Novatretin.com
TOTAL SUPPORT KIT Acitretin 10 mg and 25 mg Capsules It Is Important to read and understand thIs InformatIon Your DailY Dose of NovatretiN is:Number of Capsules per day:
x 10 mg Caps / Day
x 25 mg Caps / Day
If you ever need to check what your dose is you can refer to the above information.
Novatretin is a prescription medicine.
seCtIon 01
seCtIon 02
usInG noVatretIn seCtIon 03
seCtIon 04
seCtIon 05
CarInG for Your sKIn seCtIon 06
heLpInG Your psorIasIs seCtIon 07
treatInG darIer's dIsease seCtIon 08
manaGInG IChthYosIs seCtIon 09
manaGInG paLmo-pLantar dIsorders seCtIon 10
Consumer medICIne InformatIon seCtIon 01
Who NeeDs NovatretiN?
novatretin is used to treat severe psoriasis and a number of other conditions where the growth of skin cells needs to be normalized.
What is NovatretiN ?
novatretin capsules contain a medication known as acitretin. It is a similar substance to Vitamin a, but the action of acitretin is very different. novatretin works by normalizing skin cell growth.
While you are taking novatretin you will need to follow very carefully all the instructions given to you by your doctor. You should also follow the advice given to you in this booklet, as it will help you to look after your skin during your novatretin treatment and may give you some information on other ways you can help managed your condition. hoW loNg Will i Be takiNg NovatretiN?
the course of novatretin treatment will vary from patient to patient. Your doctor will advise you how long to take your novatretin. In most cases the treatment takes 6 weeks before an improvement will be noticed. treatment could last for several months and sometimes needs to be continued for a year or more. novatretin is often used together with other products or with uVa or uVB ultraviolet light. You should follow your doctor's instructions carefully.
the healing process that is started with novatretin may continue after the treatment has ceased. You will need to keep taking your novatretin for as long as your doctor has told you to. If you stop sooner you may not get the full benefits of novatretin. If your condition has not been cleared, a longer course of novatretin may be considered by your doctor.
are there aNY siDe effeCts?
as with all medicines, there are side effects with novatretin. the side effects include dryness in several parts of the body, possible tiredness, and sometimes aching of the muscles and bones. more information on side effects can be found in the side effects section of this booklet.
NovatretiN aND PoteNtial Birth DefeCts
novatretin should neVer be used by pregnant women or by women who intend to become pregnant, during or for two years after, their novatretin treatment.
all possibility of pregnancy must be ruled out before you start your novatretin treatment. strict birth control methods should be used for at least one month before you start your novatretin, during your whole novatretin treatment and for two years after you stop taking novatretin. two years after you have finished your novatretin, you can resume your normal practices.
further information about novatretin and birth defects can be found in the Contraception section of this booklet. there is no known risk to males who wish to father children.
Who CaN't take NovatretiN?
people who can't take novatretin include pregnant women or women who are breast feeding and people suffering from certain medical conditions such as impaired liver or kidney function. please tell your doctor if you have any other conditions or take any other medications.
sometimes you may be asked to have blood tests done. these establish a baseline for your liver function, blood lipids, and for females can also confirm that you are not pregnant. follow your doctor's advice before having blood taken.
seCtIon 02
hoW Do i use NovatretiN ?
It is very important to follow the instructions given to you by your doctor. these instructions will help to make sure you are getting the right dose of novatretin. In determining the exact dosage you need, your doctor will have considered the severity of your condition, your weight, and other factors.
It is important not to miss any of your novatretin capsules, or to take too many novatretin capsules. If you do miss a dose you should not take a double dose to make up for it, you should wait until it is time for your next dose and take your novatretin as normal, then continue taking your novatretin in the usual way.
Your doctor has prescribed a particular dose of novatretin for you for a specific reason. It is important that you do not change the amount of novatretin you are taking, if you think it is too strong or too weak speak to your doctor. Your doctor may vary your dose of novatretin, depending on how your body responds to the treatment. You should continue taking your novatretin for as long as your doctor instructs you to.
What Must i Do While takiNg NovatretiN?
While taking novatretin you must: take your novatretin capsules with meals to help absorption.
not chew or suck the capsules.
swallow the capsules whole with water or another non-alcoholic drink.
take each dose of novatretin when it is due.
follow your doctor's instructions.
If you follow the above instructions as closely as possible your novatretin will work better.
What shoulD i exPeCt froM NovatretiN?
When you first start taking novatretin you may find that your condition starts to get worse. If you have any worries or concerns about this, contact your doctor. this does not mean that the medication is not working. If this happens to you, do not be discouraged; keep taking your novatretin, as prescribed by your doctor. the worsening of your condition nearly always stops within the first few weeks, and then your condition will start to clear. Within the first four weeks of starting novatretin you may notice that your skin is much drier than before. You may also find that you need to wash your hair less often. most improvement in your condition will occur in the first 3 months of treatment and is maintained while treatment continues.
WheN i have fiNisheD MY NovatretiN
If you have any novatretin capsules left when you have finished your treatment, it is very important that you return them to your doctor or pharmacist.
never give your novatretin to anyone else, even if they have similar looking condition.
at the conclusion of your novatretin treatment your condition may continue clearing, possibly for one or two months, but it may also or later recur or worsen after the novatretin treatment has ceased. Your doctor may recommend taking novatretin again. the side effects associated with novatretin treatment will begin to clear at the conclusion of the treatment.
acitretin is an oral retinoid (vitamin-a derivative) used to treat severe psoriasis, usually at a dose of between 25 and 50 mg per day. It is best taken after a meal because fat helps it to be absorbed through the gut wall. acitretin is particularly effective for pustular psoriasis, erythrodermic psoriasis and psoriasis affecting hands and feet. It is not effective for psoriatic arthritis. It is occasionally used to treat other skin conditions including: palmoplantar pustulosis hand dermatitis (when very thick and scaly) Lupus erythematosus Cutaneous t-cell lymphoma extensive granuloma annulare severe ichthyosis extensive solar keratoses and skin cancers acitretin must not be taken in pregnancy; it can damage an unborn child and cause birth defects. strict birth control measures must be used during treatment and for two years after stopping acitretin. therefore, acitretin is rarely prescribed to females of child-bearing potential. If it is, they will be asked to have a blood pregnancy test before treatment and regularly during treatment. people on acitretin should not donate blood during treatment or for two years afterwards. also, acitretin should not be taken while breast-feeding. It has no effect on male sexual function or offspring. MeChaNisM of aCtioN
acitretin is thought to work in psoriasis by slowing down the proliferation of skin cells. a response is noted in more than half of treated patients. Improvement begins about two weeks after starting treatment, and is maximum after about twelve weeks. the affected skin either peels off or gradually clears. some patients are treated for a few months, repeated from time to time, whilst others remain on the acitretin long term. It is not known how it works in other skin disorders, but it may relate to some effect on immune cells. In resistant cases, acitretin can be combined with other anti-psoriatic drugs and/or phototherapy. siDe effeCts
acitretin has side effects that may limit the dose that can be used. dryness of lips: apply lip salve frequently especially when outdoors. dry nostrils that may crust and/or bleed: petroleum jelly can help. dry eyes: use artificial tear eye drops. dry reddened skin: apply moisturizers frequently. peeling skin, especially hands and feet; apply moisturisers frequently. fragile soft skin: protect it from injury, especially where skin can rub.
Increased susceptibility to sunburn: protect your skin from the sun. use broad spectrum sunscreen and cover up well. If you are receiving phototherapy, advise your therapist that you are taking acitretin. a reduction in dose may be necessary. skin infections, especially with staphylococcus aureus (impetigo, boils or nail fold paronychia). aggravation of your skin complaint: this is often temporary and followed by improvement but if a severe flare occurs you should tell your dermatologist and stop taking the acitretin. headaches: if these are severe or accompanied by visual problems, inform your dermatologist and stop the acitretin; the symptoms could be caused by an increase in pressure on the brain. muscle, joint or bone aches, especially with exercise; reduce exercise if needed. Generalised hair shedding and thinning may occur; this is usually temporary although permanent thinning has been reported. hyperlipidaemia (raised blood fats i.e. cholesterol and triglyceride), detected by blood tests, which are best taken when fasting (on an empty stomach). the level of the blood fats is compared with a pre-treatment test. high blood fats are more likely in diabetics and in those who drink a lot of alcohol. If the blood fats are too high, a special low fat and low sugar diet may be recommended, a lipid-lowering medication may be prescribed or the dose of acitretin may be reduced or stopped. rarely, acitretin may result in disturbed liver function (hepatitis). It should be discontinued if this occurs, and it would be unwise to take it again. mood changes; high dose retinoids can cause mood change including irritability, aggression and depression. acitretin should not normally be taken at the same time as the following medications (there may be rare exceptions): Vitamin a or any other retinoid (e.g. isotretinoin). tetracycline or one of its derivatives. It is best to avoid alcohol, during treatment and for two months after treatment with novatretin is completed. seCtIon 03
VerY Important!If you are female it is extremely important that you read and understand the information in this section.
