Res 64(1): 37-42.
Hickman, M. A., G. H. Reubel, et al. (1994). Lab Anim 28(4): 320-329.
• Shedding intermittent
regardless of stress
• Tends to reduce with
age and lose virulence over time
transmissibility and vaccine resistance all sort independently and are quasi-stable
• Virulent strains are
• Evaluate risk posed by individual based on
disease manifestations in group:
• Severity of worst disease• Health, age and vaccine status of affected individuals• Presence or absence of co-factors• Apparent ease of spread
• Risk likely reduces over time and with full
resolution of signs
• Highest risk if healthy adults from clean
environment are affected
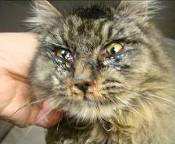
• Swelling, widespread hair
loss, crusting and ulceration
• Especially face, ears, feet
• Up to 40-60% mortality
• Some mild or subclinical
• "Peracute hepatocellular
• Variable other organ
involvement (pancreas, lung, spleen, lymph nodes, colon)
History of infectious disease exposure or spread"Typical" FCV signs precede VS-FCV signs (URI, ulcers, limping)Edema, skin involvement, hepatocellular individualization, death – other causes ruled outViral isolation from serum or tissue vs. oralcDNA sequencing of identical strain from > 1 catImmunohistochemistry on biopsy or necropsyRemember calicivirus infection does not preclude other diseases: always check for
Bannasch, M. J. and J. E. Foley (2005). "Epidemiologic evaluation of multiple respiratory pathogens in cats in animal shelters." J Feline Med Surg 7(2): 109-119.
Quaternary ammonium
Necrotizing streptococcus canis
• Unusually severe or
frequent disease in population
• Suspected Chlamydia or
rule out others in individual
• At least 5-10 acutely
• Most affected location or
per laboratory instructions
• Quantitative RT-PCR may
help distinguish important versus vaccine/carrier state
• Gram negative and gram
• Pasteurella species, E coli,
Streptococcus, Enterobacter and Staphylococcus species
• Mycoplasma very common
• Chlamydophila and
Bordetella sporadically important
• Intracellular
• Revisit stress management,
crowd control, air quality as first defense
Gram negative spectrum recommended
Schulz, B. S., G. Wolf, et al. (2006). "Bacteriological and antibiotic sensitivity test results
in 271 cats with respiratory tract infections." Vet Rec 158(8): 269-70.
1. Clavamox vs. Marbofloxaxin: no significant difference in 103
improvement or cure in 77% vs.87% on day 5
2. Amoxicillin BID vs. azythromycin Q72 hrs: no significant
difference in 31 cats
• 38% and 40% cure at 9 days, 50% more after switch for both groups
• 8/31 did not resolve after both rounds of treatment
3. Amoxicillin BID vs. pradofloxacin (5 or 10 mgs/kg) SID: no
significant difference in 43 cats (same shelter, different time)
• 67%, 77% and 92% respectively
• 9 remaining cats cured after switch
• Antibiotics only when
clearly indicated
• Including if always indicated• Not including if not always
• Consistent 1, 2 plan
based on categories of signs/severity
• Mycoplasma/Chlamydia/
Bordetella vs secondary
• Evaluate early and often
in shelter, treat to either cure or failure rather than time
• Practical considerations:
• Cost, route, frequency, side
• Less ideal given correctly is
better than ideal given wrong
• Above all, do no harm
• One cat, one set of drugs• Doxy or minocycline :
• Liquid or flush, milk products ok,
citric acid can cause toxic byproducts
• 10 mgs/kg/day with food (50
mgs/adult cat ok)
• Doxy 7 days max after mixing,
DOXYCYCLINE POTENCY AFTER STORAGE IN A COMPOUNDED FORMULATION FOR ANIMALS. Mark G. Papich, Daria DiGiovanni, and Gigi Davidson, North Carolina State University, College of Veterinary Medicine, R m
• Consider topical if no
other respiratory involvement
• Tetracycline,
• Betadine 1:30 in saline
• Caution with steroids
• One tube per cat
• Topical may not be
necessary if treating systemically
• Suspicious clinical signs• Responds to doxy or
minocycline, clavamox, fluorquinolone, azithromycin, topical tetracycline within 7 days
• Signs recur within 14-30
• Responds again to doxy or
• Continue 4 weeks minimum• Put up for adoption on
Remember Chlamydia is uncommon:
treatment once signs resolve
consider PCR before second round of
• Good foster to adopt
• Multiple cats and
observers means written record extra important
• Daily observation of
• Food intake, hydration,
demeanor, urine/feces
• +/- temperature
• Written dose, duration,
• Initials of person giving
• Delicious, stinky food
• Caution with food aversion
• Mirtazipine if not eating within 2-3
• Force feed if not eating after 5-7 days
• Calculate kcal; force feed 50%
• Dehydration chart
• Comfort and care• Pain control
• Especially if ulcers• Make sure hydration is adequate
Appetite stimulants
Nose drops EONostril/EOD
Try saline drops first
• Private Room: 3 times less likely to catch the flu and 1.3 more hours
• Carpeting: 29% fewer injuries from falls and visitors stayed 8
• A View of Nature: View of trees versus brick wall led to fewer pain
meds and an average of .74 fewer days at the hospital
• Sound-Absorbing Ceiling Tiles: More restful sleep, and a lower rate
• Light-Filled Window: Patients who recovered in sunny rooms took
22 percent less pain medication per hour than patients in dim rooms.