WhY Must i PreveNt PregNaNCY?
even if you are not sexually active it is important that you understand the effects that novatretin can have on the unborn child should you become pregnant while taking novatretin. the medication in novatretin, acitretin, is teratogenic. this means that it can cause birth defects, that is, the unborn child can become deformed.
Birth defects can only be caused by novatretin if you use novatretin while you are pregnant, become pregnant while you are using novatretin or become pregnant within two years of stopping taking your novatretin.
Your doctor may give you a pregnancy test to ensure that you are not pregnant before allowing you to start taking novatretin. should you become pregnant while taking novatretin or within two years after the end of your novatretin treatment you will need to discuss the action that may need to be taken with your doctor. this is a very serious situation. for this reason it is vitally important to follow strict birth control procedures.
Who NeeDs to Be reallY Careful?
aLL women of child bearing potential! this means any woman who is taking novatretin, who is menstruating needs to follow a strict birth control procedure.
Before you can begin taking novatretin you may be required to take a pregnancy test.
You must use strict birth control for at least one month before you start your novatretin treatment, during the entire novatretin treatment and for at least two years after you stop taking novatretin.
You should wait until the 2nd or 3rd day of your next menstrual period before you start taking novatretin. this is an extra check to make sure you are not pregnant.
If you do become pregnant while you are taking novatretin, you should immediately stop taking your novatretin and tell your doctor straight away. novatretin does not affect your fertility in the long term. so even after taking novatretin you should be able to become pregnant in the future.
Who is resPoNsiBle for MakiNg sure i DoN't get PregNaNt ?
You are! the only person who can make sure that you do not get pregnant while you are taking novatretin is you. It is relatively easy to prevent pregnancy. the details of the recommended strict birth control procedure are explained below.
Before you begin taking novatretin your doctor will go through the risks associated with novatretin and pregnancy. Your doctor may ask you to sign a Consent form. signing this form means that you understand these risks and that you will do everything possible to make sure that you do not become pregnant while you are taking novatretin or for two years after you stop taking novatretin.
What is striCt Birth CoNtrol?
strict birth control or contraception means carefully following a regimen to make sure you do not become pregnant. the most effective form of birth control or contraception is ‘the pill' (oral contraceptive) plus a barrier method (condom or diaphragm). You should carefully follow all the directions for the use of these methods of contraception.
Your doctor or your local family planning Clinic can provide you with more information about contraception. You will need a prescription for ‘the pill', which can be provided by your doctor or local family planning Clinic.
WheN CaN i stoP BeiNg so Careful?
two years after the end of your novatretin treatment the risk of birth defects is no greater than normal. should you wish to become pregnant, you can do so two years after you have stopped taking novatretin.
Where CaN i get More helP aND iNforMatioN ?
for further information about contraception contact your family doctor or your local family planning Clinic.
seCtIon 04
WhY are there siDe effeCts With NovatretiN ?
all medicines have side effects. With novatretin the side effects are closely linked to novatretin actually working. the side effects relate to its effect on the skin condition, as it reduces scaling and abnormal overgrowth of skin cells. If you are experiencing side effects, tell your doctor about the side effects you are experiencing; the dose of novatretin may need to be adjusted but this will depend on how well it is working on your condition. the side effects of novatretin can range from mild to severe. most of the side effects can be kept under control.
Who Will get siDe effeCts?
everyone! on the bright side, they can be kept under control with good skin care. some advice on how to control the side effects that happen while you are using novatretin can be found in the skin Care section of this booklet. the intensity of the side effects will vary from patient to patient. most of the common side effects are not very bad. It is important for you to be aware of the side effects that may occur while you are taking novatretin. It is also important for you to remember that you will not get all of the side effects mentioned in this section; you may only get one or two mild side effects. If you get side effects while taking novatretin you may find that they wear off with time.
What are the CoMMoN siDe effeCts?
You may start to get some side effects with novatretin before your condition starts to clear. You may also notice your condition starts to get worse at first. If this continues for more than 7 to 10 days, let your doctor know. the dose may need adjusting and/or treatments may be necessary.
dryness of the skin is the most common side effect with novatretin. novatretin may dry up some of the oil in your skin. You may find that your skin will become softer and more fragile. some skin loss on palms and soles of the feet may occur. Your face may look redder than usual and your skin may start to peel. usually any discomfort will settle with the use of a moisturizer but it may be needed several times daily. You may find that your lips become dry and cracked. While you are taking novatretin you will find that your skin is more sensitive to the sun. You will need to take extra care to avoid sunburn by wearing covering clothing and using sunscreens. It is important to look after your skin, the instructions in the skin Care section of this booklet will help you keep the side effects under control. a less common side effect of novatretin treatment is drying of the inside of the nose and dry eyes. drying of the nose can be uncomfortable and can lead to nose bleeds. there are ways to prevent and manage this. these are explained in the skin Care section of this booklet. dry eyes can be a problem for people who wear contact lenses or people who work in air conditioned areas. You may find that you need to use eye-drops to keep your eyes moist. You may also find that you cannot wear your contact lenses for as long as you did before starting on novatretin.
some people can suffer from some hair loss. hair loss is usually gradual. reducing the dose or stopping the medicine usually prevents further hair loss and hair should then begin to regrow as normal.
What are the other siDe effeCts?
most patients will not experience the side effects listed in this section, these side effects are not very common but can be serious. the side effects seen with novatretin treatment should disappear soon after you have stopped taking novatretin. there have been reports of people taking novatretin finding that their joints and muscles feel tender and stiff. this can be a problem if you are intending to do a lot of heavy exercise while taking novatretin. It is a good idea to discuss this with your doctor.
other serious but rarely experienced side effects of novatretin include skin infections especially around fingernails and toenails, bleeding and inflammation of the gums, headaches, blurred vision, dizziness, weight loss, diarrhoea and an abnormal menstrual cycle. You should immediately tell your doctor if you feel that the medication is making you unhappy or depressed.
It is important to remember that the side effects seen with novatretin treatment are reversible. they should disappear soon after you have stopped taking novatretin.
the only side effect that is not reversible are the birth defects that can be caused if you become pregnant while taking novatretin. there is detailed information about how and why you must prevent pregnancy while taking novatretin in the Contraception section of this booklet.
What is iMPortaNt for Me to tell MY DoCtor?
It is important for you to make sure that you tell your doctor: If you think you might be pregnant or you need contraceptive advice.
If you can't tolerate the side effects while taking novatretin. Your dose of novatretin may need to be changed.
If you get any of the serious less common side effects mentioned in the section: ‘What are the other side effects?' WheN Will the siDe effeCts go aWaY?
side effects will reduce when your dose of novatretin is lowered and should go away when you stop taking novatretin.
Where CaN i get More helP aND iNforMatioN ?
If you have any questions about the side effects that you have, or will get while you are on novatretin, you can talk to your doctor or call douglas pharmaceuticals Ltd (the people who make novatretin) on their toll free number 0508 672 826.
for even more information on your condition visit our website at www.novatretin.com or the dermatological website www.dermnet.org.nz seCtIon 05
CarInG for Your sKIn WhY Do i NeeD sPeCial skiN Care?
While you are taking novatretin you will have to take a little extra care of your skin as novatretin will make your skin drier and more fragile. the information in this section will help you to look after your skin and keep the side effects of novatretin under control. It is a good idea to follow the skin care advice given in this section even before you start to notice any of the side effects related to novatretin. prevention is always better than cure.