In cardiac ICUs, 61% higher death rate in facilities without natural
• Natural light, good air quality,
big comfy cages, hiding spots or half-cage-covers, minimal noise
• No dogs allowed!
• Dedicated equipment,
protective tops, gloves or hand wash before and after handling cats (in shelter with routine URI)
• Forget about footbaths
• Shoe covers if something truly
• Play/lap-sitting area ok for
• Ideally off to the side• Do not use for suspect calici• Shut down if unusually severe
• Housing allows for
easy spot cleaning
• Staff/volunteers can
comply with cleaning last, no out-of-cage time, change of top and wash of hands after care
• Mark cage clearly• Mildly ill only
• Antibiotics = isolation
• Run of the mill suspect
herpes, chronic URI unlikely risk to pet cats
• Adults lower risk than
kittens to pets in home
• Revaccinate pet cats
annually for FVRC (IN) and/or consider two way calicivax
• NOT for suspect severe
• Isolation/treatment
• Flow through issue from
isolation to adoption?
• Unusual pathogen?
• Stress, poor immune function
• Chlamydia, polyp, fungal,
deep bacterial plus structural compromise?
• Lymphoplasmacytic rhinitis,
neoplasia, dental issues, foreign body?
• Lulu – 10mo F/S DSH
presented for chronic URI
• Treated by the shelter
with multiple rounds of antibiotics:
• Clavamox• Doxycycline• Clavamox• Clindamycin• Baytril• Azithromycin
• Deep nasal swab C&S:
multi-drug resistant Pseudomonas aeruginosa
• Earlier treatment has better
• Initiate after two rounds of
appropriate (different) antibiotic tx
• Chlamydophila• Gram negative
• Careful physical exam
• Nasal versus ocular versus
• Unilateral versus bilateral
• Retrovirus testing• Diagnostics
• PCR?• Polyp check
• Antibiotics with good
• Doxy, clindamycin,
clavamox, azithromycin
• If antibiotic response in first
week, continue 6-12 WEEKS
• The longer it's been, the longer
• Outdoor access• Foster or adopt: unlikely
• Do not keep in limbo in
How do we prevent this?
• Herpesvirus causes
vast majority of "endemic" shelter URI
• Calicivirus and
Bordetella are sporadic problems in shelters and may be more commonly associated with pet cat and sanctuary URI
• Chlamydia is rare but
problematic when it occurs
• Mycoplasma is common
and important secondary player
• Improper disinfection?
• Lousy air quality?
• No place to hide?
• Too many pokey little
fingers in the cage, or not enough socialization?
• Does not prevent infection or
• Requires 2 doses in some
naïve cats to provide protection
• Exposure may not be
immediate for calici
• Resistant strains of calici
• Consider two strain calici
vaccine for sanctuary/long term cats and high risk pet cats, especially foster care providers
• IN: theoretically faster,
younger, local protection
• Possible non-specific
• More possible signs
• But not in shelter1?
• MLV parenteral PANLEUK
• BOTH IN and SC?
If they MUST stay here, IN FVRC at 2-4
• No3• Yes during outbreak of
unknown disease?4
1. Edinboro, C. H., L. K. Janowitz, et al. (1999). Feline Practice 27(6):
2. Newbury, S. P., L. Larson, et al. (2007). Conference of Research
Workers in Animal Diseases, Proceedings of the 88th Annual Meeting, Chicago.
3. Environmental and group health risk factors for feline URI,
unpublished data, 2011
4. Bradley, A., J. Kinyon, et al. (2012). "Efficacy of Intranasal
Administration of a Modified Live Feline Herpesvirus 1 and Feline Calicivirus Vaccine against Disease Caused by Bordetella bronchiseptica after Experimental Challenge." J Vet Intern Med.
• SC MLV FVRCP for all >
4-6 weeks on entry + 2-3 week booster
• Revaccinate kittens SC
every 2 weeks while in high risk environment, every 3-4 when not
• Final vaccine at 20 weeks in
whatever environment
• Vaccinate pregnant cats
unless legal case
• If outbreak confirmed by
laboratory diagnostics
• Revisit need after
outbreak resolved
• Revisit husbandry in
addition to adding vaccination
• Chlamydia requires
booster; choose MLV or antigen extract; caution with adverse effects
• E.g. kitten or cat foster
providers, shelter or veterinary staff/volunteers, long stay shelter/sanctuary/clinic resident felines
• 2 way calici vaccine?• Revaccinate annually for
FVRC especially after hiatus from exposure?
• Chlamydia and
Bordetella prior to kitten
• 37/58 cats lost average
6 % body weight in 7 days
• Weight loss in week 1
correlated with URI in days 4-14
• 15/24 remaining another 7
days also lost weight
• Weight loss significantly
correlated with stress score
• Weight may be a sensitive
and easily measured indicator of stress and URI risk
• Offer palatable, highly
absorbable, consistent diet
• Have variety on hand for
• Separate food and litter
by at least three feet
• Dim lights and/or cover
• Avoid pairing feeding
with aversive activities
• Smells, sounds, disruption
conducted in animal shelters showed no benefit of lysine supplementation for preventing URI (1,2)
• Two studies have
documented more severe URI in supplemented cats (2,3)
Drazenovich, TL, Fascetti AJ, Westermeyer HD, Sykes JE, Bannasch MJ, Kass, PH, Hurley, KF, Maggs, DJ. "Effects of dietary lysine supplementation on upper respiratory disease and infectious organism shedding in cats within an animal shelter." American Journal of Veterinary Research, Submitted 10/12/08. Manuscript ID AJVR-08-10-0330
Rees, T. M. and J. L. Lubinski (2008). "Oral supplementation with l-lysine did not prevent upper respiratory infection in a shelter population of cats." J Feline Med Surg.
Maggs, D. J., J. E. Sykes, et al. (2006). "Effects of dietary lysine supplementation in cats with enzootic upper respiratory disease." J Feline Med Surg.
• Bleach and its ilk, potassium
peroxymonosulfate (Trifectant, Virkon), accelerated hydrogen peroxide (Accel)
• Stress, fomite
transmission and respiratory irritation can cause more harm than good
• Better disinfectants and
ringworm screening skills allow use of quieter, warmer, cheaper, more flexible materials
• Spot clean where-ever
possible for cats in situ
• Change gloves between cats• Confine cat to one side, hold
gently with gloved hand, or place in carrier within cage
• Tidy cage, replace food,
water, and litter, replace dishes and litter pan if needed
• Use water, detergent, paper
towel or single use rag to wipe visible debris
• Leave bedding unless heavily
• Ok for healthy cats and
Weiss, E., K. Miller, et al. (2012). "Why Did You Choose This Pet?: Adopters and
Pet Selection Preferences in Five Animal Shelters in the United States." Animals
2(2): 144-159.
Droplet spread possible up to five feetAt least 1.5 open sides if possible
More important the smaller the cage
Minimize irritants
Spot clean, no spray
Use fans after cleaningOpen doors and windowsUtilize outdoor space whenever possibleDon't hang your hopes on air filters
• Shelf may be preferable to
box if floor space is limited
• Box maybe preferable to
shelf is height is limited but floor space adequate
• Partial front cover and
towel in cage may be best choice if both floor space and height are limited
• Tailor to individual cat in
small small cages
• Away from cage fronts by
• Visual barriers/hiding
• Ideally, walk-in for people• Consider health and
• Adult cats vaccinated at least
• Routine URI within ward OK• Discontinue during outbreaks
• Make sure staff/volunteer
time and skill is adequate
• I work at a non-profit, open admissions shelter. In the past,
the summer months have brought us rampant URI in cats, and our live release rates have been less than ideal (2010 was 54% for the month of July). We have an amazing new building that opened in 2009, and has 126 Shorline cages for cat holding (in addition to the adoption floor, which has two "kitty cities" for group housing and 16 cat "condos" that are basically tiny rooms instead of cages).