What Not to Do While takiNg NovatretiN
It is important to follow this list of things not to do so that your skin remains in good condition.
do not remove any scaly or peeling skin. since your skin is fragile you can damage your skin by trying to remove scaly and peeling skin, this could lead to skin infections.
do not have facials. Because your skin is fragile the potentially harsh treatments involved in a facial can cause damage to your skin.
do not have waxes. Waxing while your skin is fragile can actually remove skin as well as hair! do not use other medication. novatretin is a strong medication and you should not use any other medication unless your doctor has specifically told you to do so.
do not have any part of your body pierced. there can be a serious risk of infection of any new piercing while you are on novatretin.
do not have electrolysis. Because your skin is fragile, electrolysis has the potential to damage your skin.
do not use hair colouring containing peroxide and do not have a perm or use hair rollers. If you want to get your hair permed it is best to do so at least two weeks before you start taking your novatretin. While you are taking novatretin your scalp will be more sensitive and your hair will be more fragile. Because of this it is important to avoid harsh hair treatments such as colours and perms.
do not use solariums and sunbeds. solariums and sunbeds can burn your skin just like the sun, your skin is more sensitive to the sun while you are taking novatretin and it is also too sensitive to use a solarium and sun bed.
do not have overly hot showers. Very hot showers can irritate your skin.
What CaN i Do to ease the siDe effeCts?
the most common side effect of novatretin, dryness, is relatively easy to treat. the following section contains a list of products that can be used to relieve dryness. If you notice anything unusual about your skin or anything that concerns you, talk to your doctor or pharmacist about it. It is a good idea to write down anything you notice or any questions you have for your doctor. the notes section at the end of this booklet is a good place to do this.
What ProDuCts CaN i use to ease the siDe effeCts?
Dry Skindry skin is the most common side effect of novatretin treatment. You can expect your skin to become drier all over your body. to help protect your skin it is best to keep your showers shorter than two minutes if possible and use luke warm water rather than hot water.
Face Cleansersthese cleansers are designed for use on the face. You should only use cleansers that are intended for use on sensitive skin. products you could try are: Innoxa sensitivity Gentle Cleansing milk, Cetaphil Lotion and avene extremely Gentle Cleanser.
Body CleansersBody cleansers should not be used on the face, unless they are also included in the face Cleansers section. It is better for your skin if you try to avoid soaps and use one of the cleansers listed in this section. products you could try are: QV Bath oil, QV Bar, QV Wash, neutrogena extra Gentle Cleanser, hamiltons mild foam Wash and dove soap.
Face Moisturisersusing a moisturiser on your face regularly will help keep the dryness that may be seen with novatretin treatment under control. the best type of moisturiser is one designed for sensitive skin. products you could try are: QV Lotion and avene skin recovery Cream.
Body Moisturisersto keep your skin in good condition you should use a moisturising lotion on your whole body. even if you don't seem to have any dryness, prevention is always better than cure. for extremely dry areas use a cream, rather than a lotion. products you could try are: QV skin Lotion, QV Cream, hydraderm Lotion, Vaseline Intensive Care Lotion, hamilton dry skin treatment.
Dry lipsYour lips are particularly sensitive to the drying effects of novatretin. this makes it important to look after them well. this can be achieved very simply by applying a lip balm regularly. By applying a lip balm every one to two hours you can prevent your lips from becoming dry and cracked. make sure you also pay attention to the corners of your mouth, this area is prone to cracking. a lip balm that contains a sunscreen is best. You should carry a tube of lip balm with you during the day. You should see your local doctor if your lips become very cracked or begin bleeding.
products you could try are: QV Lip Balm, Vaseline Lip therapy, Lip sed, Blistex, hamilton Lipz Lip ointment and avene Lip Balm with Cold Cream.
Dry Nosethe inside of your nose can also become dry while you are taking novatretin. If this becomes severe it can result in nosebleeds. to keep the inside of your nose moist you should apply a small amount of petroleum jelly a few times a day using a cotton bud. If you suffer from persistent nose bleeds or your nose bleeds are difficult to stop, you will need to see your pharmacist or your doctor. severe nose bleeds can be treated with prescription products.
Dry EyesIf you find that your eyes feel dry or sore then you may need to use eye-drops to keep them moist. dry eyes can be a particular problem for people who wear contact lenses or people who work in air-conditioned areas. If you wear contact lenses you may find that you cannot wear your contact lenses for as long as you did before starting on novatretin. for dry eyes, products you could try are (if you wear contact lenses check with your optometrist to make sure that these products are suitable): allergan tears plus, allergan Liquifilm tears, alcon tears naturale, alcon poly-tears, alcon Bion tears and allergan Lacri-Lube ointment (this is an overnight eye moisturising ointment) and Vismed Lubricant eye-drops.
Sun Carenovatretin will make your skin more sensitive to the sun. You will need to make sure that you are well protected from the sun. You should not sunbathe, even with a sunscreen, or use a solarium. the best way to do this is to cover up as much as possible, wear a hat with a brim and wear a sunscreen, preferably one with a 30+ sun protection factor. the best sunscreens are oil free and alcohol free.
products you could try are: sunsense sport sunscreen spf 30+, sunsense daily face matt sunscreen spf 30+, aquasun spf 30+ and avene Very high protective sunscreen spf30+, hamilton sunscreen milk spf 30+ and hamilton everyday face sunscreen spf 30+.
Dry Hair and DandruffIf you find that your scalp and hair are drier than usual you may need to use a mild shampoo designed for dry hair. You should use a conditioner to help protect your hair and scalp. You should avoid using hair dyes, especially dyes containing peroxide, as they may make your hair and scalp drier and can cause irritation.
If dandruff becomes a problem you should use a medicated antidandruff shampoo. You could try the following shampoo products for dry hair and dandruff: Ketoconazole shampoo, dermaVeen oatmeal shampoo, Johnson's Baby shampoo, Galderma Ionil-t shampoo, and ducray extra Gentle shampoo.
Dry VaginaYou may find that your vagina is dry and this may cause pain during sexual intercourse. You can use dp Lubricating Gel or K-Y Jelly to help relieve this problem.
Dry AnusYou may experience some dryness and irritation around the anus. You can help relieve and reduce this problem by applying petroleum jelly several times a day.
Cosmeticsmakeup can sometimes aggravate your condition but if you choose your products carefully you can still wear makeup if you want to.
Powdersmost powders are suitable for use while taking novatretin.
Lipsticksall lipsticks are suitable for use while taking novatretin. the best lipsticks to use are those that contain sunscreens. It is also a good idea to wear a lip balm under your lipstick, because this will provide better protection for your lips.
Lip Balmsa lip balm that contains a sunscreen is best. You should carry a tube of lip balm with you during the day. products you could try are: QV Lip Balm, Vaseline Lip therapy, Lip sed, Blistex, hamilton Lipz Lip ointment and avene Lip Balm with Cold Cream.
seCtIon 06
heLpInG Your psorIasIs
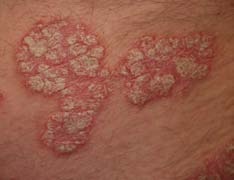
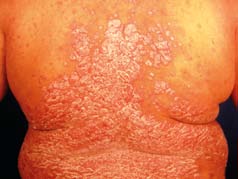
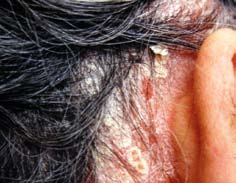
What is Psoriasis?
psoriasis is a common, chronic, scaly rash that affects people of all ages (about 2% of the population). there is a genetic predisposition to psoriasis i.e. it tends to run in families. psoriasis is also influenced by many environmental factors. It is not contagious and is not due to an allergy.
the most common ages for psoriasis to first appear are in the late teens and in the 50s. It affects men and women equally, although in children, girls are more commonly affected than boys.
psoriasis is often so mild it is barely noticed by the affected person, but it can occasionally be so severe the patient must be admitted to hospital for treatment. It may or may not be itchy.
What Does Psoriasis look like?
psoriasis is characterised by red, scaly patches of skin, which usually have very well defined edges. It is often symmetrical, affecting both sides of the body. the scale is typically silvery white. this typical scale may not be so obvious if the psoriasis affects a body fold such as the armpit or the patient is using emollients regularly. then it is more likely to be smooth and shiny.
psoriasis is often very minor, causing a few dry patches on the backs of the elbows and knees, some irritation in the umbilicus (belly button) and natal cleft (between the buttocks) or scaling in the scalp. It can, however, affect any area of skin and it may be severe or unusual in appearance.
What Causes Psoriasis?
exactly what causes psoriasis is not fully understood but there is a lot of active research into this area. the immune system is involved and appears to be overactive in a way that causes inflammation. specifically, there is excessive production of cell growth compounds. these have many effects, including growth of extra blood vessels within the skin (causing the red colour) and increased turnover of the skin cells (causing the scaling and thickening of the skin).
Genetic influences Like many diseases, psoriasis is influenced by inherited characteristics. up to 50% of people with psoriasis will know of another affected family member. patients with a family history of psoriasis tend to develop psoriasis earlier in life than those without a family history.
Stress physical and emotional stress may precipitate psoriasis and are hard to avoid.
Infection Infections may cause flares of psoriasis. sometimes, treatment of the infection may result in clearing or improvement of the psoriasis.
streptococcal throat infections (tonsillitis) may cause guttate psoriasis.
Candida infections (thrush) may aggravate flexural psoriasis.
malassezia yeasts may have a role in sebopsoriasis.
Injury psoriasis localises around the site of physical, chemical, electrical, infective and inflammatory injury as it heals (the Koebner phenomenon). Less often, psoriasis may localise to old scars.
Hormones the relationship of hormones to psoriasis is unclear. post-puberty is a peak time for the onset of psoriasis. pregnancy may also have an effect on the severity of the psoriasis; it usually improves with the potential for worsening after the birth of the baby, but the reverse can occur. psoriasis does not affect the unborn baby.
Medications several medications can precipitate or aggravate psoriasis:
Beta blockers (used to treat high blood pressure)
anti-malarials e.g. hydroxychloroquine
nonsteroidal anti-inflammatory drugs (nsaIds)
stopping oral corticosteroids
stopping strong topical corticosteroids.
Sun and UV Light
ultraviolet light can precipitate or aggravate psoriasis.
sunlight is usually beneficial for psoriasis (except in sun sensitive / photosensitive psoriasis).
Obesity many psoriasis studies have noted many affected patients to be overweight or obese. recently, it has become clear that the severity of psoriasis is correlated with insulin resistance, a feature of metabolic syndrome. psoriasis is associated with a greater risk of atherosclerosis resulting in ischaemic heart disease (angina and heart attack), stroke and peripheral vascular disease.
Alcohol and smoking there is an association between increased alcohol intake and smoking and the development of severe psoriasis. however, whether this is a cause, or effect, is not known.
is there a Cure?
there is to date no cure for psoriasis but satisfactory control of the disease is possible for most patients.
some people have a single episode of psoriasis that clears after a few months and never recurs, quite likely after acute guttate psoriasis. most other forms of psoriasis run a fluctuating course with periods of marked improvement and even complete clearance, only to relapse at a later time. there may be several years between relapses. a small group of patients have severe, persistent psoriasis that is very difficult to treat and can be very disabling.
1. Topical therapiestreatments that are applied directly to the skin are known as topical therapies. they include creams, ointments, pastes and lotions. If your psoriasis is mild, topical therapies will be the mainstay of your treatment and include the following:
emollients. emollients reduce scaling and can be used as often as needed.
salicylic acid. preparations containing salicylic acid can help heavily scaled plaques.
topical steroids. Weaker steroids often do not work very well on thick patches of psoriasis, but
may do better on the face or in the skin folds. the stronger ones have possible side effects, one
of which is to make your skin thinner. Your doctor will monitor their use closely. psoriasis
sometimes comes back quickly when topical steroid treatment stops.
tar preparations. taking a medicated tar bath may help to remove loose scales. tar creams or
ointments help most patients but may be messy and can stain clothing.
vitamin D analogues. there are vitamin d preparations used to treat psoriasis. these are safe,
clean to use and do not stain the skin. treatment is applied twice daily and can go on for as
long as required. Irritation may occur, especially on the face, buttocks and genitals, and these
treatments should be applied to those areas only on the specific instructions of your doctor.
2. Phototherapy this term refers to treatment with various forms of ultraviolet light, sometimes assisted by taking particular tablets. It is helpful if the psoriasis is extensive, or fails to clear with topical treatment, or comes back quickly after seeming to clear. topical therapy will usually continue during the phototherapy.
two types of ultraviolet (uV) light may be given, using special machines: uVa and uVB. these are different parts of normal sunlight. treatment with uVa is helped by taking a medication known as a psoralen – a combination known as puVa therapy. treatment with uVB does not need tablets.
3. Oral and Injected Treatmentsthe idea of using a tablet to treat psoriasis is attractive, but the effective ones all have potential risks, so they are not used for psoriasis if it can be kept under control in simpler ways. In addition, you will usually have to continue with some topical therapy even though you are taking the tablets.
Your dermatologist will discuss the risks with you if you start on this kind of treatment. all of the tablets may require blood tests, and many interfere with other medicines. female patients should not become pregnant whilst on any tablets for psoriasis, and with some of them it is important that male patients should not father a child.
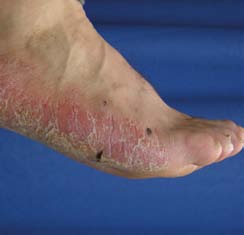
other than novatretin, the tablets in question include ciclosporin (suppresses the immune system), methotrexate (slows down the rate at which the skin cells are dividing in psoriasis), and hydroxycarbamide (formerly known as hydroxyurea – also slows down the rate at which the skin cells are dividing).
there are also several injectable forms of treatment known as "Biologicals" available for extremely severe forms of psoriasis.
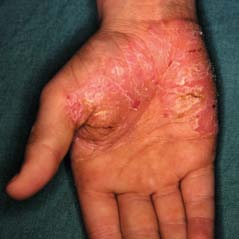
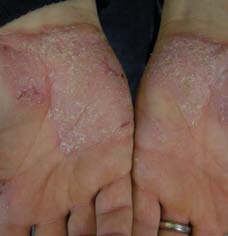
Psoriasis of the PalMs aND soles
psoriasis may predominantly affect the palms and soles in various ways:
typical scaly, red patches similar to psoriasis elsewhere
Generalised thickening and scaling of the palms and soles (keratoderma)
sheets of tiny yellow-brown pustules (palmoplantar pustulosis).
Clinical features
palms and soles affected by psoriasis tend to be partially or completely red, dry and thickened,
often with deep painful cracks (fissures). It can be quite hard to differentiate from hand
dermatitis and other forms of keratoderma, but signs of psoriasis elsewhere may help make a
diagnosis.
palmoplantar pustulosis is considered a distinct entity in which there are clusters of pustules on the palms and/or soles, but about 10-20% of those affected have psoriasis on other sites of the body.
palmoplantar psoriasis tends to be a chronic recurrent condition.
treatment
mild psoriasis of the palms and soles may be treated with topical treatments:
emollients: thick, greasy barrier creams applied thinly and frequently to moisturise the dry, scaly skin and help prevent painful cracking.
Keratolytic agents such as urea or salicylic acid to thin down thick scaling skin. several companies market effective heel balms containing these agents.
Coal tar: to improve the scale and inflammation. Because of the mess, coal tar is often applied at night under cotton gloves.
topical steroids: ultrapotent ointment applied initially daily for two to four weeks, if necessary under occlusion, to reduce inflammation, itch and scaling. maintenance use should be confined to 2 days each week (weekend pulses) to avoid thinning the skin and causing the psoriasis to become more extensive.
Calcipotriol ointment is not very successful for palmoplantar psoriasis and may cause an irritant dermatitis on the face if a treated area inadvertently touches it. dithranol is too messy for routine use on hands and feet.
more severe palmoplantar psoriasis usually requires phototherapy or systemic agents, most often:
Biologics are also sometimes prescribed for severe palmoplantar psoriasis.


reCoMMeNDeD ego ProDuCts
egoPsoryl ta
Contains (w/w): Coal tar 5%, phenol 0.5%,
sulphur 0.5% in an alcohol gel base.
Benefits: egopsoryl ta helps provide effective
relief from intense itching.
sebitar +
sebitar – Contains (w/w): pine tar 1%, Coal tar
solution 1%, salicylic acid 2%. Benefits: Gentle
formula that relieves itch and inflammation.
aids in the relief of eczema and psoriasis of the
scalp.
sebirinse – Benefits: Conditions the hair,
preventing tangles and dryness. removes any
odours remaining after sebitar treatment.
Pinetarsol
Contains (w/w): Pinetarsol gel – pine tar 1.6%
Pinetarsol – pine tar 2.3%, triethanolamine
lauryl sulfate 6%.
Pinetarsol Bath oil – pine tar 2.3% in an
emollient base.
Pinetarsol Bar – pine tar 1% with a blend of
mild surfactants.
Benefits: help to relieve dry, itchy, inflamed
Contains (w/w): egoderm Cream – Ichthammol
1% in an emollient cream base.
egoderm ointment – Ichthammol 1%, Zinc
oxide 15% in a soft paraffin base.