In 2010 we adjusted the temperatures in the cat lofts higher so the kitties wouldn't be as cold, we added hiding boxes and Kuranda beds, but we didn't see any changes in the URI rates. Cats were being euthanized daily because the URI was so widespread, and the severity of the illnesses were much greater than you see in private practice URI. Cats would go to foster for URI and be there for MONTHS with sneezing or conjunctivitis.
49 questions including cage size, material and number, hiding place, handling, infectious disease control, vaccination, feeding, timing of S/N, air quality, natural light, dog exposure
Drum roll please…
Greater than 9 square feet of floor space but not 6-8
compared to < 6
Limited movement in first 7 days
All large cages were compartmentalized
50 fold variation between shelters on per day basis
8 fold variation as percentage of intake
50, 531 total sick cat days
13% of care days overall, range < 1% to 30%
• In February 2011, we took a huge step and cut holes in
between cat holding cages, and inserted PVC portholes, effectively doubling the space available to each cat and cutting the number of cages we had in half. Actually less than half -because each loft had an odd number of cages, there is a set of triple cages in each loft. We've now got 60 separate cat holding cages. These portholes were designed to be permanent openings, we did not make any "doors" to close because then it's too tempting to revert to less space and more cats. We had many staff and volunteers who were very leary of the change, fearing that more cats would be euthanized because we lacked space.
• We saw some effects right away. The lofts were
immediately quieter, cats seeming more relaxed. There were very few cats "fake sleeping". The longer term effects are just starting to show up. Cat isolation is empty today, because our URI rates have plummeted. Cats aren't breaking with URI right before or after adoption. And now that the statistics for July are in, we found that our live release rate for felines in July 2011 was 70%. In 2010 it was 54%. We euthanized 140 fewer felines in July 2011 compared to July 2010 - and those numbers include the cats we euthanize on intake for lack of space.
• We still have to remind ourselves occasionally that we
don't have enough homes to save every cat we otherwise could right now. But making the euthanasia decision earlier on is saving a lot of staff time and stress, and in the long run we've got healthier cats to adopt. Healthier cats will make a difference in the reputation we have, and pave the road to even higher adoption numbers.
"Sometimes we just have to laugh because it almost seems impossible that one program can impact the numbers so significantly. This was one of those areas of the operation that we didn't even know would improve until after we started the program and realized what a positive impact it was having on the incidence of UR
Research on "Environmental Risk Factors for Feline URI" and "Comparison of Two Cage Types: Effect on Shelter Cat Stress, Upper Respiratory Disease and Adoption" was funded by Morris Animal Foundation— the world's largest nonprofit that supports animal health studies to protect, treat and cure animals.
Morris Animal Foundation funds research at veterinary colleges around the world. Its funding facilitates medical breakthroughs that help animals enjoy longer, healthier lives and trains the next generation of veterinary scientists.
Source: http://www.newenglandfed.org/pdf/2014%20PPT/NEFHS%202014-Hurley-Feline%20URI.pdf
Microsoft word - 42559bba-2966-08ff29.doc
ARCHIVED - Archiving Content ARCHIVÉE - Contenu archivé Archived Content Contenu archivé Information identified as archived is provided for L'information dont il est indiqué qu'elle est archivée reference, research or recordkeeping purposes. It est fournie à des fins de référence, de recherche is not subject to the Government of Canada Web
Facharbeit
Facharbeit über eine Fallstudie im Rahmen des Zertifizierungsverfahrens Verband deutscher Tierheilpraktiker (VDT) Name, Vorname: Voigt, Annette Adresse: Am Mühlenhof 5, 49201 Dissen a.T.W. Matrikelnummer: 1251516 Zertifizierungsnr.: 5657 Inhaltsverzeichnis I. Fallstudie der Facharbeit Tierheilpraktiker / Pferd