Benefits: reduces inflammation and relieves
irritation.
Dermaid 1%
Contains (w/w): Dermaid 1% (pharmacist
medicine) – hydrocortisone 1% (dissolved).
Dermaid 0.5% (pharmacy medicine) –
0.5% Cream
hydrocortisone 0.5% (dissolved). Benefits: for
temporary relief of minor skin irritations.
dissolved hydrocortisone for rapid penetration.
Dermaid soft
Contains (w/w): Dermaid soft 1% (pharmacist
1% Cream or
medicine) – hydrocortisone 1% (dispersed).
Dermaid soft
Dermaid soft 0.5% (pharmacy medicine)–
0.5% Cream
hydrocortisone 0.5% (dispersed). Benefits: for
temporary relief of minor skin irritations.
dispersed hydrocortisone for slow penetration.
seCtIon 07
treatInG darIer's dIsease
darier disease is also known as ‘keratosis follicularis'. It is a genetic disorder that causes skin changes. onset of skin changes is usually in adolescence and the disease is usually long term. It is inherited in an autosomal dominant pattern, which means that a single gene passed from one parent causes the condition. the chance of a child inheriting the abnormal gene if one parent is affected is 1 in 2 (50%) but not all people with the abnormal gene will develop symptoms of the disease.
hoW is it DiagNoseD?
usually darier disease is diagnosed by its appearance and the family history, but it is often mistaken for other skin problems.
the symptoms and signs of darier disease vary between individuals. some have very subtle signs that are found only on careful inspection. others have extensive lesions. In an affected person the severity of the disease can fluctuate over time.
skiN rash
the skin lesions are greasy, scaly papules (small bumps) which tend to occur over the oily areas of the face (scalp margins, forehead, ears, around the nostrils and sides of nose, eyebrows, and beard area), neck, and central chest and back. the flexures (within natural folds of the skin around joints such as armpits and groins) and skin under breasts and between buttocks are also commonly affected. the papules have a firm, harsh feel like coarse sandpaper and may be skin-coloured, yellow-brown or brown in colour. If several of the small papules grow together they may form larger warty lesions which can become quite smelly within skin folds. the scalp is often affected with a heavily crusted rash which can be similar to seborrhoeic dermatitis but is usually harsher to the touch.
other presentations of this disease are common. some patients may have flat, freckle-like lesions. others may have very large, raised, warty lesions. Cystic acne may occur.
lesioNs affeCtiNg the MuCous MeMBraNes
mucous membranes are the red, moist linings of all body surfaces except the skin (eg. mouth, oesophagus, rectum, vulva, vagina). patients with darier disease may uncommonly have a white cobblestone pattern or small papules affecting the mucous membranes. overgrowth of the gums is also seen.
most patients will develop signs of the disease (even if subtle) before the age of 30 years. many patients will have a mild form of the disease that, although present, will go unnoticed
throughout life. patients with more severe disease will notice a chronic relapsing-remitting pattern to their signs and symptoms although cases of spontaneous resolution of signs have been reported. the rash is often exacerbated by sunlight (a reaction which may be delayed eg. on return from holiday), and occasionally by steroid use (although this may be useful for other patients). Bacterial infection can cause flares. Widespread infection of the skin with the herpes simplex (coldsore) virus is a well recognised complication. this can cause a severe flare and patients can feel quite unwell.
In most patients general health remains good regardless of the severity of the disease.
treatment is required only if there are troublesome symptoms. for patients with mild disease simple moisturisers, sun protection and selection of the right clothing to avoid heat and sweating are usually sufficient.
dermabrasion (sanding off the surface of the skin) may be effective in localised disease. Localised darier disease may also be treated successfully with topical retinoids. secondary bacterial infection (usually due to staphylococcus aureus) should be treated with antibiotics, and herpes simplex with antiviral agents.
If symptoms are particularly severe then a trial of an oral retinoid medication such as acitretin may be effective.
reCoMMeNDeD ego ProDuCts
Qv intensive Body
Qv intensive Moisturising
Qv Bath oil
non-greasy, soap free bath
Water-free, highly emollient
suitable for dry, itchy skin.
oil. suitable for dry or
moisturiser that won't sting
Leaves a protective,
sensitive skin and suitable
inflamed or cracked skin.
moisturising film on the
for infants.
preservative free.
skin. suitable for extremely dry skin. preservative free.
Qv intensive Moisturising
Qv flare up Bath oil
this rich protective cream is
dual action formula reduces
ideal for very dry areas of
suitable for dry, itchy skin.
the level of bacteria and
Leaves a protective,
helps prevent moisture loss.
moisturising film on the
Calms irritated skin and
skin. suitable for extremely
reduces roughness and
dry skin. preservative free.
sunsense
Benefits: a very high spf broad spectrum
sensitive or
sunscreen for highly sensitive skin. for people
sunsense
who cannot use regular sunscreens. fragrance
sensitive
and chemical absorber free.
sunsense
Benefits: a very high spf broad spectrum
ultra Milk
sunscreen for general use. Water resistant for 4 hours. fragrance free.
sunsense
Benefits: a very high spf broad spectrum
sport Milk
milk for active / sports people. non-greasy, water-resistant for up to 4 hours.
sunsense
Benefits: a very high spf broad spectrum
sunscreen formulated for the face and neck.
Ideal for daily use, helps prevent dryness and sun-induced damage. fragrance free.
sunsense
Benefits: a very high spf broad spectrum
Daily face
sunscreen for daily use. Contains a sheer tint for a matte finish to the skin. fragrance free.
sunsense lip
Benefits: a very high spf broad spectrum
sunscreen for the lips. helps protect lips from burning and drying. fragrance free.
seCtIon 08
manaGInG IChthYosIs
What is iChthYosis?
Ichthyosis is characterised by persistently dry, thickened, rough, fish scale skin. there are at least 20 varieties of ichthyosis, including inherited and acquired forms.
Ichthyosis vulgaris, accounts for 95% of all ichthyosis cases. Inheritance is autosomal dominant i.e. it is passed from a parent to about half their children. signs and symptoms of ichthyosis vulgaris usually become apparent within the first year of life.
acquired ichthyosis is not inherited and occurs for the first time in adulthood. It is usually associated with some general disease, such as underactive thyroid states, sarcoidosis, lymphoma, generalised cancer or hIV infection. It may be provoked by certain medications (such as kava, nicotinic acid and hydroxyurea).
What Causes iChthYosis?
Inherited forms of ichthyosis occur as a result of a genetic mutation. the mutated gene causes an abnormality in the normal lifecycle of skin. Whilst in most people, the growth, dying and shedding of skin happens unnoticed, people with ichthyosis reproduce new skin cells at a rate faster than they can shed it, or reproduce at a normal rate but the rate of shedding is too slow. either way there is a build up of dry scaly skin.
What are the sigNs aND sYMPtoMs of iChthYosis?
although the signs and symptoms may vary amongst the different types of ichthyosis, they all show the characteristic dry, rough, scaly skin. Key characteristics of the four main types of inherited ichthyosis are listed in the table below.
type of ichthyosis
Ichthyosis vulgaris
face and scalp. the bends of arms and legs usually spared. palms are excessively lined associated with atopic dermatitis
Lamellar ichthyosis
scaling occurs over the whole body, including creases and bends may result in drooping lower eyelids
skin is moist, red, and tender at birth
fluid filled blisters may occur which may become infected and give rise to a foul skin odour thick, generalized scaling occurs within a few days pathology shows epidermolytic hyperkeratosis
X-linked ichthyosis
may be associated with testicular disease
How common is ichthyosis and who gets it?apart from ichthyosis vulgaris all other forms of ichthyosis are rare. Ichthyosis vulgaris affects about 1:250 individuals. Ichthyosis occurs worldwide and affects people of all races.
What problems does ichthyosis cause?people with ichthyosis have a normal lifespan. however they may need to spend several hours each day caring for their skin so they can lead as much of a normal life as possible. at some point during their life people with severe ichthyosis may come up against some of the following problems:
overheating: ichthyosis may affect normal temperature control by reducing the ability to sweat
Limited movement: dry, scaly skin may make it too painful to move some parts of the body
secondary infection: cracking and splitting of the skin may lead to skin infections and sometimes systemic infections
Impaired hearing or eyesight: skin may build up over the ears or eyes
What treatment is available?there is no cure for ichthyosis. the main goal of treatment is to moisturise and exfoliate. this helps prevent dryness, scaling, cracking and build-up of skin.
people with ichthyosis need to bathe, moisturise and exfoliate their skin on a daily regular basis. Your dermatologist may prescribe or recommend moisturising creams and ointments to keep the condition under control. In severe cases they may prescribe oral retinoids such as acitretin or isotretinoin. this can help to reduce scaling. oral antibiotics may be prescribed if secondary infection occurs.
the following skin care tips may help:
apply lotions and creams to wet skin to trap in the moisture (within 3 minutes of showering/bathing)
rub gently a pumice stone on wet skin to help remove thickened crusty skin
Brush washed hair to remove scales from scalp
Lanolin creams and products containing urea, lactic acid and other alpha hydroxy acids may help to exfoliate and moisturise skin.
reCoMMeNDeD ego ProDuCts
Qv skin lotion
Qv Bath oil
Light moisturizing
a soap substitute
non-greasy, soap free
lotion to help prevent
body wash for daily
bath oil. suitable for
or relieve dry skin.
use on normal, dry or
dry or sensitive skin
and suitable for infants.
Qv gentle Wash
Qv Bath oil
this rich protective
a very gentle soap
non-greasy, soap free
cream is ideal for very
substitute for dry or
bath oil. suitable for
dry areas of skin.
sensitive skin.
dry or sensitive skin and suitable for infants.
Moderate
Qv intensive Body
Qv intensive
Qv Bath oil
non-greasy, soap free
Water-free, highly
bath oil. suitable for
emollient moisturiser
suitable for dry, itchy
dry or sensitive skin
that won't sting
and suitable for
inflamed or cracked
skin. preservative free.
moisturising film on the skin. suitable for extremely dry skin. preservative free.
Moderate
Qv intensive
Qv flare up Bath oil
this rich protective
dual action formula
cream is ideal for very
reduces the level of
dry areas of skin.
suitable for dry, itchy
bacteria and helps
prevent moisture loss.
Calms irritated skin
moisturising film on
the skin. suitable for
roughness and scaling.
extremely dry skin. preservative free.
Contains (w/w):
Pinetarsol gel –pine
tar 1.6%
Pinetarsol – pine tar
2.3%, triethanolamine
lauryl sulfate 6%.
Pinetarsol Bath oil –
pine tar 2.3% in an
emollient base.
Pinetarsol Bar – pine
tar 1% with a blend of
mild surfactants.
Benefits: help to
relieve dry, itchy,
inflamed skin.
egoderm Cream or
Contains (w/w):
egoderm Cream –
Ichthammol 1% in an
emollient cream base.
egoderm ointment –
Ichthammol 1%, Zinc
oxide 15% in a soft
paraffin base.
Benefits: reduces
inflammation and
relieves irritation.
seCtIon 09
manaGInG paLmopLantar
palmoplantar pustulosis is a chronic pustular condition affecting the palms and soles.
What is the cause of palmoplantar pustulosis?
the exact cause of palmoplantar pustulosis is unknown. It appears to be a disorder of the
eccrine sweat glands, which are most numerous on palms and soles.
palmoplantar pustulosis is probably autoimmune in origin (‘self allergy'), as there is an association with other autoimmune diseases particularly gluten sensitive enteropathy (celiac disease), thyroid disease and type 2 diabetes.
palmoplantar pustulosis was previously considered to be a localised form of pustular psoriasis but about 10-20% of patients with palmoplantar pustulosis have psoriasis elsewhere. It is now known that they are distinct conditions with different genetic backgrounds.
Genetic factors account for family members having the disease. however, it rarely occurs before adulthood. It is more common in women than men.
palmoplantar pustulosis is much more common in current smokers (and in those that have smoked in the past). It is thought that activated nicotine receptors in the sweat glands cause an inflammatory process.
dermatitis, particularly pompholyx, and tinea pedis (a fungus infection) may appear similar, but require different treatment.
Palmoplantar pustulosis
palmoplantar pustulosis presents as crops of sterile pustules occurring on one or both hands and/or feet. they are associated with thickened, scaly, red skin which easily develops painful cracks (fissures).
the condition varies in severity and may persist for many years. It is not known what causes exacerbations or remissions. palmoplantar pustulosis is not infectious to other people and does not influence one's general health. however the discomfort can be considerable, interfering with working and leisure activities.
Walking for prolonged periods may cause exacerbations on the feet. If the palms are involved, manual activities may be uncomfortable, and injuries may aggravate the disorder. Certain occupations are therefore inadvisable for affected individuals.
treatment does not cure the disorder and is not always successful. the following may be helpful.
If you smoke, try to stop: however, palmoplantar pustulosis may take several months to improve.
Choose comfortable footwear made from natural fibres.
avoid friction and minor injuries.
Cover deep fissures with a waterproof dressing.
rest the affected area.
If flares appear related to tonsillitis, consider tonsillectomy.
use plenty of grease or other thick emollient to soften the dry skin to prevent fissures.
soak in warm water with emulsifying ointment for 10 minutes.
apply white soft paraffin liberally
use salicylic acid ointment or urea cream (heel balm) to peel off dead skin (may sting).
Wash with bath oil or soap substitute.
topical steroids
topical steroids are anti-inflammatory agents which range in potency and vehicle. only the
strongest ointments are effective in conditions affecting the thick skin of the hands and feet.
however the very potent products such as clobetasol proprionate should be used only for
limited periods or else side effects and loss of efficacy become a problem.
a thin smear should be applied twice daily to the affected area. the effect may be enhanced by using plastic occlusion for a few hours or even overnight – use polythene gloves, plastic bags or cling film. do not use occlusion for more than 5 days in a row.
Coal tar
Crude coal tar is very messy but applied directly to the pustules every five days or so can stop
them occurring. paint on carefully and cover. It can be mixed in an ointment base for easier
application.
acitretin
novatretin capsules, derived from Vitamin a, can control palmoplantar pustulosis in the
majority of users.
Puva
ultraviolet radiation, especially in combination with psoralens taken as tablets or applied
topically (bathwater puVa), can be effective. puVa particularly in combination with novatretin
(re-puVa) can also be effective. Careful medical supervision is necessary to avoid burning.
other
a variety of other medications can help some subjects including:
tetracycline antibiotics
Biologics are occasionally effective when used for severe palmoplantar psoriasis.
What is keratoderma?‘Keratoderma' is a term that means marked thickening of the skin.
‘palmoplantar' refers to the skin on the soles of the feet and palms of the hands; these are the areas keratoderma affects most often. palmoplantar keratoderma is also sometimes known as ‘keratosis palmaris et plantaris'.
Classification of keratoderma depends on whether or not it is inherited, and its clinical features.
diffuse keratodermas affect most of the palms and soles.
focal keratodermas mainly affect pressure areas.
punctate-type keratodermas result in tiny bumps on the palms and soles.
most often the abnormal skin involves only the palms and soles (non-transgradient) but sometimes it extends on to the top of the hands and feet as well (transgradient).
In some rare forms of keratoderma, other organs in the body may be affected in addition to the skin, and the keratoderma can be a marker of this internal abnormality.
What causes palmoplantar keratoderma?Keratoderma may be inherited (hereditary) or, more commonly, acquired.
hereditary keratoderma: the condition runs in families and is passed down from one or both
parent(s) to their children
acquired keratoderma: the condition is not inherited and occurs as a result of a change in the
health or the environment of the affected person
the hereditary keratodermas are caused by a gene abnormality that results in abnormal skin protein (keratin). they may be inherited either by an autosomal dominant or autosomal recessive pattern.
autosomal dominant keratodermas are likely to occur in every generation of a family. If one parent is affected there is a 50% chance that each child will be affected.
autosomal recessive keratodermas occur less commonly within an affected family. this is because both parents need to pass on an abnormal gene to the child for it to be affected.
people with one affected gene only do not have the condition themselves but carry the abnormal gene and are referred to as ‘carriers' of the disease. they may pass on the abnormal gene to their children but the children will only be affected if their other parent also carries an abnormal gene and passes it on to the same child.
Treatment of palmoplantar keratodermathe following treatments soften the thickened skin and make it less noticeable.
Keratolytics (e.g. 6% salicylic acid in 70% propylene glycol)
topical retinoids
topical vitamin d ointment (calcipotriol)
systemic retinoids (acitretin)
reCoMMeNDeD ego ProDuCts
Qv gentle Wash
Qv Bath oil
this rich protective cream is
a very gentle soap
non-greasy, soap free bath
ideal for very dry areas of
substitute for dry or
oil. suitable for dry or
sensitive skin.
sensitive skin and suitable for infants.
Qv intensive Body
Qv intensive Moisturising
Qv Bath oil
non-greasy, soap free bath
Water-free, highly emollient
suitable for dry, itchy skin.
oil. suitable for dry or
moisturiser that won't sting
Leaves a protective,
sensitive skin and suitable
inflamed or cracked skin.
moisturising film on the
preservative free.
skin. suitable for extremely dry skin. preservative free.
Qv intensive Moisturising
Qv flare up Bath oil
dual action formula
suitable for dry, itchy skin.
reduces the level of
Leaves a protective,
bacteria and helps prevent
moisturising film on the
moisture loss. Calms
skin. suitable for extremely
irritated skin and reduces
dry skin. preservative free.
roughness and scaling.
Contains: sodium lactate, lactic
acid. Benefits: rehydrates and
visibly revives rough, dry and
Qv feet heel Balm
cracked heels. exfoliates dead, dry skin.
Dermaid 1% Cream or
Contains (w/w): Dermaid 1% –
Dermaid 0.5% Cream
hydrocortisone 1% (dissolved).
Dermaid 0.5% – hydrocortisone
0.5% (dissolved). Benefits: for
temporary relief of minor skin
irritations. dissolved
hydrocortisone for rapid
penetration.
Dermaid soft 1% Cream
Contains (w/w): Dermaid soft
or Dermaid soft 0.5%
1% – hydrocortisone 1%
(dispersed). Dermaid soft 0.5%
– hydrocortisone 0.5%
(dispersed). Benefits: for
temporary relief of minor skin
irritations. dispersed
hydrocortisone for slow
penetration.
seCtIon 10
Consumer medICIne
Do not use NOVATRETIN capsules if the packaging is torn or
Acitretin, 10 mg and 25 mg Capsules
shows signs of tampering. In such case, please return it to your
pharmacist or talk to your doctor.
What is in this leaflet
You must tell your doctor if:
This leaflet answers some of the common questions about
• You have allergies to any other medicines, foods, dyes or
NOVATRETIN capsules.
It does not contain all the information that is known about
• You have any other health problems or issues including:
NOVATRETIN. It does not take the place of talking to your doctor
diabetes, or family members with diabetes, liver disease,
or pharmacist.
high triglycerides or cholesterol levels in the blood, or
All medicines have risks and benefits. Your doctor has weighed
family members with a history of high blood triglycerides or
the risks of taking NOVATRETIN against the benefits they expect
cholesterol levels
it will have for you. If you have any concerns about taking
Taking other medicines
NOVATRETIN capsules, ask your doctor or pharmacist.
If you are on any other medicine, including medicine bought
Keep this leaflet with the medicine. You may need to read it
from a pharmacy, supermarket or health shop, you must tell
your doctor. Some medicines may interfere with NOVATRETIN.
These include: tetracycline antibiotics (such as Doxine®, Doxy®,
What are NOVATRETIN capsules used for
Achromycin® and Minomycin®), phenytoin, the "mini-pill",
The active ingredient in NOVATRETIN capsules is acitretin, which
a low-dose progestogen oral contraceptive, vitamin A, or
belongs to a group of medicines called retinoids. It is very
formulations that contain vitamin A.
similar to Vitamin A which is obtained from our diet and is vital
Your doctor or pharmacist has an entire list of medicines to
for the normal growth and development of the body, especially
be avoided while taking NOVATRETIN. If you have not told your
doctor about any of the above, tell her or him before starting
Psoriasis is a skin disease with thickened patches of red skin,
NOVATRETIN capsules. Take NOVATRETIN capsules exactly as
often with silvery scales. NOVATRETIN is used to treat severe
your doctor has prescribed to you.
psoriasis and other severe skin disorders. NOVATRETIN works
to return skin to normal when problems with the normal
Use in Children
development of the skin are present, as in the case of severe
NOVATRETIN capsules should only be taken by children where
psoriasis and some other skin disorders.
alternative therapy cannot be used.
You may have been prescribed NOVATRETIN by your doctor
for another reason. If you have any questions about why
How to take NOVATRETIN capsules
NOVATRETIN has been prescribed for you, ask your doctor.
Always take NOVATRETIN exactly as your doctor or pharmacist
NOVATRETIN is only accessible with a doctor's prescription.
tells you to. The directions given may differ from information
contained in this leaflet.
Before you use NOVATRETIN
How much to take
Do not take NOVATRETIN capsules if:
Take NOVATRETIN capsules exactly as your doctor has
• You are pregnant or you intend to become pregnant in the
prescribed to you. Your doctor will determine exactly how many
next 24 months. Any possibility that you may be pregnant
NOVATRETIN capsules to take each day for your condition. This
must be ruled out by both yourself and your doctor before
will be matched especially to your needs and your bodyweight
you start taking NOVATRETIN capsules. The result of a
and whether you develop any side effects.
pregnancy test must be negative when performed within
two weeks before beginning NOVATRETIN treatment.
The starting dose is usually either 25 mg (1 x 25 mg capsule) or
NOVATRETIN is highly teratogenic i.e. there is an extremely
30 mg (3 x 10 mg capsules) per day for 2 to 4 weeks. Your dose
high risk of having a baby that is severely deformed.
will probably then be adjusted by your doctor when it is known
This means you must use effective contraception for one
how you respond to NOVATRETIN capsules.
month before, during and 2 years after treatment with
The initial signs of improvement may be seen in the first week
but, more often, after 2 or 3 weeks. It may take 2 to 3 months
• You are breastfeeding. Breastfeeding must stop before
until the full effect is seen. Affected skin areas will either peel
NOVATRETIN treatment can start. Do not breastfeed while
off or steadily clear. Sometimes more redness or itching may
taking NOVATRETIN capsules.
be present at first, but this will normally improve as treatment
• You have had an allergic reaction to NOVATRETIN capsules,
Vitamin A, other retinoids or any ingredients listed in the
Ingredients section of this leaflet.
How to take it
• You are taking tetracycline antibiotics. These include
NOVATRETIN capsules should be swallowed whole with a glass of
Doxine®, Doxy®, Achromycin® and Minomycin®.
• You are taking vitamin A, or preparations that contain
When to take it
• You have severe kidney or liver disease or abnormally high
NOVATRETIN capsules should be taken once daily with meals or
levels of fat in your blood
with a glass of milk. Female patients should wait until the 2nd
• You are taking methotrexate.
or 3rd day of their menstrual period before starting NOVATRETIN
Do not use NOVATRETIN capsules after the expiry date printed
capsules. This helps to ensure that you are not pregnant before
on the pack. It may have no effect at all, or worse, an entirely
you start to take NOVATRETIN therapy.
unexpected effect if you take it after the expiry date.
How long to take NOVATRETIN
Things you must not do:
Continue taking NOVATRETIN capsules for as long as your doctor
• Do not stop taking NOVATRETIN capsules or change the dose
without first checking with your doctor.
If you forget to take NOVATRETIN take it as soon as you
• Do not let yourself run out of NOVATRETIN capsules over the
remember and then go back to taking it as you would normally.
weekend or on holidays.
However, if it is nearly time for your next dose, skip the dose
• Do not donate blood while taking NOVATRETIN capsules or
you missed and take your next dose when you are supposed to.
for at least 2 years after stopping treatment.
• Do not use the "mini-pill", a low-dose progestogen oral
You should not make up for missing the dose by doubling (two
contraceptive, as contraception during treatment.
doses at the same time) the next dose. If you are unsure what
• Do not give NOVATRETIN capsules to anyone else, even if
to do, consult your doctor or pharmacist.
their symptoms seem similar to yours.
If you have issues remembering your dose, consult your
• Do not use NOVATRETIN capsules to treat other complaints
pharmacist who can offer you some hints.
unless told to by your doctor.
• Do not take any other medicines whether they need a
In case of an overdose
prescription or not without first telling your doctor or
Immediately, telephone your doctor or the National Poisons and
Hazardous Chemicals Information Centre (0800 POISON – 0800
764 766) or go to the Accident and Emergency at your nearest
Things to be careful of
hospital immediately if you think that you or anyone else may
Normally NOVATRETIN capsules would not affect your ability to
have taken too much NOVATRETIN. Do this even if there are no
drive a car or operate machinery. However visual disturbances
signs of discomfit or poisoning. You may require urgent medical
may occur while taking NOVATRETIN capsules. Make sure you
know how you react to NOVATRETIN capsules before you drive
Currently, no information is available on the effects of overdose
a car, operate machinery or do anything else that might be
with NOVATRETIN. In spite of this, based on experience with
dangerous if your vision is altered.
excessive vitamin A and other drugs similar to NOVATRETIN,
Wearing contact lenses during treatment and shortly after
signs of overdosage may include transient headache, vomiting,
treatment with NOVATRETIN capsules may cause discomfort.
flushed face, dry skin and lips, pain in the stomach, dizziness
NOVATRETIN capsules cause dry eyes so an eye lubricant,
and unco-ordination. You should recover without any after
or artificial tears (available from your pharmacist) might be
effects but may need some tests to determine if your liver has
necessary. Otherwise you might need to compensate by wearing
been affected.
your glasses.
Please keep these telephone numbers handy. If you are unsure
Avoid excessive sun exposure, and always apply sunscreen while
about what to do, ask your doctor or pharmacist.
taking NOVATRETIN capsules. Your skin may be more prone to
sunburn while on NOVATRETIN.
While you are taking NOVATRETIN
(Things you must do:)
Side effects
Tell all doctors, dentists and pharmacists who are treating you
Tell your doctor or pharmacist as soon as possible if you do not
that you are on NOVATRETIN capsules. NOVATRETIN capsules can
feel well while taking NOVATRETIN capsules. NOVATRETIN helps
cause birth defects. This means that you must use strict birth
most people with skin conditions, however in addition to the
control for at least 1 month before you start NOVATRETIN, the
beneficial effects; it is possible that unwanted side effects will
whole time you are using NOVATRETIN capsules and for at least
occur in some people during treatment, even when it is used
2 years after you finish taking NOVATRETIN capsules.
as directed. All medicines have side effects. Sometimes they
NOVATRETIN treatment should be started on the second or third
are serious but most of the time they are not. You may require
day of your next normal menstrual period.
medical treatment if you get some of the side effects. Ask your
If you become pregnant while taking NOVATRETIN capsules, stop
doctor or pharmacist to answer any questions that you may
taking it immediately and inform your doctor. You must also tell
your doctor immediately if you become pregnant in the 2 years
If side effects occur, they may be:
following the end of treatment.
• Dryness of the lips, mouth, nose, eyes and skin. Either a
Inform your doctor if, for any reason, you have not taken
moisturiser or petroleum jelly can be used to soften the lining
this medicine exactly as prescribed. Otherwise, your doctor
of the nose, lips and the skin
may think this medicine was not effective and change your
• thinning or peeling of the skin that was not previously
affected (for example, hands and feet)
It is critical to keep all of your appointments with your doctor
• sticky skin may occur
so your progress with NOVATRETIN therapy can be monitored
• hair loss sometimes occurs (and in rare cases, has persisted)
regularly. Your doctor may ask you to do some blood, liver
function and other tests from time to time in order to check
your progress and pick up any unwanted side effects.
• "redness of the skin" or itchiness
Inform your doctor if you take vitamin supplements that contain
• flushing.
greater than 2500 IU of Vitamin A. If you are unsure about this,
please check with your doctor or pharmacist.
Consumption of alcohol should be avoided during treatment.
Alcohol intake should also be avoided for 2 months after
finishing treatment with NOVATRETIN.
These side effects will most likely stop after the dose of
NOVATRETIN is lowered or stopped. Tell your doctor if you have
What it looks like:
any of the following side effects and they worry you:
NOVATRETIN hard-gelatin capsules can be described as follows:
Unusually severe or persistent headaches
10 mg Capsules: Hard gelatin capsule containing a yellow
powder with a white to off-white body and a brown cap printed
in black with "A10" on the capsule body.
Tenderness or stiffness in your joints or muscles or bones
25 mg Capsules: Hard gelatin capsule containing a yellow
powder with a yellow to light yellow body and a brown cap
printed in black with "A25" on the capsule body.
Active ingredient – acitretin
Each 10 mg capsule contains 10 mg acitretin
Male breast enlargement
Each 25 mg capsule contains 25 mg acitretin
maltodextrin, sodium ascorbate, microcrystalline cellulose,
gelatin, sodium lauryl sulfate, purified water, black printing ink
and the colourants iron oxide black (E172), iron oxide red (E172),
Changes in hearing
iron oxide yellow (E172) and titanium dioxide.
Irregular menstrual bleeding
NOVATRETIN Capsules are available in packs of 100 capsules.
Sore mouth or inflammation of the gums Taste disturbances
These side effects are dose related and indicate that the dose of
Douglas Pharmaceuticals Ltd
NOVATRETIN needs to be adjusted.
Stop taking NOVATRETIN capsules and contact your doctor
immediately if you experience any of the following:
Nausea, Vomiting, Headache, Blurred vision or visual
Phone: (09) 835 0660
This is not an entire list of all possible side effects. Others
Date of preparation of this information was July 2011.
may arise in some people and there may be some side effects
not yet known. Tell your doctor if you have anything else that
is making you unwell. Other side effects not listed above may
occur in some people. Consult your doctor or pharmacist if
there is anything you do not understand in this list. Do not
be alarmed by this list of possible side effects. You may not
experience any of them.
After taking NOVATRETIN capsules
Keep your NOVATRETIN capsules in the blister pack until it is
time to take them. If you take the capsules out of the packaging
they may not keep well. Keep NOVATRETIN capsules in a cool dry
place where the temperature stays below 25°C. Do not keep the
capsules, or any other medicine, in a bathroom or near a sink.
Do not leave the capsules in the car or on window sills. Both
heat and dampness can destroy some medicines. Protect
NOVATRETIN capsules from light.
Keep NOVATRETIN where children cannot reach them. A good
place to store medicines is in a locked cupboard at least one-
and-a-half metres above the ground.
We would like to acknowledge The New Zealand Dermatological
If your doctor asks you to stop taking NOVATRETIN, or the
Society Inc. in preparation of this booklet and the provision
capsules have passed their expiry date, you should return
of photographs from Waikato District Health Board and the NZ
any remaining capsules at the end of your treatment to your
DermNet website.
CoNfirMatioN of reCeiPt of iNforMatioN
oN treatMeNt With NovatretiN® (acitretin)
female Patients
I understand that I must not be pregnant in order to start this medicine.
I understand that I must not become pregnant while being treated with novatretin and for two years after the end of novatretin treatment.
I understand the risks associated with becoming pregnant while on novatretin as explained by my dermatologist. I am aware that significant harm may be caused to my unborn baby should it be exposed to novatretin during pregnancy.
as a precaution I agree to undergo a pregnancy test if necessary and have my doctor confirm that I am not pregnant immediately before starting treatment with novatretin. I am aware that methods to avoid pregnancy are absolutely essential during my treatment on novatretin. the safest option is an oral contraceptive plus a barrier. If there is any risk that pregnancy may have occurred, I agree to consult my specialist or Gp to discuss the need for emergency contraception.
I agree to avoid the possibility of pregnancy for one month before commencing treatment with novatretin, during the whole period of treatment and for two years after completion of treatment. should I become pregnant, I agree to inform my doctor immediately.
all Patients
I understand that I must not give novatretin to any other person.
I understand that while novatretin may help my skin, it may cause a number of side effects that have been explained to me.
I confirm that I have been fully informed of the above by:
Patient or Guardian Signature:
Patient's Address:
Source: http://www.novatretin.com/download.cfm/getfile/3
Migraine patient handout
Migraine – More than a Headache Introduction Migraine is a common clinical problem characterized by episodic attacks of head pain and associated symptoms such as nausea, sensitivity to light, sound, or head movement. It is general y thought of as a headache problem, but it has become apparent in recent years that many patients suffer symptoms from migraine who do not have severe headaches as a dominant symptom. These patients may have a primary complaint of dizziness, of ear pain, of ear or head ful ness, "sinus" pressure, and even fluctuating hearing loss. Fortunately, treatment regimens long established for the treatment of "classic" migraine headaches are general y effective against these "atypical" symptoms of migraine. How Common is Migraine?
wimjournal.com
WIMJOURNAL, Volume No. 2, Issue No. 1, 2015 Nawab P. Jamadar et.al. ORIGINAL ARTICLE A Comparative study of Triamcinolone acetonide with Methylprednisolone sodium succinate in the management of chronic low back pain Nawab P. Jamadar1, Aditya V. Vazalwar2 and Basavraj S. Nagoba3 Professor & Head, Anaesthesia1, Resident of Anaesthesia2 and Assistant Dean (R & D)3